When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Sleep Studies
- A sleep study, known as polysomnography, monitors and records various body functions during sleep.
- Sleep studies help diagnose sleep disorders like sleep apnea, restless legs syndrome, and narcolepsy.
- Sleep studies typically observe brain activity, eye movement, heart rate, and breathing patterns.
- A sleep study can be performed in specialized centers or at home, depending on the situation.
If your doctor suggests you undergo a sleep study, or polysomnography, you may be wondering what is involved in this test and what to expect. Sleep studies help doctors diagnose sleep disorders such as sleep apnea, periodic limb movement disorder, narcolepsy, restless legs syndrome, insomnia, and nighttime behaviors like sleepwalking and REM sleep behavior disorder. Often these disorders cannot be identified with a normal office visit—your doctor needs to gather more conclusive evidence while you’re asleep.
What Is a Sleep Study?
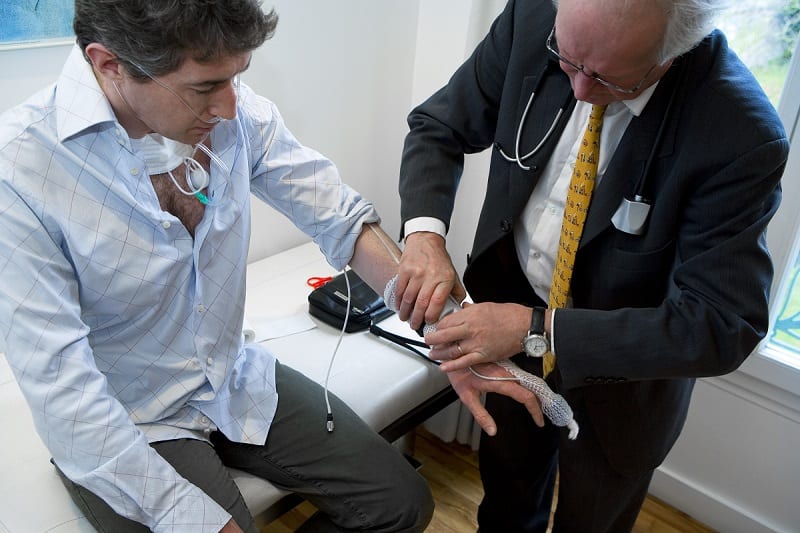
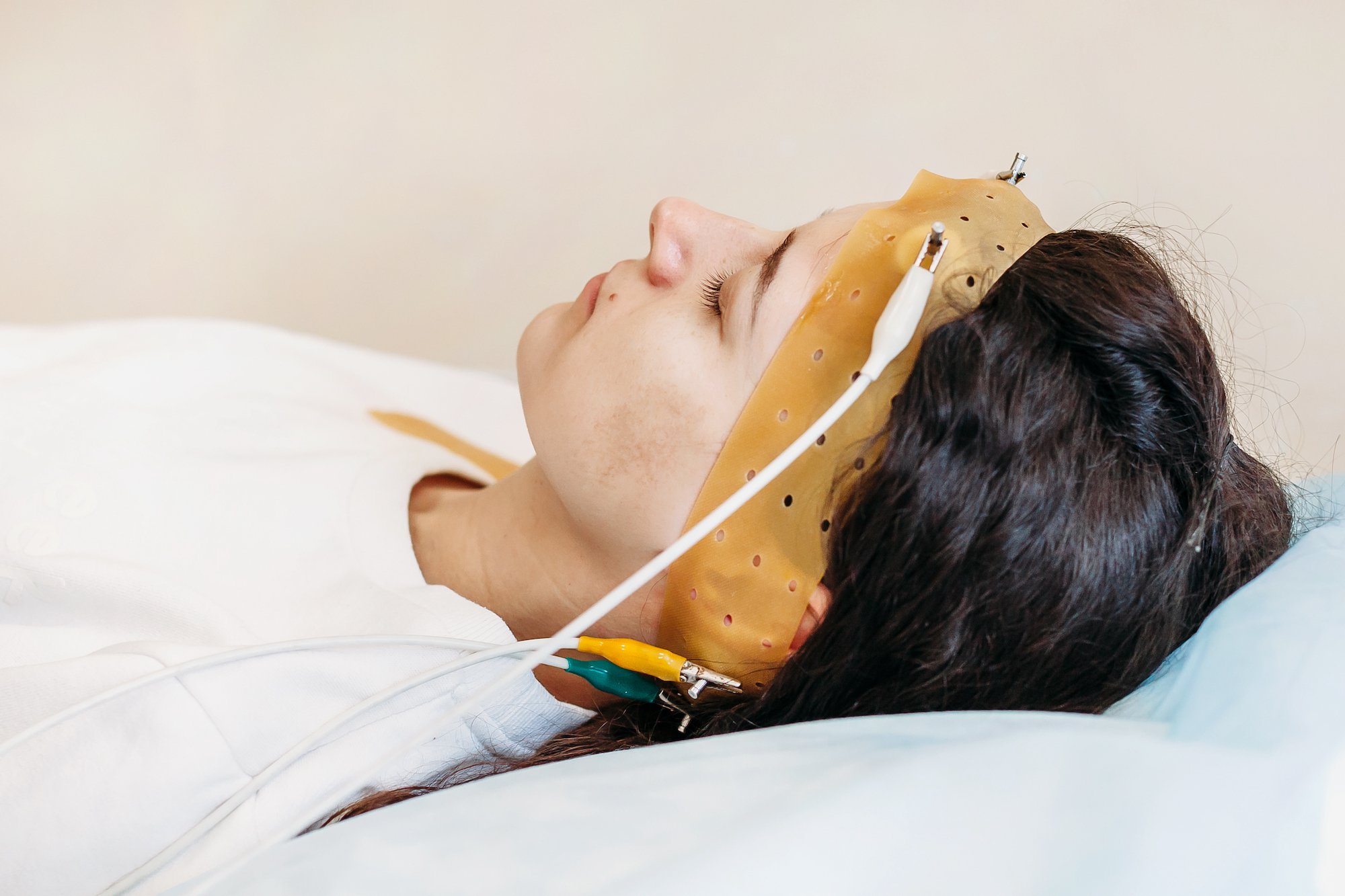
A sleep study is a non-invasive, overnight exam that allows doctors to monitor you while you sleep to see what’s happening in your brain and body. For this test, you will go to a sleep lab that is set up for overnight stays—usually in a hospital or sleep center. While you sleep, an EEG monitors your sleep stages and the cycles of REM and non-REM or NREM sleep you go through during the night, to identify possible disruptions in the pattern of your sleep. A sleep study will also measure things such as eye movements, oxygen levels in your blood (through a sensor—there are no needles involved), heart and breathing rates, snoring, and body movements.
The data from your sleep study will usually be taken by a technologist, and later evaluated by your doctor. This may take up to two weeks, when you’ll schedule a follow up to discuss the results.
Types of Sleep Studies
Sleep studies collect data about what is happening in a person’s body during sleep. Different types of sleep studies are available depending on one’s symptoms and the sleep disorders that may be present.
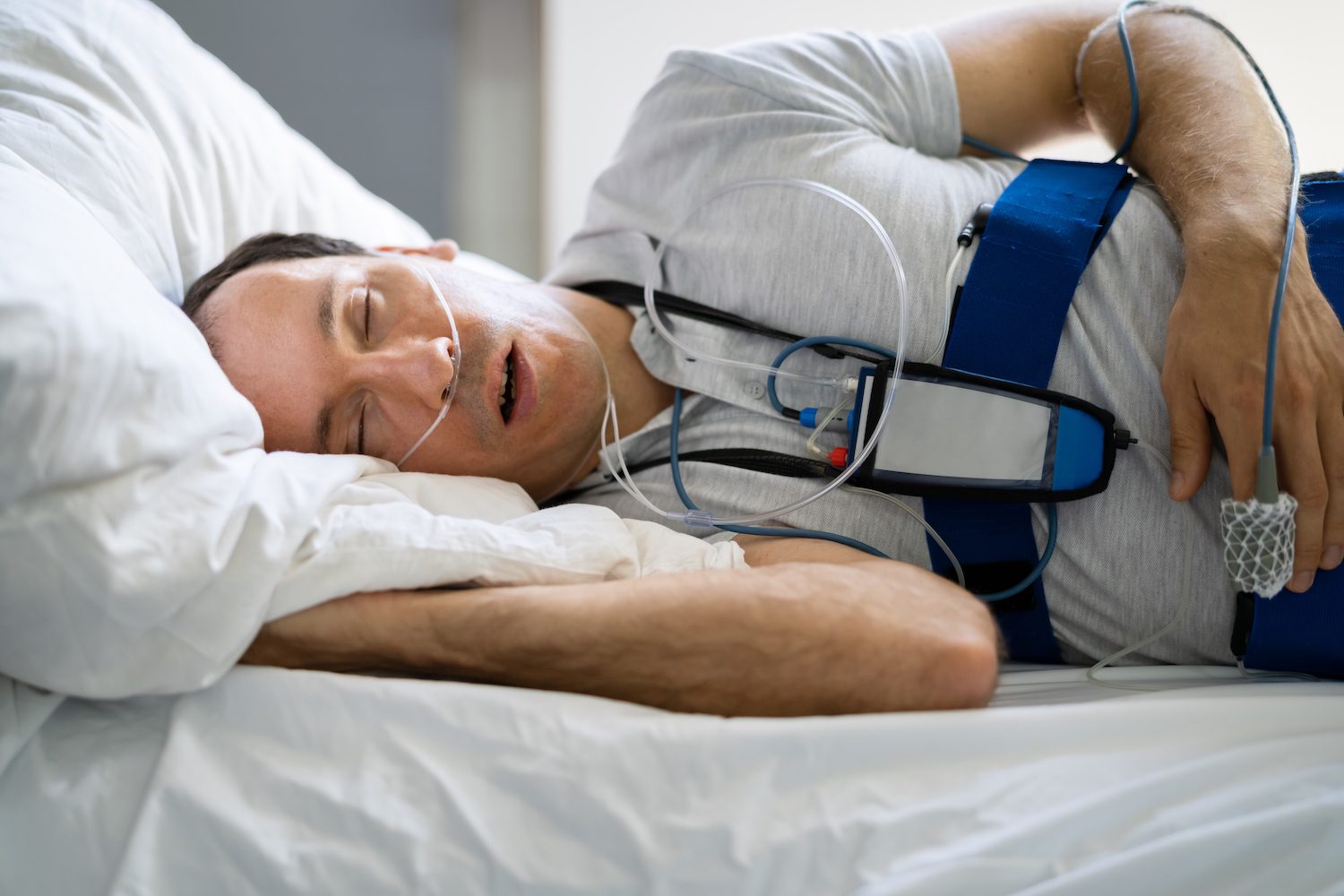
- Polysomnography: In polysomnography, a sleep technician monitors a patient who stays overnight at a specialized clinic. A variety of functions are measured throughout the night, including eye movements, brain and muscle activity, respiratory effort and airflow, blood oxygen levels, body positioning and movements, snoring, and heart rate.
- Multiple Sleep Latency Test: Multiple sleep latency testing measures how quickly someone falls asleep and how quickly they enter REM sleep during daytime naps. This test is primarily used to diagnose excessive daytime sleepiness that may be due to narcolepsy or an unknown cause (idiopathic hypersomnia).
- CPAP Titration: Continuous positive airway pressure (CPAP) is a common treatment for sleep apnea. In CPAP titration, a technologist determines the amount of air pressure that patient needs from their CPAP so that their machine can be properly programmed for home use. CPAP titration usually requires a second sleep study. When sleep apnea is strongly suspected, a split-night sleep study may be an option. In a split-night study, polysomnography is used to diagnose sleep apnea during the first half of the night, and CPAP titration is performed during the second half of the night.
- Home Sleep Apnea Testing: Home sleep apnea testing collects data about a patient’s breathing, heart rate, and other variables overnight. However, compared with polysomnography, home testing provides less information, and the process is not overseen by a technologist.
What Can a Sleep Study Diagnose?
A sleep study is used to diagnose many sleep disorders, including:
- Insomnia
- Sleep Apnea
- Restless Leg Syndrome
- Narcolepsy
- Periodic Limb Movement Disorder
- Sleepwalking
- Sleep Talking
- REM Sleep Behavior Disorder
Who Needs a Sleep Study?
Sleep studies are a vital diagnostic tool for many sleep disorders, but they aren’t necessary in all cases. A doctor can prescribe a sleep study depending on a person’s symptoms and overall health.
Talk with your doctor if you are experiencing sleep issues or daytime symptoms such as fatigue, drowsiness, depression, or difficulty concentrating. Patients with obesity with sleep issues should be screened for sleep apnea. Your doctor can help you determine whether a sleep study is right for you.
If you have been diagnosed with a sleep disorder and your symptoms are not improving with treatment, a follow-up sleep study can help your doctor determine the next steps for your care.
How Much Does a Sleep Study Cost?
The cost of a sleep study is difficult to estimate. It depends on the type of testing being used and what a facility charges. Small clinics typically charge less compared to big hospital systems. It’s important to speak directly with the clinic administering your sleep study for the most accurate information.
Insurance Coverage for a Sleep Study
The costs you are responsible for depends on what your insurance covers. Contact your insurance provider to learn about sleep study coverage provided by your plan.
If your doctor suggests a sleep study for you, but your insurance provider denies coverage for the test, it could help to ask about appealing the denial of coverage. This typically involves providing documentation as to why the test is medically necessary. Your doctor can help you put together the paperwork required to file an appeal.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
3 Sources
-
Schwab, R. J. (2020, June). Merck Manual Professional Version: Approach to the Patient with a Sleep or Wakefulness Disorder., Retrieved September 28, 2020, from
https://www.merckmanuals.com/professional/neurologic-disorders/sleep-and-wakefulness-disorders/approach-to-the-patient-with-a-sleep-or-wakefulness-disorder -
BaHammam, A. S., ALAnbay, E., Alrajhi, N., & Olaish, A. H. (2015). The success rate of split-night polysomnography and its impact on continuous positive airway pressure compliance. Annals of thoracic medicine, 10(4), 274–278.
https://pubmed.ncbi.nlm.nih.gov/26664566/ -
Epstein, L. J., Kristo, D., Strollo, P. J., Jr, Friedman, N., Malhotra, A., Patil, S. P., Ramar, K., Rogers, R., Schwab, R. J., Weaver, E. M., Weinstein, M. D., & Adult Obstructive Sleep Apnea Task Force of the American Academy of Sleep Medicine (2009). Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine, 5(3), 263–276.
https://pubmed.ncbi.nlm.nih.gov/19960649/