When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
What Does CPAP Stand For? And Other PAP Acronyms
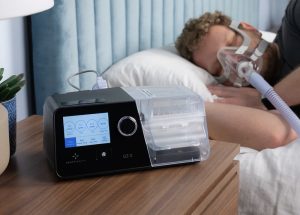
- CPAP stands for continuous positive airway pressure, a type of therapy that pumps a continuous stream of pressurized air into the user’s airway in order to keep it open while they sleep.
- APAP stands for automatic positive airway pressure. An APAP machine adjusts the pressure of the air pumped through the user’s airway based on their breathing patterns.
- BiPAP stands for bilevel positive airway pressure. BiPAP machines alternate between pumping higher pressure air for inhales and lower pressure air for exhales.
- EPAP stands for expiratory positive airway pressure. This is when a small valve attached to the nostrils prompts physical changes to help airways stay open without the use of electricity.
People who have been diagnosed with obstructive sleep apnea (OSA) may first feel overwhelmed by numerous treatment options and acronyms like CPAP, APAP, BiPAP, and EPAP. However, most treatment options have the same basic purpose – to keep the blocked or collapsed airways open, working to address the primary cause of OSA. Each form of therapy just goes about it in different ways.
To help you decide which treatment is best for you, we will discuss the different types of positive airway pressure (PAP) therapies and their acronyms, the pros and cons of each, and how to talk to your doctor about your sleep apnea diagnosis and get the treatment you need.

Exploring CPAP Machines — But Haven’t Been Tested Yet?
Start with our easy, at-home sleep test. It’s stress-free and effective. Get results within a few days.
What Does CPAP Stand For?
CPAP stands for continuous positive airway pressure and designates a specific type of positive airway pressure (PAP) therapy. A CPAP machine emits a continuous stream of pressurized air at a fixed rate. The air is directed through a mask so that a user’s upper airways remain open during both inhalation and exhalation. Pressure is adjustable on a CPAP machine, but it remains constant throughout the night once set. Most CPAP machines have pressure settings between 4 and 20 cm H2O.
What Are the Other Types of PAP Therapy?
A CPAP machine is most commonly prescribed for OSA, but it is not the only type of PAP therapy. APAP and BiPAP machines can also be effective treatments.
Some people respond better to certain PAP therapies more than others. Your doctor can advise you on the most appropriate treatment for your needs.
APAP
Automatic positive airway pressure (APAP) machines adjust the amount of pressure delivered based on a user’s breathing rates. CPAP machines deliver constant pressure, but the set level is adjustable.
- Who’s a Match for APAP Therapy: By sensing subtle changes in breath resistance, APAP machines can address the needs of severe or unstable breathing conditions. APAP machines optimize therapeutic results by adjusting to the variable pressure needs of different sleep stages and sleep positions. Body weight affects pressure demands, which allows APAP machines to accommodate changes in weight better than a CPAP machine.
- Who APAP Therapy May Not Work For: APAP therapy is not recommended for people with central sleep apnea (CSA), congestive heart failure, COPD, obesity hypoventilation syndrome, or drug-related sleep apnea. It’s also not appropriate for people who find masks too uncomfortable to maintain regular therapy.
BPAP or BiPAP
Unlike a CPAP machine, a bilevel positive airway pressure (BiPAP or BPAP) machine has two different pressure settings to help regulate breathing. Higher pressurized air is pumped out while inhaling, while less pressure is delivered during exhalation.
BiPAP therapy is often used as treatment for people with OSA who don’t tolerate CPAP machines. Many people experience less discomfort and dryness when exhaling on a lower pressure setting.
BiPAP machines have a wider pressure range than CPAP and APAP machines. The typical BiPAP range is between 4 and 30 cm H2O.
- Who’s a Match for BPAP or BiPAP Therapy: BiPAP therapy is used to treat congestive heart failure, central sleep apnea, complex sleep apnea, COPD, and breathing disorders that require higher pressure levels. People who have difficulty exhaling on CPAP machines may have more success with BiPAP machines.
- Who BPAP or BiPAP Therapy May Not Work For: BiPAP therapy is not recommended for people who have had recent facial surgery, or for those with altered mental status, life-threatening hypoxemia, irregular heartbeat, or respiratory secretions. BiPAP machines are the most expensive PAP device, so they may be cost-prohibitive for some people.
EPAP
Unlike CPAP therapy, expiratory positive airway pressure (EPAP) therapy treats OSA without using machines or electricity. The EPAP device consists of a small valve that attaches to the nostrils. The user’s exhales create pressure that helps keep airways open.
EPAP treatment is still considered an emerging therapy, but numerous studies have found it effective for treating OSA. Studies suggest that it also boasts impressive patient adherence rates. It may be especially useful for those who can’t tolerate side effects of CPAP therapy and those who find it difficult to maintain CPAP therapy adherence over time.
- Who’s a Match for EPAP Therapy: EPAP therapy may be a good alternative for people who resist CPAP therapy because of negative side effects or maintenance. EPAP devices are quiet, unobtrusive, and easy to maintain. They can also be a good choice for people who travel often, as they are portable and require no battery or electricity.
- Who EPAP Therapy May Not Work For: Since the EPAP device attaches to the nostrils, those who breathe through their mouths may not benefit. Also, CPAP therapy is still considered the gold standard for treating OSA, so those who don’t have problems with this treatment should likely stick with it. Note that insurance is less likely to cover EPAP therapy, so while its base price is lower, it may end up costing more.
ASV
Adaptive servo-ventilation (ASV) machines keep the user’s breathing stable throughout the night by monitoring the breath and adjusting the air pressure accordingly. While the equipment itself – a mask connected to a machine by a tube – is similar to PAP machines, ASV machines’ monitoring and pressure adjustment are considerably more advanced than even BiPAP machines.
ASV therapy has been found effective for people experiencing central sleep apnea in addition to OSA, also known as complex sleep apnea, or treatment-emergent central sleep apnea.
- Who’s a Match for ASV Therapy: While it has been found effective against OSA alone, people with complex sleep apnea are the best candidates for ASV therapy. It has also been shown to be effective treating sleep apnea induced by narcotics, which can help those who are prescribed opioids for pain. Those with systolic heart failure with preserved ejection fraction may also benefit.
- Who ASV Therapy May Not Work For: ASV machines may pose risks to users with a certain type of congestive heart failure that affects pumping, called reduced ejection fraction. Your doctor will determine whether to proceed with treatment in these cases. Also, since it carries many of the same potential side effects as PAP therapies, those who have OSA but no central sleep apnea typically opt for PAP treatment.
Which Type of PAP Therapy Is Right for You?
Your doctor will help you determine which type of PAP therapy is best for your needs and preferences, but understanding each type will help you have a more informed conversation.
CPAP therapy will be the starting point for most people.
However, if you know that you change positions often while sleeping or have responded poorly to CPAP therapy in the past, you may want to try APAP therapy so that the pressure adjusts to your breathing needs. Similarly, if you know you have additional breathing disorders or heart problems, you may look more closely at BiPAP therapy, which lowers its air pressure on the exhale. For ASV therapy, a doctor will typically advise whether this more specialized treatment is necessary.
Those with claustrophobia or trouble sleeping with headgear or noise may consider EPAP therapy, since it is quiet and doesn’t cover the face.
Sometimes it takes a little trial and error to find the best treatment. However, OSA is associated with adverse health conditions like cardiovascular disease, stroke, and diabetes, so it’s important to address it. If you have trouble with the first type of therapy you try, don’t hesitate to visit your doctor again to discuss alternatives.
Who’s a Match for CPAP Therapy
CPAP therapy is the first-line treatment for sleep apnea, so most people with OSA start off using a CPAP machine.
Regular CPAP treatment can help control high blood pressure, decrease or eliminate snoring, lower the risk of stroke, improve cognitive function, and reduce daytime sleepiness. CPAP therapy can also lower the risk of heart failure in people over the age of 60.
CPAP therapy is sometimes used to treat severe chronic obstructive pulmonary disease (COPD) and can also reduce mortality rates in those with COPD.
Since CPAP machines are typically less expensive than other PAP machines, they may be more accessible for some people. This is particularly true if you’re not eligible for insurance coverage or if you have a high deductible. Insurance providers are also more likely to cover CPAP equipment when compared to other PAP devices.
Who CPAP Therapy May Not Work For
It can take time to adjust to CPAP therapy, and not everyone will adapt to the treatment. CPAP therapy is not recommended for those who have had esophageal or gastric surgery or for people with anxiety, claustrophobia, severe asthma, air leak syndrome, or severe nasal congestion. CPAP therapy also isn’t as effective for people over 80 years old who have moderate to severe OSA.
How to Talk to Your Doctor About PAP Therapy
Ultimately, your doctor chooses the best treatment for you. But with a little bit of preparation, you can help guide the decision and make sure that they address your needs and preferences.
The first appointment: Pull together a list of your symptoms and note what’s bothering you the most (daytime sleepiness, snoring, morning headaches, etc.). Before prescribing any type of PAP therapy, the doctor will likely order a sleep study.
The diagnosis/prescription: Familiarize yourself with the different types of PAP therapy, and note any additional medical conditions or lifestyle factors to bring up. For example, if you travel often or experience severe claustrophobia, make sure to tell the doctor. Check with your insurance company about what treatments are covered and the requirements for coverage – if you know what is and is not covered, it may affect what the doctor chooses to prescribe.
The treatment: Once you determine your treatment course, set a follow-up appointment to discuss your progress. Do not hesitate to see your doctor sooner if you experience negative side effects that affect your ability to stick to the treatment plan.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of product specialists, sleep health professionals, and people just like you. Whether you’re searching for the perfect mattress or need expert sleep advice, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
5 Sources
-
Berry, R. B., Kryger, M. H., & Massie, C. A. (2011). A novel nasal expiratory positive airway pressure (EPAP) device for the treatment of obstructive sleep apnea: A randomized controlled trial. Sleep, 34(4), 479–485.
https://pubmed.ncbi.nlm.nih.gov/21461326/ -
Lorenzi-Filho, G., Almeida, F. R., & Strollo, P. J. (2017). Treating OSA: Current and emerging therapies beyond CPAP. Respirology (Carlton, Vic.), 22(8), 1500–1507.
https://pubmed.ncbi.nlm.nih.gov/28901030/ -
Liu, Y., Ying, Y., Pandu, J. S., Wang, Y., Dou, S., Li, Y., & Ma, D. (2019). Efficacy and safety assessment of expiratory positive airway pressure (EPAP) mask for OSAHS therapy. Auris, Nasus, Larynx, 46(2), 238–245.
https://pubmed.ncbi.nlm.nih.gov/30262209/ -
Iftikhar, I. H., Bittencourt, L., Youngstedt, S. D., Ayas, N., Cistulli, P., Schwab, R., Durkin, M. W., & Magalang, U. J. (2017). Comparative efficacy of CPAP, MADs, exercise-training, and dietary weight loss for sleep apnea: A network meta-analysis. Sleep medicine, 30, 7–14.
https://pubmed.ncbi.nlm.nih.gov/28215266/ -
Patel A, Perez I, Rabiei-Samani S. What Is Adaptive Servo-Ventilation (ASV)?. Am J Respir Crit Care Med. 2021;204(2):P3-P4. doi:10.1164/rccm.2042P3
https://www.thoracic.org/patients/patient-resources/resources/adaptive-servo-ventilation-asv.pdf