When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
CPAP: Continuous Positive Airway Pressure
- CPAP machines work by delivering pressurized air through a mask to keep the airway open during sleep, helping reduce apneas, snoring, and oxygen drops.
- Consistent use of CPAP significantly improves symptoms of obstructive sleep apnea (OSA), including daytime sleepiness, cognitive focus, and cardiovascular health.
- Proper mask fit, cleaning, and equipment maintenance are essential for comfort and effectiveness; addressing common side-effects early can improve therapy adherence.
People who are diagnosed with a sleep-related breathing disorder are often prescribed a treatment called positive airway pressure (PAP) therapy. Although there are multiple ways of delivering PAP therapy, continuous positive airway pressure (CPAP) is a common sleep apnea treatment.
Consistent use of a CPAP machine provides both short- and long-term benefits to people diagnosed with sleep apnea. Learn about using a CPAP machine, choosing the right machine for you, and tips to help you get the most out of CPAP therapy.

Exploring CPAP Machines — But Haven’t Been Tested Yet?
Start with our easy, at-home sleep test. It’s stress-free and effective. Get results within a few days.
What Is a CPAP Machine?
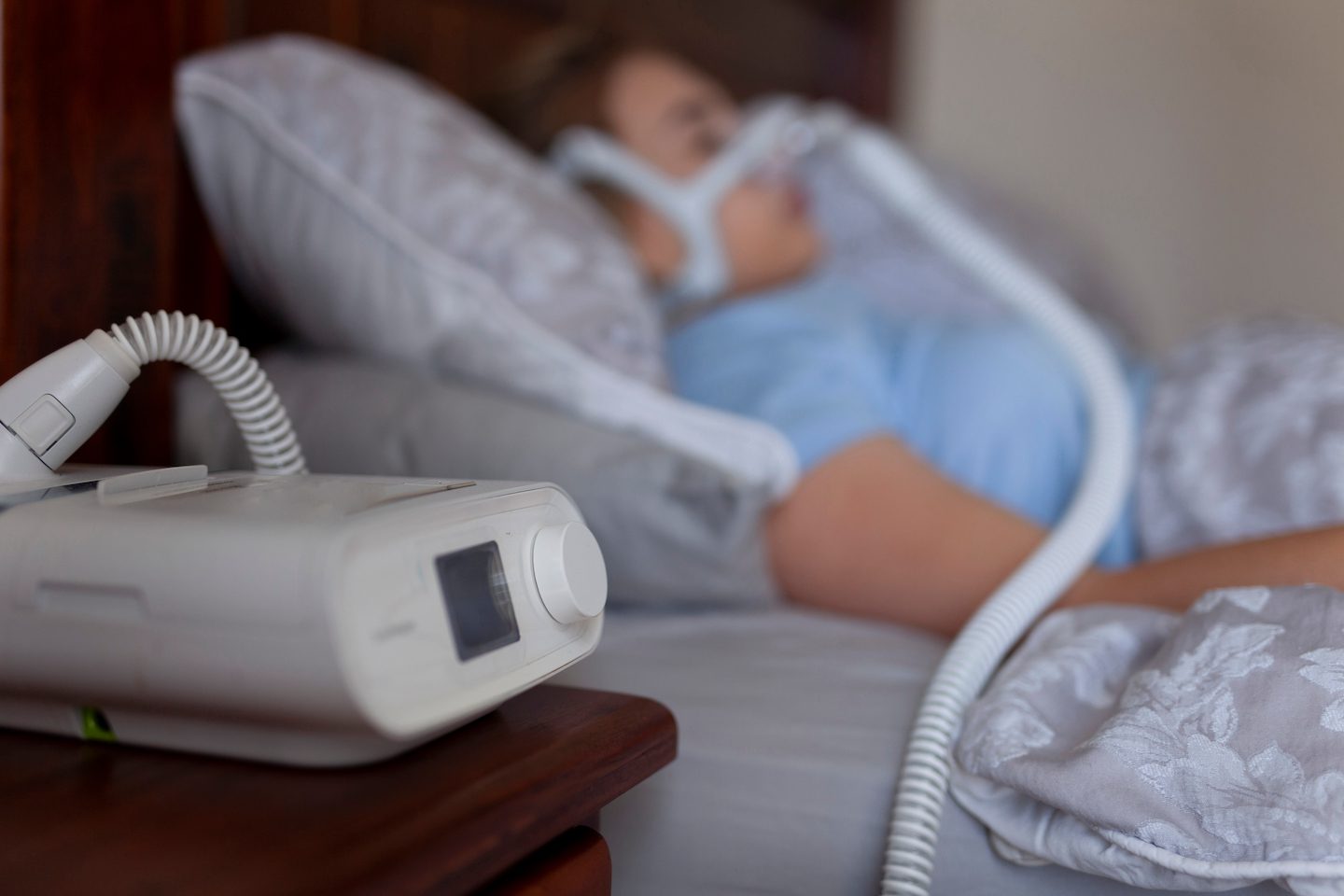
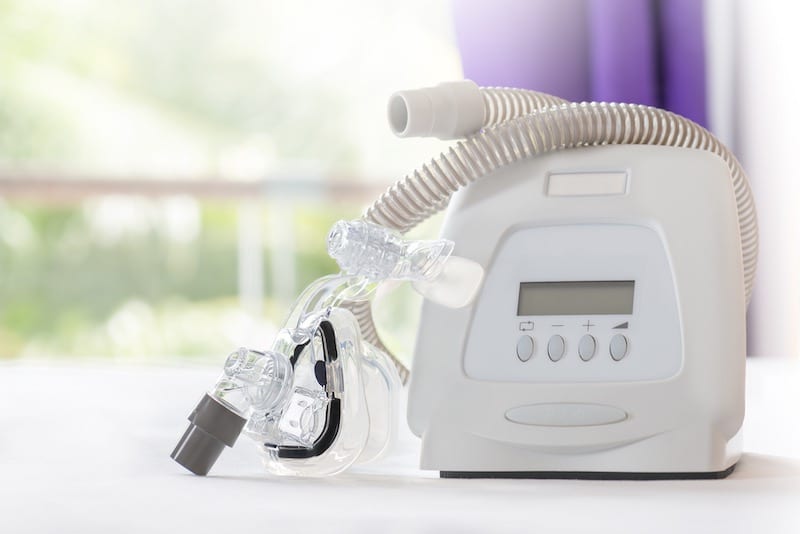
A CPAP machine is a bedside device that delivers positive airway pressure and is used to treat obstructive sleep apnea (OSA) and other breathing problems.
To help reduce periods of abnormal breathing in people with sleep apnea, a CPAP machine pushes air into a person’s airway, keeping it open as they sleep. As a result, sleepers treated with CPAP should experience fewer obstructive apneas and central apneas during sleep.
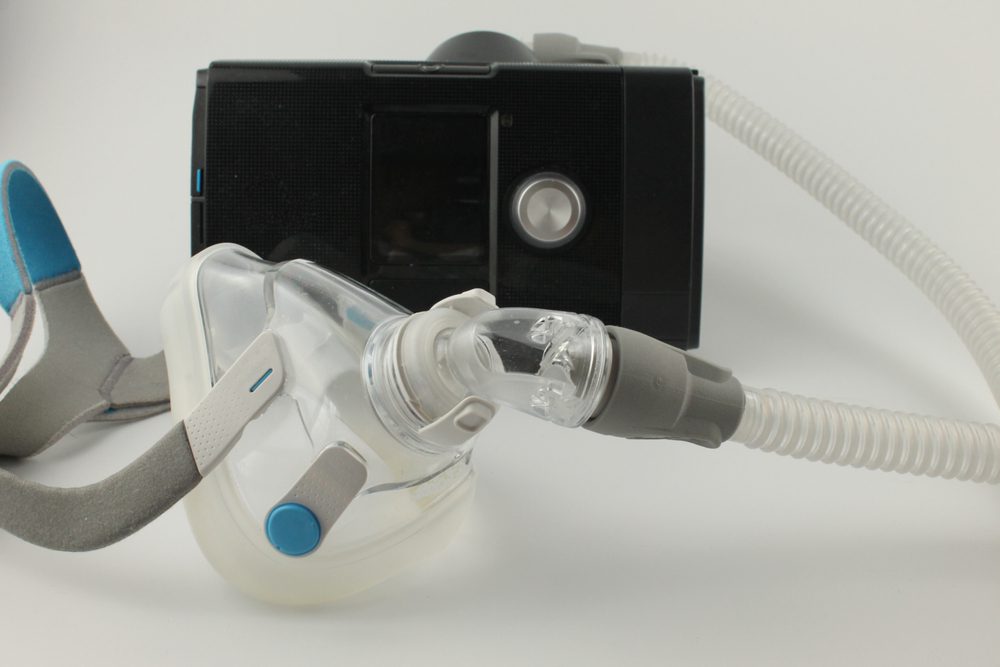
Parts of a CPAP Machine
Although CPAP machines can vary somewhat depending on the manufacturer, they generally contain these components:
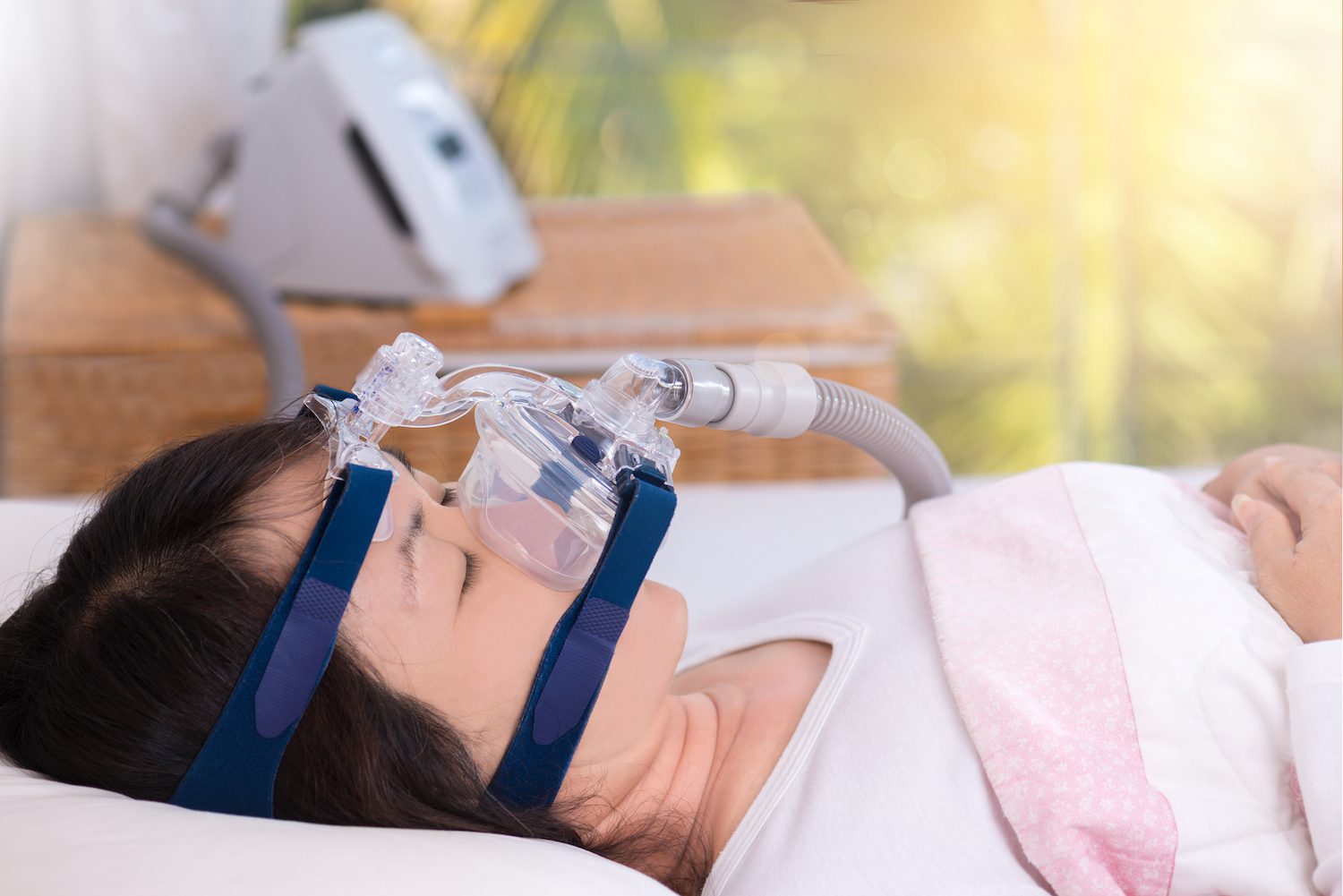
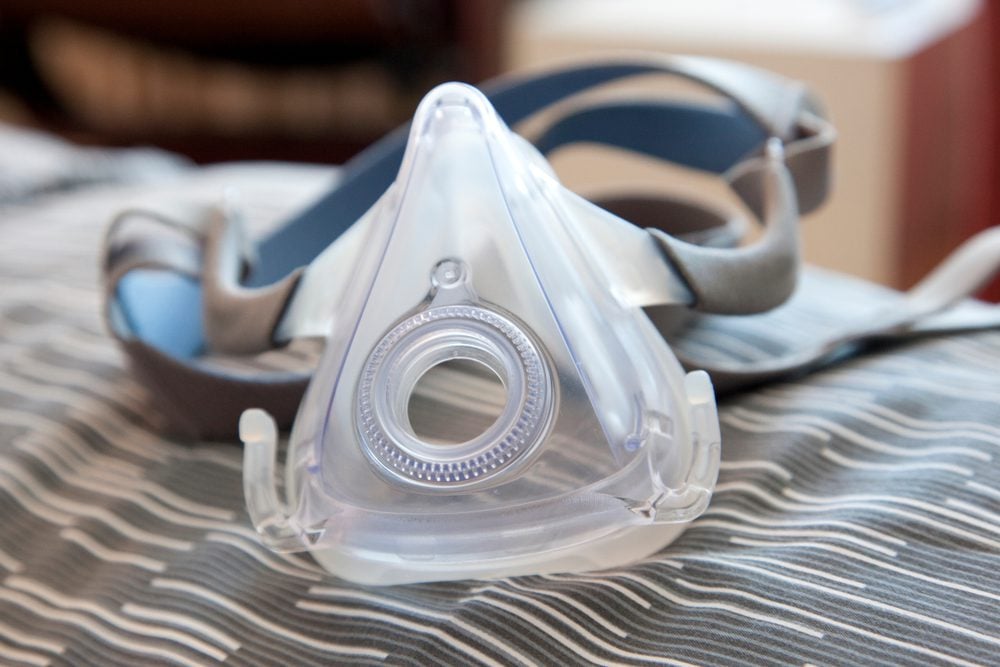
- Mask: A mask sits over the sleeper’s nose or both their nose and mouth, creating a seal so air can be pushed into the airway without escaping.
- Tubing: A plastic tube or hose connects the mask to the CPAP machine’s motor that pushes out air.
- Motor: The CPAP machine motor blows air into the connected tube.
- Filters: These trap dust, pollen, and other airborne particles before they enter your machine.
- Humidifier: Most CPAP machines include an integrated humidifier that adds moisture to the air from your CPAP machine to prevent dryness and irritation in your nose, mouth, and throat during sleep.
- Power source: Most machines must be plugged into an electrical outlet to power the motor, but some battery-operated CPAP machines are available.
Types of CPAP Machines
There are several types of CPAP machines designed to meet different breathing needs and comfort preferences:
- Standard CPAP: Delivers a fixed level of air pressure throughout the night. It’s the most common and often the first type prescribed for people with obstructive sleep apnea.
- Auto-Adjusting PAP (APAP): Automatically changes pressure levels based on your breathing patterns, providing more pressure when needed and less when you’re breathing normally.
- Bi-Level PAP (BiPAP): Uses two pressure settings—one for inhaling and one for exhaling—making it more comfortable for people who need higher pressures or have conditions like central sleep apnea or COPD.
- Travel CPAP: A compact, lightweight version of a standard or auto CPAP, ideal for frequent travelers or those with limited bedside space.
Types of CPAP Masks
CPAP masks designed for at-home use come in a variety of styles. A doctor can help choose the mask that offers the best fit.
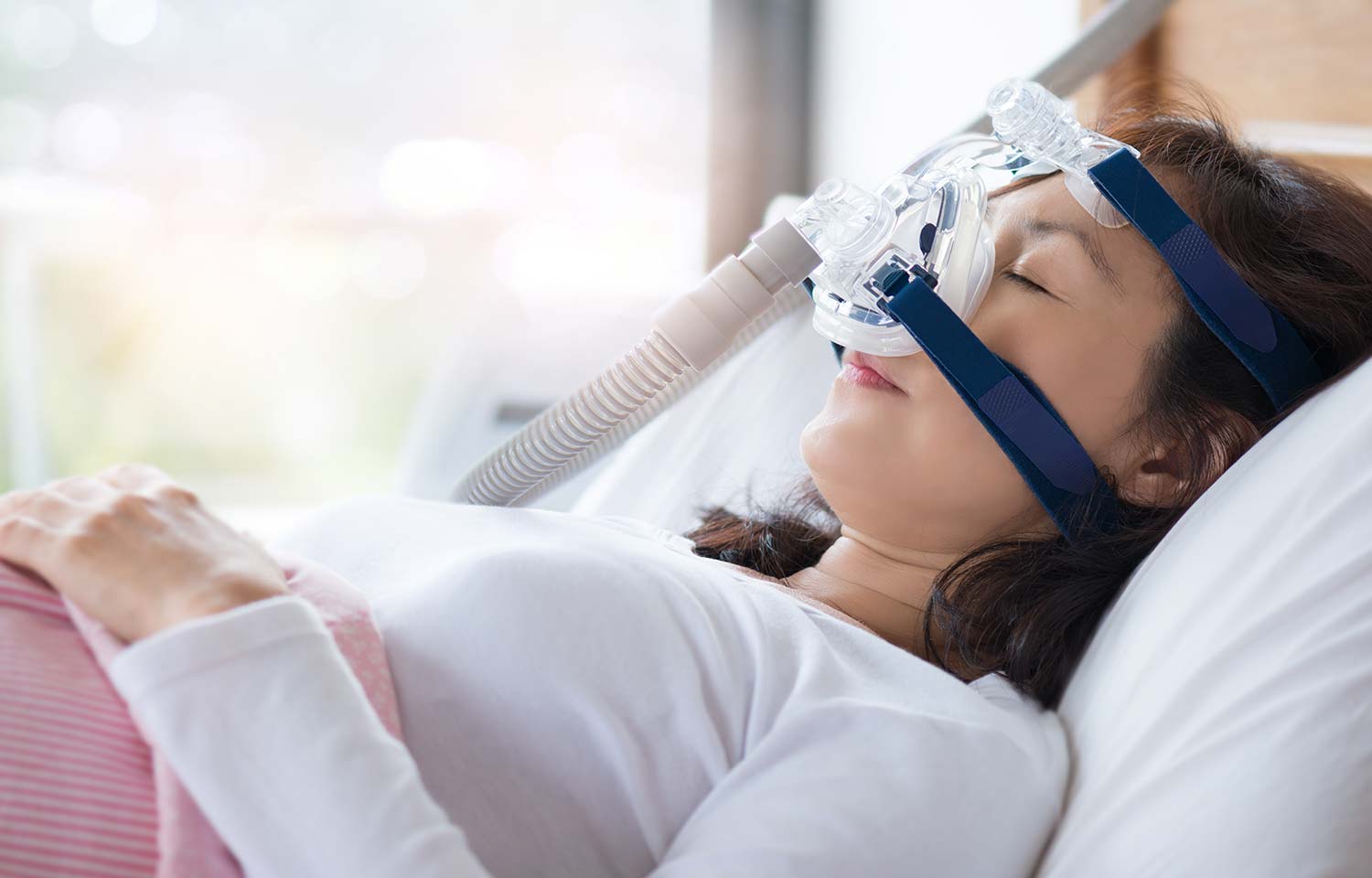
- Nasal mask: A nasal mask pumps air through a mask that covers just the nose.
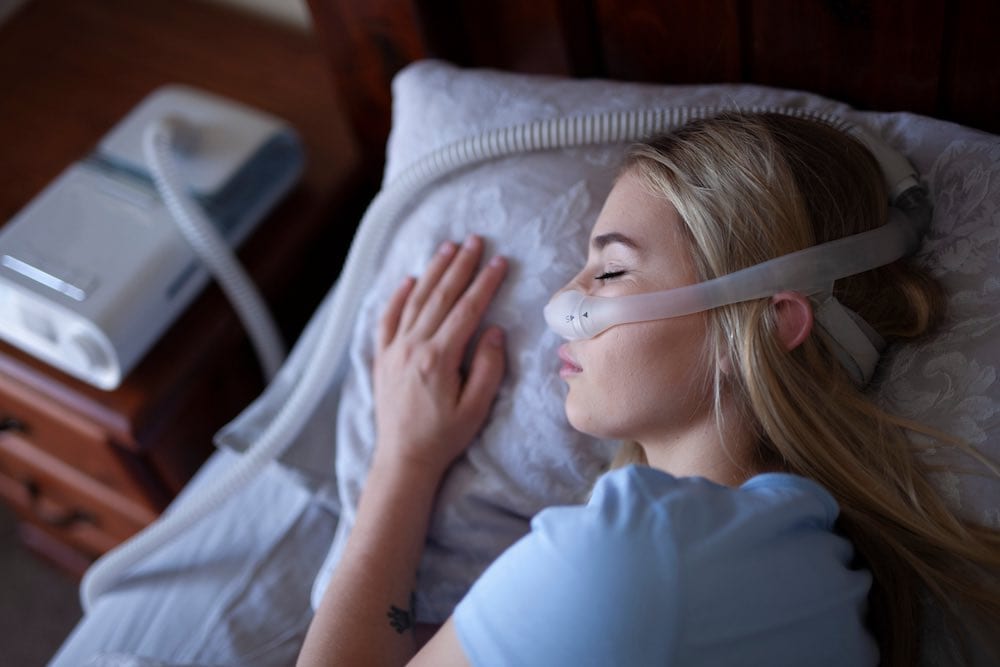
- Nasal pillow: A nasal pillow delivers air through two prongs that extend into the nose.
- Full face mask: Most full face masks cover the nose and the mouth, but some may cover the full face.
- Oral mask: An oral mask is an uncommon style that covers just the mouth.
While not typically used in a person’s home, other types of CPAP masks may be used in hospitalized patients. For example, a nasopharyngeal mask involves inserting tubes into the nose that extend into the throat.
How Does a CPAP Machine Work?
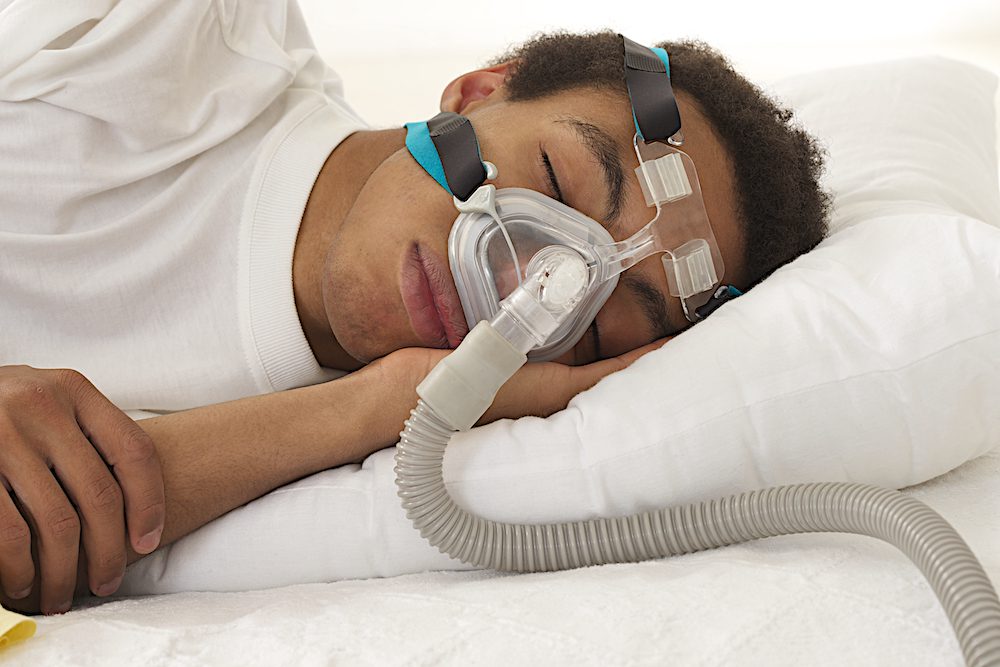
A CPAP machine operates by pushing air through a tube into a sleeper’s nose, mouth, or both as they sleep. This air applies pressure to the airway, reducing the likelihood the airway will collapse and obstruct breathing. With a traditional CPAP machine, air is pushed out continuously at one fixed rate of pressure.
CPAP machines are not the only machines that can provide positive airway pressure. Understanding the differences among the various machines that deliver PAP therapy may help shed light on why a certain type of machine is recommended by a doctor or sleep specialist.
What Does a CPAP Machine Do When You Stop Breathing?
When you stop breathing during sleep, a CPAP machine automatically delivers a steady stream of pressurized air through your mask to reopen your airway. This gentle airflow keeps your throat tissues from collapsing, allowing you to resume normal breathing without fully waking up.
Benefits of CPAP Machines
The primary benefit of using a CPAP machine is a reduction in episodes of abnormal breathing during sleep. As a result, CPAP therapy may improve symptoms associated with sleep-disordered breathing, resulting in improved sleep quality, reduced snoring, and less daytime sleepiness.
What Is a CPAP Machine Used For?
A CPAP machine is primarily used to treat sleep-related breathing disorders, especially obstructive sleep apnea (OSA). By delivering continuous air pressure, it helps keep the airway open during sleep and prevents pauses in breathing. Common uses include:
- Obstructive sleep apnea (OSA): Prevents airway collapse caused by relaxed throat muscles.
- Central sleep apnea (CSA): Helps stabilize breathing when the brain doesn’t send consistent signals to the muscles that control it.
- Snoring: Reduces or eliminates loud snoring related to upper airway obstruction.
- Improved sleep quality: Supports deeper, more restorative sleep and reduces daytime fatigue.
Does CPAP Stop Snoring?
Because snoring is usually caused by vibrations in the throat when airflow is partially blocked, the steady stream of pressurized air from a CPAP machine keeps the airway open and prevents those vibrations from occurring. While most people notice a significant improvement, occasional snoring may still happen if the mask doesn’t fit properly or the pressure settings need adjustment.
Potential CPAP Machine Side Effects
Although CPAP machines are very useful for treating sleep-disordered breathing, many people do not use their prescribed machine as much as recommended. Using a CPAP machine may produce side effects, such as:
- Dry mouth or nasal passages
- Nasal congestion or irritation
- Skin irritation or pressure marks
- Aerophagia (air swallowing), leading to bloating or gas
- Claustrophobia or discomfort
- Noise sensitivity
How to Get a CPAP Machine
The first step in getting a CPAP machine is to see a doctor. After an initial evaluation, a doctor may refer you to a sleep specialist, who can order a sleep study if they suspect you have a form of sleep-disordered breathing.
Do You Need a Prescription for a CPAP Machine?
CPAP machines are classified as medical devices, so they’re only available with a prescription.
If you’re diagnosed with sleep-disordered breathing and your doctor or sleep specialist wants you to try CPAP therapy, they will likely prescribe the best CPAP machine for you. Of course, you can ask questions and give feedback if you feel the machine they choose is not a good fit.
How Much Does a CPAP Machine Cost?
CPAP machines range from about $500 to $1,000 or more. Optional features like a heated humidifier can add to the cost of a CPAP machine.
Health insurance may cover some or all of the cost of a CPAP machine. Check with your insurance provider or doctor to learn how much you would have to pay out-of-pocket for a CPAP machine. Follow-up visits with a doctor or sleep-specialist may be required for continued coverage of your CPAP machine.
Does Medicare Cover CPAP Machines?
If you are diagnosed with obstructive sleep apnea and both your doctor and CPAP supplier are enrolled in Medicare, then Medicare will cover some of the cost of your CPAP machine. Initially, they may only cover a three-month trial, then require additional doctor’s visits before continuing coverage. You may still have to pay out-of-pocket for 20% of the cost of a CPAP machine and accessory supplies, like the mask and tube.
How to Use a CPAP Machine
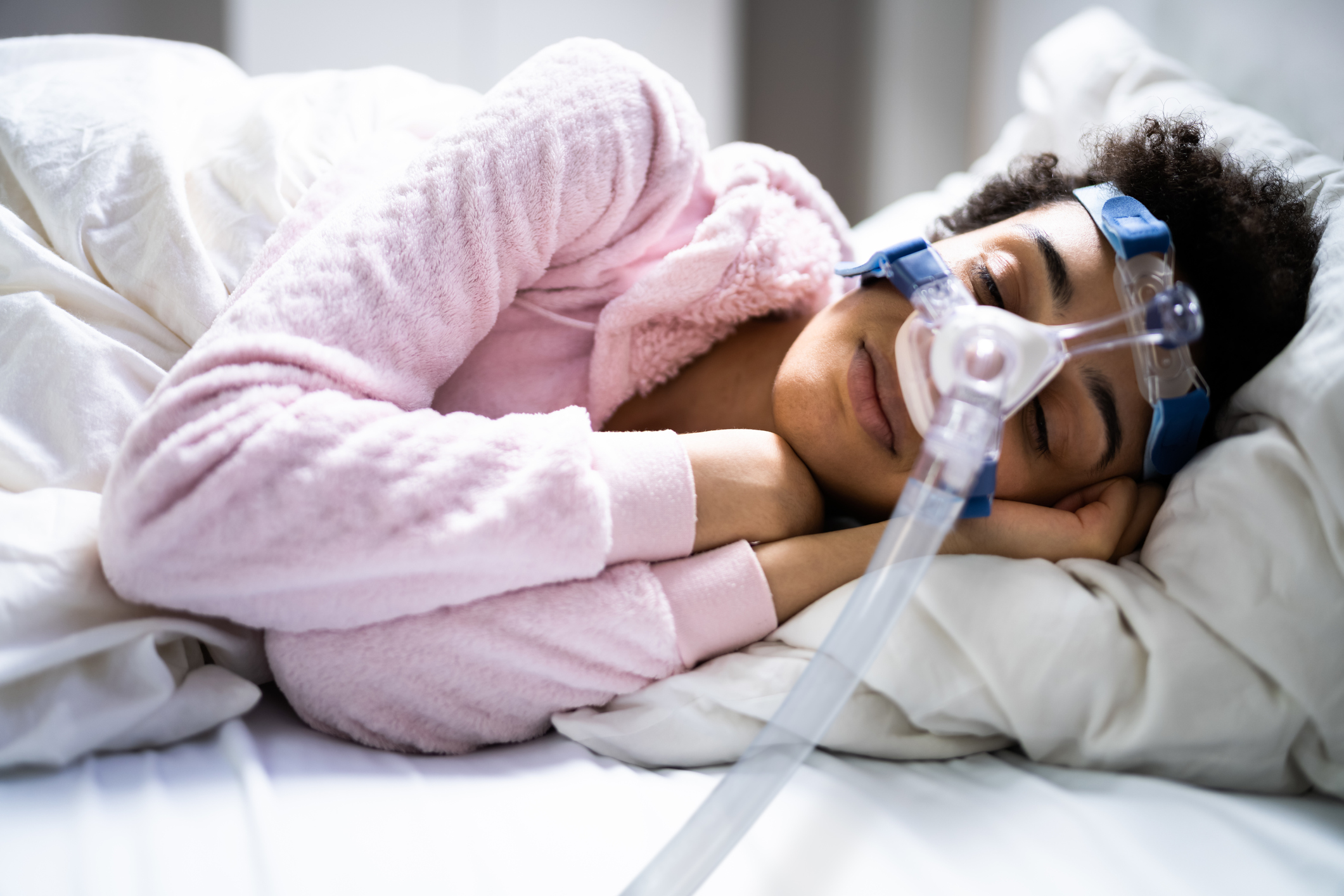
Using a CPAP machine involves wearing a fitted mask connected to a small device that delivers a steady stream of pressurized air to keep your airway open while you sleep. To get started, set up the machine on a flat surface near your bed, attach the tubing and mask, and fill the humidifier with distilled water if your device includes one. Put on the mask snugly (but not too tight), turn on the machine, and breathe normally.
Consistent nightly use is key. Most people find that comfort improves as they get used to the mask and airflow. Bu if you experience discomfort or side effects at first, there are ways to make using a CPAP machine feel more comfortable.
- Ask about a humidifier: If your CPAP machine does not have a heated humidifier, switching to one that does may reduce the likelihood of dry mouth, nosebleeds, and congestion.
- Try another mask: There are multiple styles of CPAP masks. If one feels uncomfortable or allows air to escape, another type might be a better fit.
- Clean your CPAP machine: Be sure to clean your machine regularly, as directed by the manufacturer. A clean machine can reduce the chance of infection.
- Adjust machine settings: If you have trouble sleeping because the air coming out of the CPAP machine feels too forceful, see your sleep specialist. They may adjust the airflow rate or have the machine begin at a lower rate and ramp up over time.
- Consider an APAP machine: When the air of a fixed-rate CPAP feels uncomfortable, an APAP machine that automatically adjusts the rate of airflow to your needs might be a better fit.
- Wear earplugs: If the sound of your CPAP machine makes it difficult for you to fall or stay asleep, consider wearing earplugs to block out the sound.
Frequently Asked Questions
How long does CPAP take to work?
Many people notice improvements in their sleep quality and daytime alertness within the first few nights of using CPAP therapy. For others, it may take several weeks to adjust fully and experience consistent benefits. Regular nightly use and proper mask fit help speed up this adjustment period.
How do you clean a CPAP machine?
Daily, wash the mask cushion and tubing with warm, soapy water and let them air dry. Once a week, clean the humidifier chamber and inspect the mask, tubing, and filters for signs of wear. Avoid using harsh chemicals; mild, fragrance-free soap is best. Never use UV or ozone-based cleaners, which the FDA warns may be unsafe.
Can you use purified water in a CPAP machine?
While purified water is cleaner than tap water, distilled water is the best choice for your CPAP humidifier. Distilled water prevents mineral buildup that can damage your equipment or irritate your airways. Use purified water only temporarily as a last resort if distilled water isn’t available.
Are there alternatives to CPAP machines?
Alternatives to CPAP include oral appliances that reposition the jaw to keep the airway open, positional therapy to reduce back sleeping, weight-loss programs, or advanced PAP options like BiPAP or APAP machines. For some people with severe obstructive sleep apnea, surgical treatments or newer therapies like hypoglossal nerve stimulation may also be considered.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References9 Sources
Brown, L. K. & Lee, W. (2021, September 17). Titration of positive airway pressure therapy for adults with obstructive sleep apnea. In N. Collop (Ed.). UpToDate.
https://www.uptodate.com/contents/titration-of-positive-airway-pressure-therapy-for-adults-with-obstructive-sleep-apneaNational Heart, Lung, and Blood Institute. (2022, March 24). CPAP.
https://www.nhlbi.nih.gov/health/cpapStrohl, K. P. (2020, September). Obstructive sleep apnea. Merck Manual Professional Version.
https://www.merckmanuals.com/professional/pulmonary-disorders/sleep-apnea/obstructive-sleep-apneaPinto, V. L., & Sharma, S. (2022, May 2). Continuous positive airway pressure. In StatPearls. StatPearls Publishing.
https://www.ncbi.nlm.nih.gov/books/NBK482178/A.D.A.M. Medical Encyclopedia. (2020, January 29). Positive airway pressure treatment. MedlinePlus.
https://medlineplus.gov/ency/article/001916.htmDeshpande, S., Joosten, S., Turton, A., Edwards, B. A., Landry, S., Mansfield, D. R., & Hamilton, G. S. (2016). Oronasal masks require a higher pressure than nasal and nasal pillow masks for the treatment of obstructive sleep apnea. Journal of Clinical Sleep Medicine, 12(9), 1263–1268.
https://pubmed.ncbi.nlm.nih.gov/27448430/Weaver, T. E. (2021, September 28). Assessing and managing nonadherence with continuous positive airway pressure (CPAP) for adults with obstructive sleep apnea. In N. Collop (Ed.). UpToDate.
https://www.uptodate.com/contents/assessing-and-managing-nonadherence-with-continuous-positive-airway-pressure-cpap-for-adults-with-obstructive-sleep-apneaAmerican Academy of Sleep Medicine. (2018, October 19). FDA reclassifies positive airway pressure as a Class II medical device.
https://aasm.org/fda-reclassifies-positive-aiway-pressure-class-ii-medical-device/U.S. Centers for Medicare and Medicaid Services. (n.d.). Continuous positive airway pressure (CPAP) devices, accessories, & therapy.
https://www.medicare.gov/coverage/continuous-positive-airway-pressure-devices