When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Light and Sleep
Light is the most important external factor affecting sleep. While most people intuitively know that it’s easier to sleep when it’s dark, the link between light and sleep goes much deeper.
Light plays a central role in regulating circadian rhythm, the body’s internal clock that signals when to be alert and when to rest. Light also affects the production of melatonin, an essential sleep-promoting hormone.
Daily light exposure, including the type of light we see as well as when and how long we’re exposed to it, has a critical effect on sleep. Learning about the complex links between light and sleep allows you to set up your bedroom to be more conducive to consistent, high-quality sleep.
How Does Light Affect Sleep?
While human biology evolved with sleep following the daily patterns of sunlight and darkness, ubiquitous electricity makes 24/7 illumination possible. From streetlights to office lighting to cell phones, artificial light is a constant part of modern life and has dramatic effects on sleep, influencing circadian rhythm, melatonin production, and sleep cycles.
Looking to improve your sleep? Try upgrading your mattress.
Circadian Rhythms
Circadian rhythm is a 24-hour internal clock that coordinates a wide range of processes in the body, including sleep. This rhythm is controlled by a small part of the brain, known as the circadian pacemaker, that is powerfully influenced by light exposure.
When light enters the eye, it is sensed by a special group of cells on the retina, which is carried to the brain and interpreted as information about the time of day. The brain then sends signals throughout the body to control organs and other systems in accordance with that time of day.
When exposed to only natural light, a person’s circadian rhythm becomes closely synchronized with sunrise and sunset, staying awake during the day and sleeping when it’s dark. In modern society, though, electricity creates an abundance of light sources that affect the brain’s circadian pacemaker.
Excess or poorly timed artificial light exposure can cause a person’s circadian rhythm to be misaligned with the day-night schedule. This can throw their sleep out-of-whack and induce other concerning health impacts including worsened metabolism, weight gain, cardiovascular problems, and perhaps even an elevated cancer risk. Circadian rhythms are also strongly correlated to mood, mental health, and seasonal affective disorder.

Melatonin
Melatonin is a hormone that is naturally made by the body, and its production is closely tied to light. In response to darkness, the pineal gland in the brain initiates production of melatonin, but light exposure slows or halts that production.
Drowsiness increases with rising melatonin levels, which is one way that this hormone facilitates sleep. In addition, daily cycles of melatonin production normalize circadian rhythm, reinforcing a stable sleep-wake schedule. For some people with sleeping problems supplemental melatonin may be prescribed to help regulate sleep timing.
Sleep Cycles
Not all sleep has the same characteristics. In a normal sleep period, a person goes through four to six sleep cycles, each of which lasts from 70 to 120 minutes. Those cycles are made up of multiple stages of sleep, including both rapid eye movement (REM) and non-REM sleep.
Light exposure at night can hinder transitions between sleep cycles, reducing the quality of sleep. Too much light can cause repeated awakenings, interrupting the sleep cycle and reducing time spent in deeper, more restorative sleep stages.
Circadian Rhythm Disorders
Circadian rhythm sleep-wake disorders occur when a person’s internal clock isn’t functioning properly or becomes misaligned with their environment. Many circadian rhythm disorders are tied to patterns of light exposure.
Jet Lag
Jet lag is a circadian disorder that arises after long-distance plane travel. When confronted with the distinct day-night cycle in the arrival city’s time zone, circadian rhythm can get thrown off-kilter. As a result, a person may struggle to fall asleep, wake up earlier than they want to, or experience excessive daytime sleepiness.
Addressing jet lag usually means acclimating to the new time zone, such as by getting daylight exposure at specific times and avoiding light at certain times to realign circadian rhythm. This process can take several days and up to two weeks.
Shift Work Disorder
Some work schedules, known as shift work, require working into the evening or overnight. Night shifts may be an everyday part of a job or part of a rotating schedule. The Bureau of Labor and Statistics estimates that around 16% of workers in America have evening or overnight shifts.
Shift workers typically have to sleep during the daytime, putting them at high risk of a misaligned circadian rhythm and the development of shift work disorder. This circadian rhythm disorder can cause insufficient sleep, excessive sleepiness at inopportune times, mood problems, and elevated risk of workplace accidents.
Other Circadian Sleep-Wake Disorders
Circadian rhythm disorders can happen when a person’s internal clock gets shifted too far forward or back or if it fails to follow a stable 24-hour schedule. These problems are frequently connected to a person’s daily behavior and light exposure.
One treatment for many circadian disorders is light therapy, which uses sitting close to a high-powered lamp at scheduled times to retrain the body’s internal clock. The strong lamp is meant to mimic daylight and is often used in the morning to normalize circadian timing.
What Types of Light Affect Sleep?
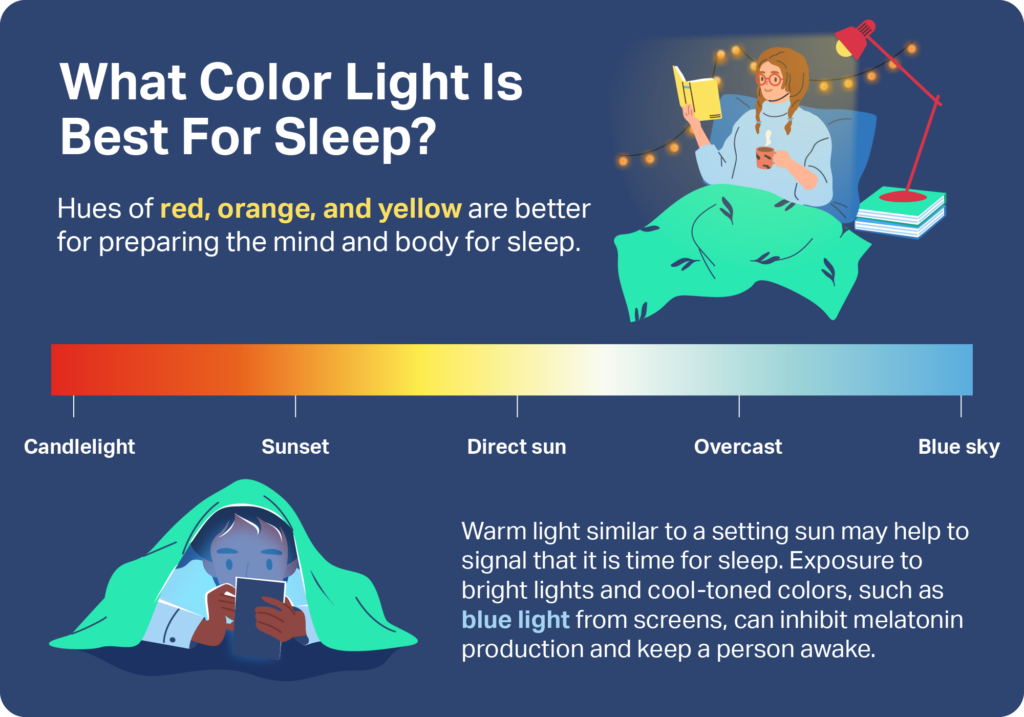
Virtually all light can affect sleep, but not all types of light have the same impact. Daylight, which in direct sunlight has up to 10,000 lux, a unit to measure illuminance, is far more intense than even bright office lighting, which rarely reaches about 500 lux. For this reason, daylight is a profound influence on sleep and circadian timing.
There can be important differences between types of artificial light as well. Some types have more illuminance and brightness. That said, even light that appears to have the same brightness may, in reality, have a different wavelength, changing how it’s perceived by the eye and brain.
For example, blue light has a short wavelength and is emitted by many LEDs. Studies have found that it has a significantly larger effect on melatonin and circadian rhythm than light with a longer wavelength. Many electronic devices, including cell phones, tablets, and laptops, emit blue light, and their extensive evening use can contribute to sleep problems.
Is It Best to Sleep in Pitch Darkness?
As a general rule, it is best to sleep in as much darkness as possible. Pitch darkness reduces potential distractions and disruptions to sleep. Sleeping with a light on interferes with sleep cycles and causes more fragmented sleep, and these downsides may be greatest in the few hours before waking up.
Research demonstrates that closing your eyes isn’t enough ; your eyelids can’t block sufficient light. The effects on circadian rhythm can occur even with low levels of indoor light andclosed eyes.
In addition to sleep quality, there are other reasons why research indicates that it’s best to sleep in pitch darkness:
- Eye strain: Even low levels of ambient light during sleep have been associated with eye strain, resulting in soreness, tiredness, and discomfort in the eyes, as well as greater difficulty focusing.
- Weight gain: Keeping lights on during sleep appears to affect circadian regulation of metabolism, increasing the risk of weight gain even if sleep itself is not disrupted. In one study over a five year period, women who slept with a light or TV on were considerably more likely to gain 10 pounds or more, even after controlling for factors relating to their diet and exercise habits.
- Cancer risk: One observational study found an association between people whose homes had high levels of artificial light at night and their risk of breast and prostate cancers. This study did not demonstrate causation, and further research is necessary to understand this correlation.
The diverse potential consequences of excess artificial light in your bedroom reflect that light exposure may throw off circadian rhythm and its vital role in promoting numerous elements of physical and mental health.
How Can You Adjust Your Bedroom Environment to Get the Best Sleep?
A first step in setting up your bedroom to promote sleep is to make it as dark as possible. Blackout curtains block the majority of external light to foster a darker environment.
When preparing for bed, keep your lights dim. Using a small, low-power lamp can help transition to bedtime and pitch darkness. Low illuminance and warm color temperature may help with relaxation and getting into the right mindset for sleep.
Another step is to reduce or eliminate technology in your bedroom. Screen time can keep your mind stimulated, delaying bedtime, and, at the same time, the light can disrupt circadian timing, melatonin production, and overall sleep. If you can’t get electronics completely out of your bedroom, turn their brightness down as far as possible, try not to use them before bedtime, and keep them silenced during the night.
Lighting a Path to the Bathroom
For many adults, especially older adults at risk of falls, it’s important to be able to see where they are walking when going to the bathroom at night.
To address this, first ensure that the floor is free of tripping hazards like rugs or cords. Motion-activated lights for hallways or the bathroom can deliver low levels of light only when it’s necessary rather than throughout the night.
Wearing an Eye Mask
Sometimes another person wants to keep the TV or a light on, preventing you from sleeping in the dark. Having a conversation about keeping the bedroom dark may or, if they insist on having a light or the TV on, it should be kept at the lowest brightness setting.
If the light is still bothersome, you may get relief by wearing a close-fitting eye mask. Some evidence indicates that an eye covering can contribute to improved sleep quality.
Changing the Settings on Your Electronics
If you doze off with the TV on, it continues generating artificial light in your bedroom during the night. The most sure-fire way to resolve this is to remove the TV from your bedroom. If that’s not practical, check if your TV has a sleep timer to automatically turn off after a period of time. If not, schedule a “lights out” time to shut off the TV each night, and use that as a way to establish a consistent bedtime.
Staring at a cellphone screen before bed has also become more commonplace. Make it a routine to minimize electronic use two to three hours before bedtime. Special glasses can filter blue light to keep it from reaching your eye, which may cut down on the effect of blue light on your sleep. Many phones and tablets have a “night mode” to reduce blue light, although the stimulation from screen time may still affect sleep. If you need to use devices before bed, try out one of several smartphone and computer applications that can help reduce blue light emission.
Frequently Asked Questions about Light and Sleep
What About People Who Sleep With the Lights On?
Not everyone wants or is able to sleep in the dark. Some people prefer to have a light on during sleep because it gives them comfort or because they are afraid of the dark. In these cases, lights should be set to the lowest setting. Lights with a timer may be beneficial so that even if you light is needed to fall asleep, the majority of sleep occurs in darkness.
For serious fears of the dark, consult with a mental health professional who may be able to develop a plan to minimize anxiety at bedtime.
Is There Ever a Time When Sleeping With the Lights on Is Better for You?
It’s almost always better to sleep in the dark; however, you may want some light when taking a daytime nap. Naps are usually the most refreshing when shorter than 30 minutes, and having the lights on may keep you from oversleeping and settling into a deeper sleep than you intend.
What Other Steps Can Improve Sleep and Circadian Rhythm?
If you have long-lasting sleeping problems that are affecting your energy, thinking, or mood, you should talk with your doctor who can best determine the cause, including any potential circadian rhythm disorder.
In addition, you can take steps to improve your sleep hygiene and reset your circadian rhythm. Avoiding excess caffeine, having a consistent sleep schedule, and getting regular exercise, are examples of how your habits and routines can support healthy sleep.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References14 Sources
Fonken, L. K., Workman, J. L., Walton, J. C., Weil, Z. M., Morris, J. S., Haim, A., & Nelson, R. J. (2010). Light at night increases body mass by shifting the time of food intake. Proceedings of the National Academy of Sciences of the United States of America, 107(43), 18664–18669.
https://pubmed.ncbi.nlm.nih.gov/20937863/Sancar, A., Lindsey-Boltz, L. A., Gaddameedhi, S., Selby, C. P., Ye, R., Chiou, Y. Y., Kemp, M. G., Hu, J., Lee, J. H., & Ozturk, N. (2015). Circadian clock, cancer, and chemotherapy. Biochemistry, 54(2), 110–123.
https://pubmed.ncbi.nlm.nih.gov/25302769/Masters, A., Pandi-Perumal, S. R., Seixas, A., Girardin, J. L., & McFarlane, S. I. (2014). Melatonin, the Hormone of Darkness: From Sleep Promotion to Ebola Treatment. Brain disorders & therapy, 4(1), 1000151.
https://pubmed.ncbi.nlm.nih.gov/25705578/Bureau of Labor Statistics. (2019, September). Job Flexibilities and Work Schedules Summary. (USDL-19-1691)., Retrieved October 22, 2020, from
https://www.bls.gov/news.release/flex2.nr0.htmBarion, A., & Zee, P. C. (2007). A clinical approach to circadian rhythm sleep disorders. Sleep medicine, 8(6), 566–577.
https://pubmed.ncbi.nlm.nih.gov/17395535/Blume, C., Garbazza, C., & Spitschan, M. (2019). Effects of light on human circadian rhythms, sleep and mood. Somnologie : Schlafforschung und Schlafmedizin = Somnology : sleep research and sleep medicine, 23(3), 147–156.
https://pubmed.ncbi.nlm.nih.gov/31534436/Lockley, S. W., Brainard, G. C., & Czeisler, C. A. (2003). High sensitivity of the human circadian melatonin rhythm to resetting by short wavelength light. The Journal of clinical endocrinology and metabolism, 88(9), 4502–4505.
https://academic.oup.com/jcem/article/88/9/4502/2845835Carter, B., Rees, P., Hale, L., Bhattacharjee, D., & Paradkar, M. S. (2016). Association Between Portable Screen-Based Media Device Access or Use and Sleep Outcomes: A Systematic Review and Meta-analysis. JAMA pediatrics, 170(12), 1202–1208.
https://pubmed.ncbi.nlm.nih.gov/27802500/Figueiro, M. G., & Rea, M. S. (2012). Preliminary evidence that light through the eyelids can suppress melatonin and phase shift dim light melatonin onset. BMC research notes, 5, 221.
https://pubmed.ncbi.nlm.nih.gov/22564396/Suh, Y. W., Na, K. H., Ahn, S. E., & Oh, J. (2018). Effect of Ambient Light Exposure on Ocular Fatigue during Sleep. Journal of Korean medical science, 33(38), e248.
https://pubmed.ncbi.nlm.nih.gov/30224909/Park, Y. M., White, A. J., Jackson, C. L., Weinberg, C. R., & Sandler, D. P. (2019). Association of Exposure to Artificial Light at Night While Sleeping With Risk of Obesity in Women. JAMA internal medicine, 179(8), 1061–1071. Advance online publication.
https://pubmed.ncbi.nlm.nih.gov/31180469/Garcia-Saenz, A., Sánchez de Miguel, A., Espinosa, A., Valentin, A., Aragonés, N., Llorca, J., Amiano, P., Martín Sánchez, V., Guevara, M., Capelo, R., Tardón, A., Peiró-Perez, R., Jiménez-Moleón, J. J., Roca-Barceló, A., Pérez-Gómez, B., Dierssen-Sotos, T., Fernández-Villa, T., Moreno-Iribas, C., Moreno, V., García-Pérez, J., … Kogevinas, M. (2018). Evaluating the Association between Artificial Light-at-Night Exposure and Breast and Prostate Cancer Risk in Spain (MCC-Spain Study). Environmental health perspectives, 126(4), 047011.
https://pubmed.ncbi.nlm.nih.gov/29687979/Huang, H. W., Zheng, B. L., Jiang, L., Lin, Z. T., Zhang, G. B., Shen, L., & Xi, X. M. (2015). Effect of oral melatonin and wearing earplugs and eye masks on nocturnal sleep in healthy subjects in a simulated intensive care unit environment: which might be a more promising strategy for ICU sleep deprivation?. Critical care (London, England), 19(1), 124.
https://pubmed.ncbi.nlm.nih.gov/25887528/Wahl, S., Engelhardt, M., Schaupp, P., Lappe, C., & Ivanov, I. V. (2019). The inner clock-Blue light sets the human rhythm. Journal of biophotonics, 12(12), e201900102.
https://pubmed.ncbi.nlm.nih.gov/31433569/






















