When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Does Insurance Cover CPAP Machines?
- Most insurance plans, as well as Medicare and Medicaid, partially cover the cost of CPAP machines and necessary supplies.
- To qualify for insurance coverage, you’ll need a prescription from your doctor.
- Some insurance providers reimburse for purchases, while others require rent-to-own arrangements.
- Buying CPAP machines without insurance may cost less than with a high-deductible plan, but you’ll still need a prescription.
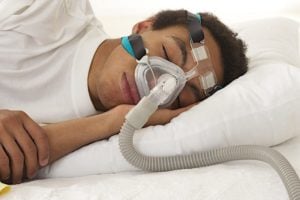
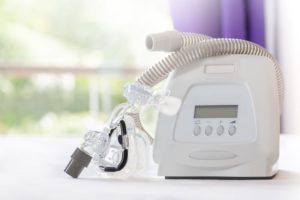
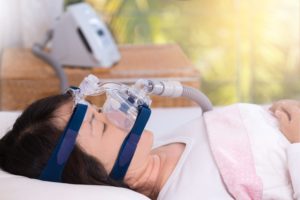
If you’ve been diagnosed with obstructive sleep apnea (OSA), your doctor may prescribe you a continuous positive airway pressure (CPAP) machine to help you sleep better. While CPAP therapy is considered effective treatment for most people with OSA, it can also be expensive. CPAP machine prices can amount to hundreds, if not thousands, of dollars in out-of-pocket costs, and this does not include the cost of important accessories such as face masks.
We’ll cover some of the most common insurance policies surrounding CPAP equipment. These policies may be updated from time to time, so always check with your insurance provider for the most up-to-date information. You can see our recommended suppliers that take insurance for CPAP here.

Exploring CPAP Machines — But Haven’t Been Tested Yet?
Start with our easy, at-home sleep test. It’s stress-free and effective. Get results within a few days.
How Does Insurance for CPAP Machines Work?
Most insurance plans partially cover the costs of CPAP machines and related equipment. The machines are often covered to an extent, but you may be responsible for other components such as tubing. Insurance allows for replacement parts at specific intervals, according to a set schedule (see below for more details). Many insurance providers require you to meet your annual deductible before covering your CPAP equipment.
Insurance providers typically take your apnea-hypopnea index (AHI) into consideration when determining your eligibility for CPAP therapy coverage. Your AHI is the average number of partial or complete breathing cessation events you experience per hour. To determine your AHI, you must undergo a sleep study in a sleep lab or take a home sleep test (HST).
Sleep apnea is classified as mild, moderate, or severe, depending on the AHI reading . An AHI of 5 to 15 is considered mild, 15 to 30 is moderate, and greater than 30 is severe. Medicaid and Medicare partially cover CPAP machines for all three AHI indexes, provided you meet certain conditions . Some insurance providers follow different standards. Be sure to check your insurance policy to determine specific requirements.
What Do I Need to Get Insurance to Cover My CPAP Machine?
Before most insurance providers will pay for your CPAP equipment, you must fulfill two requirements .
- First, you must obtain a prescription for CPAP therapy from your healthcare provider.
- Second, you must successfully complete a compliance period with the CPAP machine to demonstrate that you are using the treatment correctly and regularly .
Some insurances also require a visit with the doctor before testing to establish the need for testing as well as a visit post study completion.
In order to write you a prescription for a CPAP machine, your doctor must confirm that your sleep difficulties are caused by sleep apnea and not another condition. Your doctor will first check for symptoms of obstructive sleep apnea , including:
- Loud snoring throughout the night
- Gasping or snorting during sleep
- Excessive daytime sleepiness
- Forgetfulness
- Headaches
- Drowsiness or falling asleep while driving
Sleep Study and CPAP Prescription
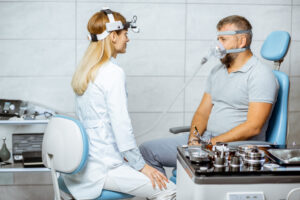
If your symptoms indicate you might have obstructive sleep apnea, the next step is to take a sleep study . Doctors can test for sleep apnea with an overnight in-lab sleep study, also called polysomnography, or with a home sleep test (HST) you’ll self-administer before sleeping in your own bed.
After reading and interpreting the results of your sleep study, your doctor may diagnose you with sleep apnea and work with you to develop a treatment plan.
CPAP Compliance Requirements
In order to be eligible for reimbursement , the Centers for Medicaid and Medicare (CMS) require proof that you are using the CPAP machine at least four hours per night, on 70% of nights, in a consecutive 30-day period. Most machines record your use for you.
Some machines connect to an app on your phone and transmit usage information, while others use an SD card reader to collect the data. If you’re unable to meet these requirements during the first three months, you may have to restart the process. They can also require you to turn in the equipment.
While these are the most common prescription and compliance requirements for CPAP coverage, each provider has its own specific rules. Review your policy to learn about the requirements specific to your insurance provider.
What Does CPAP Insurance Coverage Include?
Insurance coverage and costs for CPAP equipment depend on your specific policy and whether you are complying with usage requirements. When considering costs and insurance coverage, it’s important to look beyond just the machine. We’ll explain typical insurance coverage for CPAP machines, supplies, and optional accessories.
CPAP Machines
Your insurance coverage for a CPAP machine depends on your provider. Some providers reimburse you for the cost of purchasing the machine outright, while others require a rent-to-own plan under which you must use the machine for a set period before owning it.
On average, most CPAP machines cost between $700 and $1,000. BiPAP and APAP machines frequently run in the thousands of dollars. Typical insurance plans, including Medicare and Medicaid, cover up to 80% of these costs once the policy-holder has met their deductible. Some CPAP machines may not be covered at all. For example, most insurance providers consider travel CPAP machines to be non-essential devices.
If you are on a rent-to-own structure, your monthly fee typically equals the cost of the CPAP machine divided by the number of rental months. The exact amount your insurance company pays depends on your policy. If you rent for longer than a year, you may need to pay a second deductible.
If your insurance company determines you are not using the machine frequently enough as per your policy, they may stop covering their portion of the machine rental.
Be aware that if you decide to stop CPAP treatment and decide later that you want to try the treatment again, your insurance company may require you to re-do the prescription process to qualify for coverage. The doctor’s appointments and sleep study may pose additional costs, depending on your policy.
If this all sounds overwhelming, CPAPinsurance.com can help simplify the process. The site walks you through your options and connects you with recommended providers so you can get your CPAP machine and supplies through insurance — without the guesswork.
CPAP Supplies
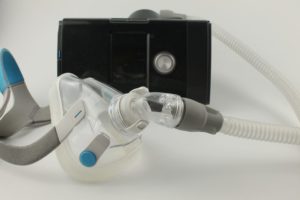
When beginning CPAP treatment, the biggest upfront cost is the CPAP machine itself. Then there are supplies that need to be replaced over time, including:
- Masks
- Mask components
- Tubing
- Filters
- Chin straps
- Headgear
- Water chamber
The costs for each component vary. Filters, which need to be replaced frequently, run between $5 and $30 each. Most masks cost at least $100, and other equipment ranges between $20 and $100 per component. Some rental plans may include the cost of replacement equipment, which is something to bear in mind when comparing the cost of buying outright versus purchasing with insurance.
Many insurance providers use the Medicare guidelines for replacing equipment:
| Item Description | Replacement Schedule |
| Combination Oral/Nasal CPAP Mask | Every 3 months |
| Full Face Mask | Every 3 months |
| Chinstrap | Every 6 months |
| Tubing | Every 3 months |
| Headgear | Every 6 months |
| Disposable Filter | Twice per month |
| Nondisposable Filter | Every 6 months |
| Humidifier Water Chamber | Every 6 months |
CPAP Accessories
As you adjust to CPAP treatment, you may want additional accessories for more comfortable sleep and easier travel. There are a number of optional accessories you can purchase for your CPAP machine. These include:
- CPAP pillows are cut to accommodate the machine and tubing and allow you to move during the night.
- CPAP cleaners may help disinfect your machine and extend its longevity.
- Mask liners can wick away moisture and ensure a tighter seal to keep the mask in place.
- Hose holders help the CPAP machine feel softer against the body and look less medical in appearance.
- CPAP batteries are convenient for travel when you don’t have access to a power outlet.
- Travel bags can hold all your CPAP equipment when you’re on the go.
Insurance does not typically cover any products that are considered optional. Costs for these products can vary depending on the quality. More expensive accessories often come with warranties of one to three years.
Does Medicare Cover CPAP?
Medicare considers CPAP devices to be durable medical equipment (DME) and provides 80% coverage under Part B as long as you meet certain conditions. First, your doctor must diagnose you with obstructive sleep apnea following an approved laboratory sleep study or an at-home sleep study and give you a prescription for a CPAP machine.
Then, Medicare covers a 12-week initial period of CPAP therapy for obstructive sleep apnea, as long as you meet one of thefollowing requirements:
- You have an hourly AHI between 5 and 14 and acomorbid condition related to obstructive sleep apnea, including hypertension, history of stroke, heart disease, excessive daytime sleepiness, insomnia, mood disorders, and impaired cognition.
- You have an hourly AHI of 15 or higher.
You must also meet Medicare’s compliance requirements, which state that you must use the machine at least four hours per night, 70% of the time or more, during the first three months. If you fail to meet these requirements, you’ll need to begin the process again. This involves completing another sleep study, either in a lab or at home, and obtaining another prescription from your doctor.
If the CPAP therapy helps improve your sleep apnea symptoms during the 12-week period, Medicare will continue to cover the cost of your CPAP equipment. With Original Medicare coverage, you pay 20% of the machine rental plus the cost of supplies such as the CPAP mask and tubing. Once you meet your Medicare Plan B deductible, Medicare pays for the rental of the machine for 13 months if you use it continually. After 13 months, you own the machine.
Does Medicaid Cover CPAP?
Medicaid programs vary by state, and typically follow the same guidelines as Medicare . You need a sleep test, diagnosis of obstructive sleep apnea, and prescription from your doctor. Your AHI must also meet one of the same requirements as for Medicare:
- AHI index between 5 and 14, along with a comorbidity related to obstructive sleep apnea
- AHI of at least 15
If you meet these requirements, then Medicaid provides CPAP coverage for a 12-week trial. Coverage continues if your sleep apnea improves with the CPAP treatment. You must also adhere to the same compliance requirements as Medicare recipients, namely using the machine at least four hours every night on 70% of nights.
Can You Buy a CPAP Machine Without Insurance?
Insurance plans can significantly help with the cost of a CPAP machine. However, if you have a high deductible, you may consider bypassing insurance and purchasing CPAP equipment on your own.
When making your decision, calculate whether your CPAP equipment is likely to cost more than your deductible, remembering to budget the ongoing costs of tubes, filters, and other replacements. You might be able to find direct-to-supplier CPAP manufacturers with lower prices than those available through your insurance plan, though be sure to check if these devices are approved by the FDA.
When you choose to buy your CPAP equipment without insurance, you can skip the rent-to-own process and own your machine right away. You also avoid the insurance requirements of treatment compliance. This eliminates the risk of needing to return your machine and restart the prescription process.
Another benefit to paying a medical equipment supplier directly is the wider selection of products, since insurance often restricts you to covered suppliers.
Keep in mind that whether or not you use insurance, you’ll still need to complete a sleep study — either in a lab or at home — and obtain a CPAP prescription.
Frequently Asked Questions
How often does insurance cover CPAP machines?
Most insurance plans offer partial coverage for CPAP machines once you meet your deductible. Medicare participants are responsible for paying their deductible, plus 20% of the machine rental. If you have a high deductible under your health insurance policy, you may end up covering the full cost of your CPAP machine.
How much will I pay for CPAP equipment?
The lowest CPAP machine prices start around $250 for certified refurbished machines, but for new machines, the price can easily exceed $1,000. More advanced machines tend to cost more. How much you pay depends on your insurance coverage. You’ll also need to pay for additional equipment such as filters, which run between $5 and $30, and masks, which typically start at $100. Other CPAP equipment ranges between $20 and $100 per component.
Does my deductible apply to CPAP equipment?
Most insurance deductibles apply to essential CPAP equipment and don’t include optional accessories. Providers usually have schedules to cover replacements for components such as tubes, masks, and filters. If you require more frequent replacements of certain components, you may need to pay these costs out of pocket.
Will insurance pay for sleep apnea sleep studies?
Most insurance plans cover a portion of the cost of your sleep studies, including studies conducted in a sleep lab or at home. Typically, you need a referral for a sleep study in order to receive coverage. Your doctor must determine which type of study is right for you.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of product specialists, sleep health professionals, and people just like you. Whether you’re searching for the perfect mattress or need expert sleep advice, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
12 Sources
-
A.D.A.M. Medical Encyclopedia. (2020, January 29). Polysomnography. MedlinePlus.
https://medlineplus.gov/ency/article/003932.htm -
Centers for Medicare & Medicaid Services. (2009, March 3). Sleep testing for obstructive sleep apnea (OSA). Centers for Medicare & Medicaid Services.
https://www.cms.gov/medicare-coverage-database/view/ncd.aspx?NCDId=330&ncdver=1&bc=AAAAQAAAAAAAAA%3D%3D& -
American Academy of Sleep Medicine. (2018, October 19). FDA reclassifies positive airway pressure as a Class II medical device.
https://aasm.org/fda-reclassifies-positive-aiway-pressure-class-ii-medical-device/ -
American Academy of Sleep Medicine Sleep Education (2025). Positive Airway Pressure and Your Insurance: What You Should Know.
https://sleepeducation.org/patients/pap-and-insurance/ -
MedlinePlus: National Library of Medicine (US). (2023, January 9). Obstructive sleep apnea – adults
https://medlineplus.gov/ency/article/000811.htm -
National Heart, Lung, and Blood Institute. (2022, March 24). Sleep studies.
https://www.nhlbi.nih.gov/health/sleep-studies -
Naik, S., Al-Halawani, M., Kreinin, I., & Kryger, M. (2019). Centers for Medicare and Medicaid Services positive airway pressure adherence criteria may limit treatment to many Medicare beneficiaries. Journal of Clinical Sleep Medicine, 15(02), 245–251.
https://pubmed.ncbi.nlm.nih.gov/30736874/ -
Office of Inspector General. (2013, June). Replacement schedules for Medicare continuous positive airway pressure supplies. Department of Health and Human Services.
https://oig.hhs.gov/oei/reports/oei-07-12-00250.pdf -
U.S. Centers for Medicare and Medicaid Services. (n.d.) Durable medical equipment (DME) coverage. Medicare.gov.
https://www.medicare.gov/coverage/durable-medical-equipment-dme-coverage -
Centers for Medicare and Medicaid. (2024). Continuous Positive Airway Pressure (CPAP) Therapy for Obstructive Sleep Apnea (OSA).
https://www.cms.gov/medicare-coverage-database/view/ncacal-decision-memo.aspx?proposed=N&NCAId=204 -
Centers for Medicare and Medicaid .(2008). Continuous Positive Airway Pressure (CPAP) Therapy For Obstructive Sleep Apnea (OSA),
https://www.cms.gov/medicare-coverage-database/view/ncd.aspx?ncdid=226 -
Medicaid.gov. (2025). State Profiles.
https://www.medicaid.gov/state-overviews/state-profiles