When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
How Much Does a Sleep Study Cost?
- Sleep study costs vary significantly based on the type. Home sleep tests typically range from $150 to $1,000, while in-lab studies can cost between $1,000 and $10,000.
- Insurance often covers medically necessary sleep studies, though coverage and out-of-pocket costs depend on your plan and deductible.
- Home sleep tests offer a more affordable and convenient alternative to in-lab tests, but they may be less comprehensive.
- Beyond the testing cost, additional expenses can include equipment rental or purchase (for PAP therapy), follow-up appointments, and treatment supplies
The cost of a sleep study can vary widely depending on insurance coverage and whether the test is done at home or in a sleep lab. A sleep study helps doctors and sleep specialists diagnose many types of sleep disorders, including sleep apnea, insomnia, restless legs syndrome, and narcolepsy. Some people may also undergo sleep studies to establish a treatment plan or to confirm that treatment is working.
Below, we’ll discuss the typical costs of sleep studies, what affects pricing, and how insurance coverage or at-home testing can help lower your expenses.
How Much Does a Sleep Study Cost?
A sleep study can cost as little as $150 for an in-home sleep study or more than $10,000 for an in-lab sleep study. Sleep study costs vary from state to state and depend in part on whether a person has insurance coverage .
In-Lab Sleep Study
The average price of an in-lab sleep study is $3,000 . Prices can range from $1,000 to over $10,000, depending on insurance coverage. Facility charges for hospital outpatients can also drive up the total cost of an in-lab sleep study. Fortunately, many insurance providers cover much of a sleep study’s cost.
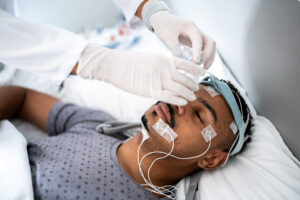
An in-lab sleep study, also known as polysomnography, conducts a comprehensive analysis of a person’s sleep quality by measuring their brain waves, breathing, heart rate, and other parameters. Afterward, sleep specialists analyze the results to reach a diagnosis. This type of sleep study costs more than an at-home sleep study because it takes place while the person sleeps overnight in a lab, with technicians on hand.
People who appear to have an uncomplicated case of moderate to severe obstructive sleep apnea (OSA) may be eligible for a split-night sleep study. The first part of the night is used to diagnose the severity of the sleep apnea while the second half is used to fit the person with a positive airway pressure (PAP) device, a common OSA treatment. A split-night sleep study can be more cost-effective , since it saves the person from having to come back another night for PAP titration.
At-Home Sleep Study
At-home sleep studies can range from $150 to around $1,000 or more, which is much less expensive than in-lab sleep studies. This type of sleep study uses less equipment and takes place at a person’s home, unattended by technicians. The price of an at-home sleep study also depends on the equipment required.
The cost of an at-home sleep study is lower than an in-lab sleep study because it doesn’t involve an overnight clinic stay, typically takes fewer measurements, and has no technicians in attendance. However, a sleep clinic still oversees the test and provides the equipment and instructions, while a certified sleep specialist interprets the results .
Since an at-home sleep study takes fewer measurements than an in-lab sleep study, it isn’t an appropriate test for most sleep disorders. Usually, doctors only recommend at-home sleep studies for people suspected of having moderate to severe obstructive sleep apnea with no other co-occurring sleep disorders. At-home sleep studies may not be appropriate for people with heart or lung conditions.
Most at-home sleep tests don’t measure brain waves, so they may not accurately reflect the amount of time a person is asleep. As a result, at-home tests may underestimate the severity of a person’s OSA . Doctors may request a follow-up in-lab sleep study if the results are inconclusive, which can increase the total cost of testing.
Additional Costs
Some sleep clinics and providers may bill significant outpatient costs in addition to the cost of the sleep study itself. These can include fees for interpreting the test, as well as for treatment and follow-up appointments. These fees may or may not be covered by insurance.
For example, doctors prescribe positive airway pressure therapy to many people with obstructive sleep apnea. A second in-lab sleep study may be required to set up and properly calibrate the PAP machine so that it works effectively while the person is sleeping.
Ongoing costs after the sleep study may include renting or buying a PAP machine, buying related sleep accessories such as a humidifier and PAP mask, and follow-up visits to adjust the airway pressure of the PAP machine.
These costs may be covered by insurance, but some insurance providers require stringent adherence to guidelines for proper use.
Are Sleep Studies Covered by Insurance?
Sleep studies are usually covered by insurance if they’re deemed medically necessary.
Medicare and Medicaid
Medicare covers 80% of the cost of medically necessary sleep studies and PAP titration after the deductible is met, including in a hospital or an approved sleep clinic. To qualify for coverage, a person must have a doctor’s referral for testing based on symptoms of a sleep disorder such as sleep apnea, narcolepsy, or a parasomnia.
The conditions for Medicaid coverage are similar: a person must have symptoms of a relevant sleep disorder and undergo the test in an approved facility. Medicaid and Medicare also cover at-home sleep studies for suspected obstructive sleep apnea.
Private Insurance
Coverage from private insurance providers may vary. Before booking a sleep study, a person should confirm that the center they have chosen is covered by their insurance plan.
As with most medical treatments, a person may be responsible for paying a deductible if they haven’t yet reached their limit. If the plan has a very high deductible, or if a person doesn’t have insurance, they may want to ask for quotes from several sleep clinics.
How Do You Get a Sleep Study?
The first step to obtaining a sleep study is to talk to your doctor about your sleep problems. To provide a better picture of your sleep patterns, it may help to keep a sleep diary before your doctor’s appointment. A sleep partner can also help by sharing observations about your behaviors during sleep.
Your doctor may conduct tests or ask you to fill out a questionnaire about your sleep patterns and medical history. If your doctor refers you for a sleep study, you should contact your insurance provider to make sure the sleep center is covered by your plan.
If your doctor refers you for a sleep study, you will make an appointment for the study with the sleep center or pick up the equipment needed for an at-home sleep study. The center will explain how the sleep study works and how to prepare for the sleep study.
Not all sleep disorders are diagnosed with polysomnography. People with certain sleep disorders may require different tests, such as the maintenance of wakefulness test or the multiple sleep latency test, in addition to or instead of a polysomnography sleep study.
Frequently Asked Questions
What are five symptoms of sleep apnea?
Sleep apnea can come with many symptoms, but there are five that stand out. The first two happen during sleep: frequent and loud snoring, and gasping for air or noticeable pauses in breath. The other three are noticed in the morning or during the day and could be caused by sleep apnea. These are dry mouth, daytime sleepiness/fatigue, and headache during daytime hours.
What is the 4% rule for sleep apnea?
The 4% rule for sleep apnea is used as a diagnostic benchmark by the Centers for Medicare and Medicaid Services to determine if someone is eligible for sleep apnea treatment coverage. It states that one of the criteria for a finding of sleep hypopnea is a minimum of 4% oxygen desaturation from the patient’s baseline.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References13 Sources
Chiedi, J. M. (2019, June). Medicare payments to providers for polysomnography services did not always meet Medicare billing requirements. Department of Health and Human Services, Office of Inspector General.
https://oig.hhs.gov/oas/reports/region4/41707069.pdfHenry, O., Brito, A., Lloyd, M. C., Miller, R., Weaver, E., & Upender, R. (2022). A model for sleep apnea management in underserved patient populations. Journal of Primary Care and Community Health, 13, 21501319211068969.
https://pubmed.ncbi.nlm.nih.gov/35040343/NC Medicaid: Sleep studies and polysomnography services. (2021, May 1). Medicaid and Health Choice Clinical Coverage Policy No.: 1A-20.
https://medicaid.ncdhhs.gov/media/12476/download?attachmentKramer, N. R. & Millman, R. P. (2022, November 15). Overview of polysomnography in adults. In S. M. Harding (Ed.). UpToDate.
https://www.uptodate.com/contents/overview-of-polysomnography-in-adultsKim, R. D., Kapur, V. K., Redline-Bruch, J., Rueschman, M., Auckley, D. H., Benca, R. M., Foldvary-Schafer, N. R., Iber, C., Zee, P. C., Rosen, C. L., Redline, S., & Ramsey, S. D. (2015). An economic evaluation of home versus laboratory-based diagnosis of obstructive sleep apnea. Sleep, 38(7), 1027–1037.
https://pubmed.ncbi.nlm.nih.gov/26118558/Pietzsch, J. B., Garner, A., Cipriano, L. E., & Linehan, J. H. (2011). An integrated health-economic analysis of diagnostic and therapeutic strategies in the treatment of moderate-to-severe obstructive sleep apnea. Sleep, 34(6), 695–709.
https://pubmed.ncbi.nlm.nih.gov/21629357/Wickramasinghe, H. (2020, September 15). Obstructive sleep apnea (OSA) workup.
https://emedicine.medscape.com/article/295807-workup#showallStrohl, K. P. (2022, October). Obstructive sleep apnea (OSA). Merck Manual Professional Version.
https://www.merckmanuals.com/professional/pulmonary-disorders/sleep-apnea/obstructive-sleep-apnea-osaU.S. Centers for Medicare and Medicaid Services. (n.d.) Durable medical equipment (DME) coverage. Medicare.gov.
https://www.medicare.gov/coverage/durable-medical-equipment-dme-coverageU.S. Centers for Medicare and Medicaid Services. (n.d.) Continuous positive airway pressure (CPAP) devices, accessories, & therapy. Medicare.gov.
https://www.medicare.gov/coverage/continuous-positive-airway-pressure-devicesU.S. Centers for Medicare and Medicaid Services. (n.d.) Sleep studies. Medicare.gov.
https://www.medicare.gov/coverage/sleep-studiesU.S. Centers for Medicare & Medicaid Services. (2009, August 10). Sleep testing for obstructive sleep apnea (OSA). CMS.gov.
https://www.cms.gov/medicare-coverage-database/view/ncd.aspx?NCDId=330&ncdver=1&bc=AAAAQAAAAAAAAA%3d%3d&CPAP For Obstructive Sleep Apnea | CMS. www.cms.gov. https://www.cms.gov/medicare/coverage/evidence/cpap
https://www.cms.gov/medicare/coverage/evidence/cpap