Do We Lose Sleep to Seasonal Affective Disorder?
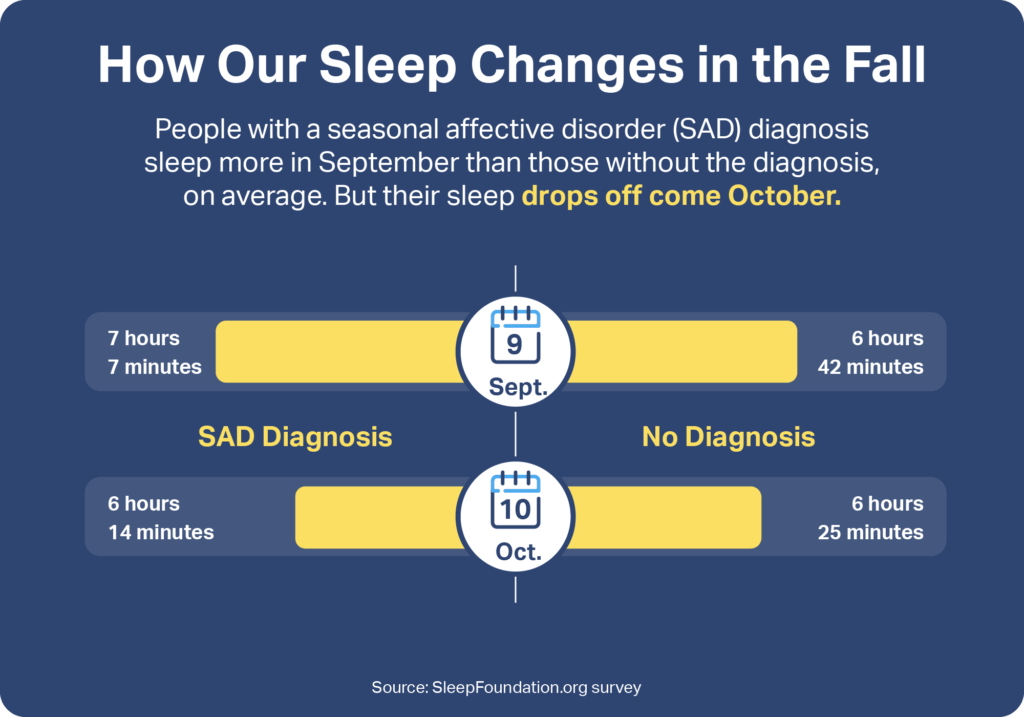
- People with seasonal affective disorder (SAD) sleep 52.9 minutes less in October than in September, according to a survey.
- 70.9% of respondents with SAD also have a sleep disorder, compared to 26.9% of respondents without SAD.
- 58.2% of respondents with SAD reported using sleep aids in the past month, compared to 26.3% of those without SAD.
- 70% of respondents with SAD feel tired in the winter, compared to 44.2% of those without it.
- SAD affects as much as 3% of the U.S. population.
The end of daylight saving time on Nov. 6 signals the beginning of shorter, darker winter days. It also can trigger symptoms of seasonal affective disorder for some people.
Seasonal affective disorder, or SAD, is “a condition in which people experience many symptoms often seen in depression but during times of shorter daylight,” says Dr. Alex Dimitriu, founder of Menlo Park Psychiatry & Sleep Medicine, in Menlo Park, California, and a SleepFoundation.org medical-review panel member. It affects as much as 3% of people in the U.S., with low energy, lack of concentration, irritability, and sleeping issues among the symptoms, he says.
Although some may experience it in the summer, seasonal depression is more common in the fall and winter. When sunlight becomes scarce and we’re feeling fatigued, we may want to get cozy and sleep.
“You might think, ‘If I’m still tired, I’ll get more sleep,’ but with SAD, the answer isn’t always more sleep,” says Dr. Norman E. Rosenthal, a clinical professor of psychiatry at Georgetown School of Medicine in Washington, D.C., who first coined the term “seasonal affective disorder” in the 1980s. “Lying in bed for longer within a dark room with covers over your head is not recommended.”
It might be what some of us are doing this time of year.
In an October 2022 SleepFoundation.org survey of 1,250 U.S. adults, respondents with SAD reported getting 52.9 minutes less sleep in October than in September. They slept less in October than respondents without a diagnosis, despite sleeping more in September. Some 70.9% of people with SAD also reported having a sleep disorder, compared to 26.9% of people without a SAD diagnosis.
As we try to understand more about how we sleep, here’s a look at how the changing seasons and related conditions play into it.
What Role Does Light Play in Seasonal Affective Disorder?
There’s science behind those vitamin D-boosting lamps or light boxes you may see folks buying. Research suggests that low sunlight is a key factor in SAD . Insufficient light exposure can delay or disrupt our internal clocks, or circadian rhythms.

The transition from daylight saving time can exacerbate this issue, says Dr. Chris Winter, owner of Charlottesville Neurology & Sleep Medicine in Charlottesville, Virginia. Waking up when it’s dark out can contribute to feelings of sleepiness and fatigue, he says, taking a real toll on emotional and physical health.
“(Seasonal affective disorder) really is about the perception of light.” — Dr. Chris Winter, Charlottesville Neurology & Sleep Medicine
Dr. Winter says this is because light heavily influences our physiology.
“SAD really is about the perception of light,” he says. “It causes an imbalance in our circadian rhythm, which doesn’t just control sleep. It oversees hormone release, body temperature, and even blood cell production.”
That may be why 57.7% of survey respondents with SAD reported feeling tired during the fall months compared to 48% in the spring. That increased to 70% during the winter months, when days are at their shortest. Meanwhile, people without a SAD diagnosis reported feeling most tired in the summer.
Bach, a 32-year-old who lives in Illinois and prefers to go by her first initial, has experienced this seasonal shift. She was officially diagnosed with SAD in 2017 but says she has felt its effects for a decade.
“I start seeing symptoms in October, and they usually let up by sometime in April,” Bach says. “For me, it’s a lack of energy and interest in pretty much anything, and waking up is a problem.”
It can also be a problem for people who live in areas where the sun sets as early as 4 p.m. during those short winter months.
Where Is SAD Most Common?
Winter days can be coldest and darkest in northern states that are farthest from the equator , thanks to the Earth’s tilt causing a lack of direct sunlight. That’s why we have different seasons, after all.
According to the Centers for Disease Control and Prevention’s North America Land Data Assimilation System, which measures the average daily sunlight in the lower 48 states, the least amount of winter sunlight is in the Northeast and Upper Midwest states.
Do folks living in states with less sunlight have higher instances of SAD? And do they sleep differently?
Among survey respondents, 24.4% of people in low-sunlight states had a SAD diagnosis, compared to 15.2% in states with the most sunlight. More than half, or 51.2%, of low-sunlight-state residents felt tired in the fall, compared to 42.2% in high-sunlight states. In the winter, those percentages changed to 50.5% and 40%, respectively.
Meanwhile, 41.7% of people in low-sunlight states had a diagnosed sleep disorder, compared to 38.6% in high-sunlight-states. All, however, had nearly the same sleep latency, or the time it takes to fall asleep.
What Does SAD Mean for Our Sleep?
The sleep story among people with SAD may be one of quantity and quality.
They clock an average of 7 hours and 7 minutes of sleep in September. By early October, that number slips to 6 hours and 14 minutes, which is less than the recommended minimum of seven hours of sleep . By comparison, people without SAD averaged 6 hours and 42 minutes of sleep in September and 6 hours and 25 minutes in early October, a difference of 17 minutes.
Sleeping too little or too much comes down to a lack of restorative sleep, says Dr. Rosenthal, who has studied the quality of sleep in people with SAD .
“They’re missing deep sleep,” he says. “They’re not feeling refreshed.”
In people with SAD, 40.1% of people reported a diagnosis of insomnia, with 24.7% having sleep apnea and 18.5% having restless legs syndrome. Among those without the diagnosis, 14.6% have insomnia, 7.6% have sleep apnea, and 6.1% have restless legs syndrome.
Dr. Rosenthal says that there aren’t studies definitively linking sleep disorders with SAD. But they share things in common.
“[Sleep disorders and SAD] are all aspects of the same dysregulation,” he says.
How Do You Treat SAD?
For many, managing SAD with therapies and lifestyle shifts is key. Some 40.5% of survey respondents with SAD spend their summers in a different location than their winters, compared to just 14% of those without a SAD diagnosis.
Prescriptions and sleep aids are also go-to treatments. Among survey respondents with SAD, more than half (58.2%) reported using sleep aids in the past month. Meanwhile, 37% of people take antidepressants for SAD, 23.8% treat it by changing their sleep regimen, and 15.4% don’t treat it at all.
Experts say staying active and knowing your triggers are good ways to figure out the plan that works best for you. Dr. Dimitriu and Dr. Winter recommend going outside for morning sun and exercise if possible.
“Exercise intrinsically benefits neurotransmitter release to ward away depression,” Dr. Winter says.
If you can’t get real sunlight, the next best bet is a sun lamp or light box, says Dr. Rosenthal, who pioneered the use of light therapy to treat SAD. A higher percentage of respondents say they discontinued light therapy (25.1%) to treat seasonal affective disorder than those who use it currently (21.2%), however.
Dimitriu also suggests supplementing with vitamin D to make up for what you’re not getting from sunlight and looking into cognitive behavioral therapy (CBT).
Antidepressants are another option. They take one to two weeks to start working, if not longer .
Whatever treatment you choose, Dr. Rosenthal says it is also good to accept that SAD happens.
“You change what you can, and you control what you can,” he says. “But you have to realize that sometimes the winter is not going to feel as great as the summer.”
Methodology
The survey commissioned by SleepFoundation.org was conducted on the online survey platform Pollfish on Oct. 2, 2022. Results are from 1,250 survey participants who were ages 18 and older and lived in the United States at the time of the survey. All attested to answering the survey questions truthfully and accurately.
References
10 Sources
-
Melrose S. (2015). Seasonal Affective Disorder: An Overview of Assessment and Treatment Approaches. Depression research and treatment, 2015, 178564.
https://pubmed.ncbi.nlm.nih.gov/26688752/ -
National Library of Medicine. MedlinePlus. (May 1, 2019) Seasonal Affective Disorder., Retrieved October 26, 2022.
https://medlineplus.gov/genetics/condition/seasonal-affective-disorder/#frequency -
American Academy of Sleep Medicine. (February 19, 2020) How seasonal affective disorder disrupts sleep., Retrieved October 26, 2022.
https://sleepeducation.org/how-seasonal-affective-disorder-disrupts-sleep/ -
Wescott, D. L., Soehner, A. M., & Roecklein, K. A. (2020). Sleep in seasonal affective disorder. Current opinion in psychology, 34, 7–11.
https://pubmed.ncbi.nlm.nih.gov/31536962/ -
Hansen, Bertel T.; Sønderskov, Kim M.; Hageman, Ida; Dinesen, Peter T.; Østergaard, Søren D., Daylight Savings Time Transitions and the Incidence Rate of Unipolar Depressive Episodes. Epidemiology: May 2017 – Volume 28 – Issue 3 – p 346-353
https://journals.lww.com/epidem/fulltext/2017/05000/daylight_savings_time_transitions_and_the.7.aspx -
Watson, N. F., Badr, M. S., Belenky, G., Bliwise, D. L., Buxton, O. M., Buysse, D., Dinges, D. F., Gangwisch, J., Grandner, M. A., Kushida, C., Malhotra, R. K., Martin, J. L., Patel, S. R., Quan, S. F., & Tasali, E. (2015). Recommended Amount of Sleep for a Healthy Adult: A Joint Consensus Statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep, 38(6), 843–844.
https://pubmed.ncbi.nlm.nih.gov/26039963/ -
Rosenthal, N. E., Sack, D. A., Gillin, J. C., Lewy, A. J., Goodwin, F. K., Davenport, Y., Mueller, P. S., Newsome, D. A., & Wehr, T. A. (1984). Seasonal affective disorder. A description of the syndrome and preliminary findings with light therapy. Archives of general psychiatry, 41(1), 72–80.
http://archpsyc.jamanetwork.com/article.aspx?doi=10.1001/archpsyc.1984.01790120076010 -
U.S. Department of Health and Human Services, National Institutes of Health, National Institute of Mental Health. Seasonal Affective Disorder., Retrieved October 26, 2022
https://www.nimh.nih.gov/health/publications/seasonal-affective-disorder -
Nussbaumer-Streit, B., Forneris, C. A., Morgan, L. C., Van Noord, M. G., Gaynes, B. N., Greenblatt, A., Wipplinger, J., Lux, L. J., Winkler, D., & Gartlehner, G. (2019). Light therapy for preventing seasonal affective disorder. The Cochrane database of systematic reviews, 3(3), CD011269.
https://pubmed.ncbi.nlm.nih.gov/30883670/ -
InformedHealth.org. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); (Updated June 18, 2020). Depression: How effective are antidepressants?, etrieved October 26, 2022
https://www.ncbi.nlm.nih.gov/books/NBK361016/