When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
EPAP Therapy: Expiratory Positive Airway Pressure
- Expiratory positive airway pressure (EPAP) offers a portable, no-electricity treatment alternative to CPAP for people with mild to moderate sleep apnea.
- While more research is needed, studies so far show that EPAP can effectively reduce breathing interruptions, snoring, and daytime sleepiness with limited serious adverse effects.
- Many insurance companies do not cover EPAP therapy, and your suitability for the treatment can depend on your breathing style and the severity of your diagnosis. A medical professional can help you determine if it’s a good treatment option.
While continuous positive airway pressure (CPAP) therapy is an effective, commonly prescribed treatment for obstructive sleep apnea (OSA), it’s not the right fit for everyone. For people who cannot tolerate CPAP machines, expiratory positive airway pressure (EPAP) has emerged as an innovative potential alternative.
EPAP devices offer a simpler, more portable approach to treating sleep apnea without the bulk, noise, or electricity requirements of traditional CPAP machines. We’ll explore the differences between these therapies and help you understand which treatment option might be right for you.

Exploring CPAP Machines — But Haven’t Been Tested Yet?
Start with our easy, at-home sleep test. It’s stress-free and effective. Get results within a few days.
What Is EPAP?
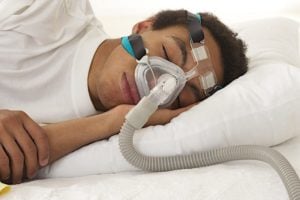
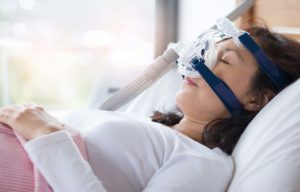
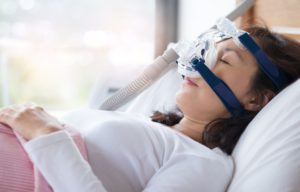
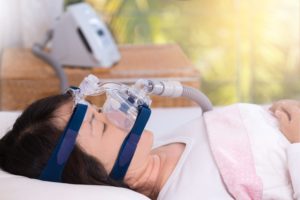
Expiratory positive airway pressure (EPAP) is a therapy that uses a small valve attached to the nostrils to treat sleep apnea. This valve uses only the sleeper’s breath to create pressure as they exhale. This pressure prompts physical changes that make it more likely the airway will remain open during inhalation, reducing the periods of lapsed breathing that characterize sleep apnea.
Unlike a CPAP device, an EPAP does not use electricity or add pressure on inhalation. EPAP is considered an emerging therapy for sleep apnea, available as an alternative for people who cannot or do not want to use the standard CPAP therapy.
In multiple studies, EPAP devices have been demonstrated as a successful treatment for sleep apnea. In one study, EPAP devices significantly reduced the number of times people with OSA stopped breathing during sleep, as well as decreased feelings of daytime sleepiness . A study comparing EPAP and CPAP therapies in people with OSA found no significant difference — both therapies were helpful and safe.
A long-term study of people with OSA found that adherence to EPAP after one year was excellent, provided the therapy was working at the 3-month mark. People using EPAP had fewer breathing cessations, reduced snoring, and less daytime sleepiness.
What Are the Benefits of EPAP Therapy?
EPAP therapy offers potential benefits both in treating sleep apnea and in addressing common problems people experience with CPAP machines.
Clinical Benefits
Research shows that, with proper adherence, EPAP therapy may significantly reduce the number of breathing interruptions during sleep. As a result, it can decrease snoring and gasping during the night. Studies have also found that EPAP improves oxygen levels during sleep and reduces daytime sleepiness.
Practical Benefits
Both CPAP and EPAP therapy require consistent use to be effective. EPAP devices address many of the common complaints that reduce CPAP adherence:
- Less claustrophobic: EPAP uses small nasal valves rather than full face or nasal masks that some people find uncomfortable or confining
- Portability: EPAP devices are small and lightweight, making them easy to travel with, unlike bulky CPAP machines
- No electricity required: EPAP can be used in locations without electrical outlets
- Quieter operation: EPAP devices produce no noise, eliminating complaints about machine sounds disturbing sleep
- Simpler maintenance: EPAP devices require less cleaning and upkeep than CPAP machines with their masks, tubing, and filters
What Are the Side Effects of EPAP Therapy?
Like most medical treatments, EPAP therapy can cause side effects, though they are generally more mild than CPAP effects. In clinical trials, about 42% of people using EPAP devices reported experiencing side effects.
The most commonly reported side effects were difficulty exhaling, nasal discomfort, dry mouth, headache, and insomnia. Other reported side effects include nasal congestion, nasal drainage, nasal itching, and difficulty breathing.That said, research has found no serious adverse effects related to EPAP use overall, and adherence rates remained high even among people experiencing side effects.
EPAP vs. CPAP: What Is the Difference?
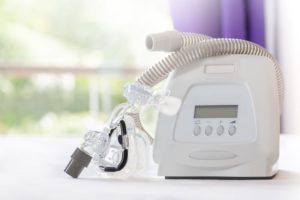
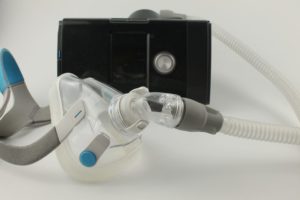
The primary differences between EPAP and CPAP therapies are in how the devices look and function. A CPAP machine has a motor that pushes filtered air through a tube into the sleeper’s airway, helping keep the airway open throughout the night.
To use a CPAP machine, a sleeper must wear a mask that covers their nose or nose and mouth. The entire setup needs to be cleaned regularly, with certain parts replaced every few months. CPAP machines can run on battery power, but most plug into the wall and use electricity.
In comparison to a CPAP machine, an EPAP device is small and light, and it does not require battery power or electricity. Instead, an EPAP device fits in or over the nostrils and contains a valve that naturally creates pressure as a person exhales. This pressure helps keep the airway open when the person later inhales. An EPAP device works because of the sleeper’s own breath and doesn’t involve pushing any external air into the airway, like the CPAP machine does.
Is EPAP as Effective as CPAP?
Further research is needed to determine if an EPAP device is as effective as a CPAP machine when it comes to treating OSA. Some studies show that the two OSA therapies are equally effective. Other studies, however, suggest that a CPAP machine can be more effective .
Even if a CPAP machine is more effective overall, it can only work when it is being regularly used. Initial research shows promising results for EPAP adherence , with some studies finding that people use the EPAP device 92% of the time. If a person doesn’t adhere to CPAP therapy, using an EPAP device would be more effective than no treatment at all.
Who Is EPAP Best For?
Although EPAP therapy is still considered an alternative treatment for OSA, an EPAP device could be a better option for people who cannot consistently tolerate using a CPAP machine.
People might be interested in an EPAP device if they want to discontinue using a CPAP machine due to side effects. An EPAP device might also be a better choice for people who travel. Because an EPAP device is much smaller and lighter than a CPAP machine, it is easier to carry. An EPAP device doesn’t require electricity, so it can be easily used while camping or sleeping away from an electrical outlet. A CPAP machine requires routine cleaning and maintenance.
Who Is CPAP Best For?
The efficacy of CPAP therapy for OSA is backed by a large body of scientific research. Most doctors initially prescribe CPAP therapy after diagnosing a person with OSA.
A CPAP machine works best for people with OSA who are able to tolerate the machine. Tolerating the machine well means that a person can fall asleep and stay asleep with their CPAP mask on, without experiencing many negative side effects. Full-face CPAP masks may be more effective than nasal EPAP devices for people who tend to breathe through their mouth.
Although CPAP machines are not as small as EPAP devices, there are portable, battery-operated CPAP machines available that are easier to travel with than standard CPAP machines.
How Do I Decide Which PAP Therapy Is Right for Me?
You can consider an at-home sleep apnea test to determine your best first steps. However, if you’ve already been diagnosed with OSA, you should discuss your situation with your doctor or sleep specialist to determine which treatment is best for you. Usually, most doctors recommend people with OSA try a CPAP machine first.
Although CPAP machines require a greater investment up front, they are generally covered at least in part by most insurance plans. Coverage for EPAP devices may be more limited, and in the case of disposable EPAP devices, they may be expensive over the long term.
In general, the best treatment for you will depend on the severity of your diagnosis, as well as a number of personal factors. For example, EPAP therapy is generally recommended only for patients with mild to moderate sleep apnea. Also, EPAP may not be suitable for people with significant nasal obstruction or those who breathe through their mouths as the device requires nasal breathing and clear nasal passages to function properly.
On the other hand, if you experience side effects from CPAP that affect your ability to maintain consistent treatment, you should talk to your doctor about whether EPAP therapy could be an option. Together, you and your doctor can develop a treatment plan that helps you get the rest you need each night.
Frequently Asked Questions
Is EPAP FDA-approved?
The U.S. Food and Drug Administration (FDA) has cleared several prescription EPAP devices as Class II medical devices to treat sleep apnea. Some non-prescription EPAP devices are also available, but they are only FDA-approved to treat snoring, not sleep apnea.
Can EPAP stop snoring?
While more research is needed, studies so far have shown that EPAP therapy can significantly reduce snoring by creating pressure during your exhales that helps keep the airway open.
Will my insurance cover EPAP therapy?
Many insurance companies, including Medicare, do not currently cover EPAP devices because they are often considered experimental despite FDA clearance.
In contrast, CPAP therapy is typically well-covered by insurance, with Medicare covering 80% of costs after the deductible.
However, insurance policies vary widely and you should check with your provider to verify coverage.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of product specialists, sleep health professionals, and people just like you. Whether you’re searching for the perfect mattress or need expert sleep advice, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
13 Sources
-
Lorenzi-Filho, G., Almeida, F. R., & Strollo, P. J. (2017). Treating OSA: Current and emerging therapies beyond CPAP. Respirology, 22(8), 1500–1507.
https://pubmed.ncbi.nlm.nih.gov/28901030/ -
Berry, R. B., Kryger, M. H., & Massie, C. A. (2011). A novel nasal expiratory positive airway pressure (EPAP) device for the treatment of obstructive sleep apnea: A randomized controlled trial. Sleep, 34(4), 479–485.
https://pubmed.ncbi.nlm.nih.gov/21461326/ -
Liu, Y., Ying, Y., Pandu, J. S., Wang, Y., Dou, S., Li, Y., & Ma, D. (2019). Efficacy and safety assessment of expiratory positive airway pressure (EPAP) mask for OSAHS therapy. Auris, Nasus, Larynx, 46(2), 238–245.
https://pubmed.ncbi.nlm.nih.gov/30262209/ -
Kryger, M. H., Berry, R. B., & Massie, C. A. (2011). Long-term use of a nasal expiratory positive airway pressure (EPAP) device as a treatment for obstructive sleep apnea (OSA). Journal of Clinical Sleep Medicine: Official Publication of the American Academy of Sleep Medicine, 7(5), 449–453B.
https://pubmed.ncbi.nlm.nih.gov/22003339/ -
Riaz, M., Certal, V., Nigam, G., Abdullatif, J., Zaghi, S., Kushida, C. A., & Camacho, M. (2015). Nasal expiratory positive airway pressure devices (Provent) for OSA: A systematic review and meta-analysis. Sleep Disorders, 2015, 734798.
https://pubmed.ncbi.nlm.nih.gov/26798519/ -
Wu, H., Yuan, X., Zhan, X., Li, L., & Wei, Y. (2015). A review of EPAP nasal device therapy for obstructive sleep apnea syndrome. Sleep & Breathing = Schlaf & Atmung, 19(3), 769–774.
https://pubmed.ncbi.nlm.nih.gov/25245174/ -
Walsh, J. K., Griffin, K. S., Forst, E. H., Ahmed, H. H., Eisenstein, R. D., Curry, D. T., Hall-Porter, J. M., & Schweitzer, P. K. (2011). A convenient expiratory positive airway pressure nasal device for the treatment of sleep apnea in patients non-adherent with continuous positive airway pressure. Sleep Medicine, 12(2), 147–152.
https://pubmed.ncbi.nlm.nih.gov/21256800/ -
Iftikhar, I. H., Bittencourt, L., Youngstedt, S. D., Ayas, N., Cistulli, P., Schwab, R., Durkin, M. W., & Magalang, U. J. (2017). Comparative efficacy of CPAP, MADs, exercise-training, and dietary weight loss for sleep apnea: A network meta-analysis. Sleep medicine, 30, 7–14.
https://pubmed.ncbi.nlm.nih.gov/28215266/ -
Rosenthal L, Massie CA, Dolan DC, Loomas B, Kram J, Hart RW. A multicenter, prospective study of a novel nasal EPAP device in the treatment of obstructive sleep apnea: efficacy and 30-day adherence. J Clin Sleep Med. 2009;5(6):532-537.
https://pmc.ncbi.nlm.nih.gov/articles/PMC2792968/ -
Emerging OSA Treatment Alternatives -Side-By-Side Comparison AASM Emerging Technology Committee.
https://aasm.org/wp-content/uploads/2021/10/Montage_Tech_Article_Supplemental_Content_21.pdf -
A Novel Non-Prescription Nasal EPAP Device (Theravent) to Treat Snoring. Sleepdt.com. Published August 3, 2012.
https://sleepdt.com/a-novel-non-prescription-nasal-epap-device-theravent-to-treat-snoring/ -
Medicare Medical Policy Sleep Disorder Treatment with Positive Airway Pressure MEDICARE MEDICAL POLICY NUMBER: 53.
https://www.providencehealthplan.com/-/media/providence/website/pdfs/providers/medical-policy-and-provider-information/medical-policies/mp53.pdf -
Continuous Positive Airway Pressure (CPAP) therapy. Medicare. Published 2025.
https://www.medicare.gov/coverage/continuous-positive-airway-pressure-devices#coverage-content-description