When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Aerophagia: Symptoms, Causes, and Treatment
- Definition: Aerophagia occurs when excessive air swallowing leads to a buildup in your digestive system, resulting in symptoms like bloating, belching, and abdominal discomfort.
- Causes: Common causes can include use of CPAP machines, anxiety, carbonated drinks, and rushing through meals.
- Symptoms: You may experience bloating, belching, flatulence, gurgling stomach, abdominal pain, or distended belly.
- Diagnosis: Your healthcare provider will review your symptoms and may order an abdominal x-ray. A diagnosis requires symptoms lasting for at least 12 weeks within a year.
- Treatment: Aerophagia caused by CPAP can often be fixed by adjusting features or changing masks. Other cases can be addressed by lifestyle changes, therapy, or stress reduction.
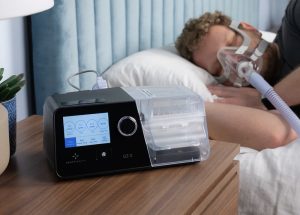
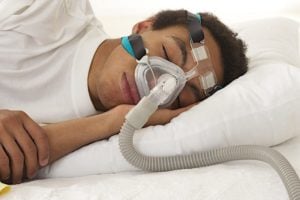
Frequent belching, bloating, and abdominal discomfort are common complaints from people who suffer from a condition called aerophagia. This disorder is caused by swallowing more air than normal, and often goes unrecognized. Using continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA) can increase the chances of this disorder, so if you use a CPAP machine, you may notice some symptoms.
It’s important to know that there are many ways to reduce discomfort from swallowed air. Understanding what causes aerophagia and when to visit a doctor are the first steps toward getting relief.
What Is Aerophagia?
Aerophagia is a digestive disorder that occurs when a person swallows too much air. Some air swallowing is normal during eating and drinking, but the excess swallowing associated with aerophagia causes air to accumulate in the stomach and intestines instead of the lungs. This results in bloating and belching, as well as other uncomfortable digestive symptoms. The disorder is very common, but despite frequent gulping and other telltale signs, people may not realize that air swallowing is the cause of their discomfort.
What Causes Aerophagia?
Aerophagia can happen anytime a person swallows too much air, but this may occur more often during certain activities or situations. Here are some common triggers:
Medical conditions and treatments
- CPAP therapy, a treatment for OSA, especially during the initial phase of treatment
- Gastroesophageal reflux disease (GERD)
- Anxiety or stress, which can cause irregular breathing patterns
- Nausea
- Certain medications or drugs
- Wearing loose dentures
Activities and behaviors
- Lying on your back
- Drinking carbonated beverages
- Chewing gum
- Using a drinking straw
- Smoking
- Talking quickly while eating
- Eating or drinking too fast
How Do CPAP Machines Cause Aerophagia?
CPAP devices deliver a constant stream of pressurized air designed to keep the airway open for people with OSA. As your muscles relax during sleep, the separation between the windpipe and the esophagus becomes weaker, allowing air to pass more easily into the esophagus. This air then travels down the esophagus into the stomach and sometimes the intestines.An estimated 16 to 50% of CPAP users experience aerophagia symptoms, including both children and adults. Some researchers have also linked aerophagia from CPAP to symptoms of gastroesophageal reflux, or heartburn. The theory is that as swallowed air causes the stomach to bloat, the stomach pushes upwards, making it easier for stomach acid to rise up into the esophagus.
What Are the Symptoms of Aerophagia?
Aerophagia is characterized by excessive air swallowing. The word aerophagia means “ air eating ” in Greek. The air enters the gastrointestinal tract and causes a range of symptoms.
The symptoms of aerophagia are related to the way air passes through the body. Depending on whether the air primarily stays higher up or passes down through the intestines, you may experience:
- Bloating
- Belching
- Flatulence
- Gurgling stomach
- Abdominal pain or discomfort
- Distended belly
Though some of the symptoms are similar, aerophagia is considered a different disorder than excessive belching, irritable bowel syndrome, constipation, or functional dyspepsia, which is indigestion with no known cause. Aerophagia is not caused by a blockage in the intestines. That being said, it is not uncommon for people with aerophagia to have another gastrointestinal disorder as well.
Less common symptoms include constipation, diarrhea, decreased appetite, and nausea. Unlike with other gastrointestinal disorders, vomiting is not generally considered a symptom of aerophagia. Symptoms may come and go over time.
How Is Aerophagia Diagnosed?
To diagnose aerophagia, your doctor may ask you to describe your symptoms, particularly regarding belching, bloating, abdominal pain, flatulence, or constipation. They may check for signs of a distended belly and tap your abdomen to see if it sounds like there is extra air inside. They may also listen for bowel sounds and verify that you do not have any physical blockages obstructing your intestines.
An abdominal X-ray, also called a radiograph, can provide visual confirmation of excessive air inside your intestines or expanded bowels due to air. With this test, your doctor checks for air-fluid levels , a pattern of air and fluid mixing together that indicates a bowel obstruction.
Your doctor might also rule out supragastric belches, which differ from air swallowing in that the air enters the esophagus and immediately comes out again. If appropriate, they may perform an upper endoscopy, which consists of inserting a small camera into the esophagus and stomach.
To receive a diagnosis of aerophagia, you must have symptoms for at least 12 weeks — not necessarily in a row — out of the previous 12 months.
How Do You Prevent Aerophagia With CPAP?
Doctors may try several methods to improve your aerophagia symptoms while using CPAP therapy.
Adjust CPAP Pressure
Reducing the total amount of air entering the body is one way to protect against aerophagia, but it can be counterproductive if the low air pressure causes a rebound in apnea symptoms.
To work around this problem, some researchers have proposed switching to an automatic positive airway pressure (APAP) device, which adjusts air pressure throughout the night as needed. Initial research suggests this switch can relieve symptoms of bloating, flatulence, belching, and abdominal pain without negatively affecting OSA treatment.
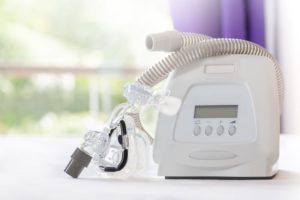
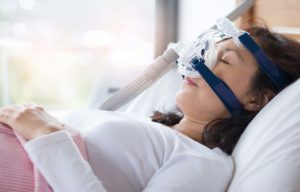
Change Mask
Some researchers believe that full face CPAP masks may cause more aerophagia symptoms than nasal masks. Using a mask that covers both the nose and the mouth may leave you more susceptible to leaks, and the larger mask may require higher pressure. Your doctor can help you find a mask that seals properly and allows you to receive the air you need, according to whether you primarily breathe through your mouth or nose.
If adjusting pressure on your CPAP device or switching you to a nasal mask does not ease your aerophagia, talk to your doctor about alternate options to treat your OSA. They may suggest a bi-level positive airway pressure (BiPAP) device instead, as this type of device offers lower pressure during exhalation.
Are There Other Treatments for Aerophagia?
Aerophagia usually improves with certain lifestyle changes. Depending on what is causing your aerophagia symptoms, your doctor may recommend:
- Changing the way you swallow
- Practicing breathing exercises
- Taking medications
- Avoiding carbonated beverages, drinking straws, and chewing gum
- Eating more slowly
- Undergoing speech therapy to minimize air swallowing
- Behavioral therapy or psychotherapy for anxiety
- Biofeedback therapy (using monitoring equipment to improve breathing and swallowing)
- Stress reduction techniques
In rare cases, a person may swallow so much air that they risk twisted organs and breathing difficulties. In these cases, doctors may siphon out the extra air using a tube through the nose and administer sedatives as a short-term method of reducing air swallowing.
Frequently Asked Questions
Is aerophagia dangerous?
Aerophagia is usually not dangerous, but its symptoms like belching and flatulence can be uncomfortable. It can be managed with lifestyle changes or medical treatment. In very rare cases, severe aerophagia can lead to complications such as bowel obstruction, twisted organs, or breathing difficulties that require immediate medical attention.
What’s the best CPAP mask for aerophagia?
Nasal masks may cause less aerophagia than full-face masks. Full-face masks typically require higher air pressure and may be prone to leaks, which can increase the risk of aerophagia. Your healthcare provider can help you find the best mask for your needs based on whether you breathe through your nose or mouth, and your specific pressure needs.
How can you tell if it’s indigestion or aerophagia?
You can often determine whether you’re experiencing indigestion or aerophagia by looking for distinguishing symptoms. Aerophagia involves frequent belching and noticeable air swallowing, while indigestion causes heartburn and nausea. However, both conditions can cause bloating, flatulence, and abdominal discomfort. If you are having trouble telling the difference, your healthcare provider can evaluate you and order tests, such as abdominal x-rays.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of product specialists, sleep health professionals, and people just like you. Whether you’re searching for the perfect mattress or need expert sleep advice, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
8 Sources
-
Hillamaa A, Mustonen T, Bachour A. Gastrointestinal symptoms and CPAP-related aerophagia A questionnaire study. Sleep Breath. 2025;29(3):197. Published 2025 May 23. doi:10.1007/s11325-025-03360-w
https://pubmed.ncbi.nlm.nih.gov/40407970/ -
Nishida T, Higaki Y, Watabe K. Persistent Nausea and Gastrointestinal Distention: A Case Report of Aerophagia. Cureus. 2023;15(12):e50070. Published 2023 Dec 6. doi:10.7759/cureus.50070
https://pmc.ncbi.nlm.nih.gov/articles/PMC10772479/ -
Shirlaw, T., Hanssen, K., Duce, B., & Hukins, C. (2017). A randomized crossover trial comparing autotitrating and continuous positive airway pressure in subjects with symptoms of aerophagia: Effects on compliance and subjective symptoms. Journal of Clinical Sleep Medicine, 13(7), 881–888.
https://pubmed.ncbi.nlm.nih.gov/28558864/ -
Bredenoord A. J. (2013). Management of belching, hiccups, and aerophagia. Clinical Gastroenterology and Hepatology: The Official Clinical Practice Journal of the American Gastroenterological Association, 11(1), 6–12.
https://pubmed.ncbi.nlm.nih.gov/22982101/ -
Shepherd, K., Hillman, D., & Eastwood, P. (2013). Symptoms of aerophagia are common in patients on continuous positive airway pressure therapy and are related to the presence of nighttime gastroesophageal reflux. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 9(1), 13–17.
https://pubmed.ncbi.nlm.nih.gov/23319899/ -
A.D.A.M. Medical Encyclopedia. (2021, September 1). Small bowel obstruction – x-ray. MedlinePlus.
https://medlineplus.gov/ency/imagepages/3069.htm -
Genta, P. R., Grad, G. F., & Herculano, S. (2017). Aerophagia during CPAP for OSA: The case for auto-CPAP and nasal mask. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 13(7), 859–860.
https://pubmed.ncbi.nlm.nih.gov/28633717/ -
Chiarioni G, Whitehead WE. The role of biofeedback in the treatment of gastrointestinal disorders. Nat Clin Pract Gastroenterol Hepatol. 2008;5(7):371-382. doi:10.1038/ncpgasthep1150
https://pubmed.ncbi.nlm.nih.gov/18521115/