When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Maintenance of Wakefulness Test (MWT)
People who experience excessive sleepiness, which involves feeling overly tired or nodding off during the day, often bring their concerns to a sleep specialist. A sleep specialist might order an overnight or at-home sleep study, along with daytime tests such as the the maintenance of wakefulness test (MWT). These tests can uncover potential underlying sleep disorders, as well as evaluate how effectively a disorder is being treated.
We explore the maintenance of wakefulness test in particular, explaining what it entails, what it is used for, and how to prepare for this test.
What Is the Maintenance of Wakefulness Test (MWT)?
The maintenance of wakefulness test (MWT) monitors a person during their normal waking hours as they try to stay awake, unlike a sleep study, which monitors a person as they sleep at night. An MWT is generally given within one-and-a-half to three hours after a person wakes up from their main period of sleep, whether that sleep was obtained at home or in a sleep center for a sleep study.
An MWT indicates how alert a person is by repeatedly measuring how well they are able to resist sleep in a dark, quiet space. Although it is not used to diagnose sleep disorders, the MWT can help sleep specialists identify the severity of symptoms in people experiencing certain sleep disorders, such as narcolepsy and obstructive sleep apnea.
MWT results can also help sleep specialists determine how well a person’s treatment is working, and if it is safe for them to drive a vehicle or work in certain occupations without facing a higher risk for accidents and injuries.
The MWT is designed to give an objective measurement, since subjective feelings of tiredness are not always accurate. That said, there is some debate about whether the MWT is effective for certain uses. Authors of an analysis of many driving studies argue that the MWT cannot accurately predict a person’s driving ability and that a better test is needed for that purpose, while other recent study authors maintain that the MWT can assess driving risk.
Sometimes, researchers also use the MWT to explore how sleepiness affects people with medical conditions that are not traditionally considered sleep disorders. For example, researchers have used the MWT when studying adults with attention deficit hyperactivity disorder (ADHD), based on the premise that the condition might arise from trouble regulating levels of arousal.
Although the MWT is one of the standard tests for measuring daytime sleepiness, it is often used in conjunction with other tests. For example, a doctor might give someone both an objective MWT and the subjective Epworth Sleepiness Scale (ESS), a questionnaire in which people rate the likelihood that they would fall asleep in several different situations. Some researchers also argue that microsleep analysis should be performed along with the MWT, to account for when people fall asleep very briefly during the test.
How Does the Maintenance of Wakefulness Test Work?
Like sleep studies, the maintenance of wakefulness test (MWT) usually takes place in a sleep center or hospital. Generally, the MWT involves four separate time periods — called wake trials — during which a person is monitored for how well they can stay awake.
The first wake trial should begin between one-and-a-half and three hours after you wake up from your major sleep period. This likely means, if you are sleeping at home, you need to set an alarm so you wake up at a specific time on the day of the MWT. People who generally use sleep apnea treatment devices should continue to use them the night before the test.
Before the first wake trial, a clinician may ask questions about recent sleep habits and medications. They may also look over relevant personal data before beginning the test. Sometimes, a urinary drug test is given to verify that drug use does not interfere with test results. Even if there is no drug test, the person being tested might be asked if they need to use the bathroom before the trial begins.
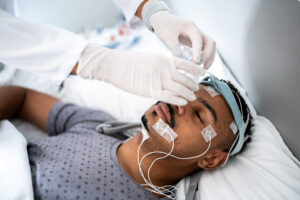
To prepare for the MWT, a clinician connects three or more electroencephalogram (EEG) electrodes to the scalp of the person about to be tested. An EEG measures electrical activity in the brain. By using an EEG to identify the types of brain waves a person is experiencing, experts can determine if they are asleep or awake and, if asleep, what sleep stage they are in.
Once the person being tested has confirmed they are comfortable in the room, the first wake trial starts. The person being tested is asked to remain in their current position and stay awake for as long as they can. They are also instructed to look straight ahead, rather than at the dim light. Any overhead lights are turned off, and wake-promoting activities like fidgeting or singing are not permitted. The trial lasts for 40 minutes, or until the person falls asleep for more than 90 seconds or reaches a deeper sleep stage for at least 30 seconds, whichever comes first.
After the first wake trial, the person being tested leaves the bed or chair. Each of the remaining three wake trials operates identically to the first and begins two hours after the start time of the trial before it. Consuming tobacco and using digital devices are prohibited in the 30 minutes before each wake trial. Sunlight or other bright lights and strenuous activity must be avoided between trials. Often, a light meal is allowed after the second trial.
How Maintenance of Wakefulness Tests Are Scored
Commonly, medical professionals are most interested in the average time it takes a person to fall asleep across the four MWT wake trials. In healthy sleepers, the average time it takes to fall asleep during a wake trial is approximately 30.4 minutes, give or take 11.2 minutes. A significant number of people stay awake for the entire 40 minutes. A sleep specialist may compare an individual’s results against the general population, or they may look for improvements specific to that person’s condition.
Falling asleep in less than eight minutes during a daytime test indicates excessive sleepiness and is part of the criteria for disorders such as narcolepsy and idiopathic hypersomnia. Other cutoff times may be used for measuring sleepiness in high-risk occupations such as professional drivers, where taking less than 30 minutes to fall asleep during the MWT might be considered dangerously sleepy.
Throughout the MWT, these measures are recorded for each wake trial:
- Start time
- End time
- Total sleep time
- Time it took to fall asleep (sleep latency)
If the person does not fall asleep during a wake trial, the sleep latency is recorded as 40 minutes. The raw data from the MWT must be analyzed by a board-certified sleep medicine physician.
How to Prepare for the Maintenance of Wakefulness Test
Prior to undergoing a maintenance of wakefulness test (MWT), there are many things you should share with the sleep specialist:
- How well and how long you have been sleeping each night
- Any symptoms, like excessive daytime tiredness or insomnia, that you have been experiencing
- Your continuous positive airway pressure (CPAP) machine data, if you use a CPAP
- Medications you take, including prescriptions, over-the-counter drugs, and herbal supplements, and any recent adjustments
- How often you consume caffeine and the quantities you consume
Generally, an MWT is conducted when a person is obtaining adequate sleep each night and any sleep disorder symptoms seem well-managed. To verify this, your doctor may ask you to keep a sleep diary or wear a watch-like device that tracks your movements in the two weeks leading up to the test date. There is a lack of evidence on how well the MWT works for shift workers, so it is a good idea to tell your doctor if you have atypical sleep patterns before scheduling the test.
Follow your doctor’s instructions regarding sleep habits, medication changes, and caffeine consumption in the two weeks prior to the test. Often, people preparing for the MWT are advised not to make any medication changes and to reduce or eliminate caffeine. Your doctor might also ask you to limit your use of alcohol, recreational drugs, and sedatives in the weeks leading up to the test.
On the day of the MWT, wear comfortable clothes that will help you maintain a pleasant body temperature during the test. Avoid drinking alcohol, using cannabis, or ingesting any substances that make you sleepy. Eat at the times your doctor advises, which is likely to be at least an hour before the test. Consider bringing a book or magazine to peruse between wake trials. You will not be allowed to sleep, your device usage might be limited, and you might not be able to go out into the sunlight during these breaks.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References15 Sources
Krahn, L. E., Arand, D. L., Avidan, A. Y., Davila, D. G., DeBassio, W. A., Ruoff, C. M., & Harrod, C. G. (2021). Recommended protocols for the multiple sleep latency test and maintenance of wakefulness test in adults: Guidance from the American Academy of Sleep Medicine. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 17(12), 2489–2498.
https://pubmed.ncbi.nlm.nih.gov/34423768/Van der Heide, A., van Schie, M. K., Lammers, G. J., Dauvilliers, Y., Arnulf, I., Mayer, G., Bassetti, C. L., Ding, C. L., Lehert, P., & van Dijk, J. G. (2015). Comparing treatment effect measurements in narcolepsy: The sustained attention to response task, Epworth sleepiness scale and maintenance of wakefulness test. Sleep, 38(7), 1051–1058.
https://pubmed.ncbi.nlm.nih.gov/25902810/Basille, D., Baud, M. E., Andrejak, C., Basille-Fantinato, A., & Jounieaux, V. (2020). Correlation between the Epworth sleepiness scale and the maintenance of wakefulness test in obstructive sleep apnea patients treated with positive airway pressure. Respiratory Medicine and Research, 78, Article 100787.
https://pubmed.ncbi.nlm.nih.gov/32920453/American Academy of Sleep Medicine. (2014). The International Classification of Sleep Disorders – Third Edition (ICSD-3). Darien, IL.
https://aasm.org/Sagaspe, P., Micoulaud-Franchi, J. A., Coste, O., Léger, D., Espié, S., Davenne, D., Lopez, R., Dauvilliers, Y., & Philip, P. (2019). Maintenance of wakefulness test, real and simulated driving in patients with narcolepsy/hypersomnia. Sleep Medicine, 55, 1–5.
https://pubmed.ncbi.nlm.nih.gov/30735912/Valent, F., Sincig, E., Gigli, G. L., & Dolso, P. (2016). Maintenance of wakefulness and occupational injuries among workers of an Italian teaching hospital. Safety and Health at Work, 7(2), 120–123.
https://pubmed.ncbi.nlm.nih.gov/27340598/Sander, C., Hensch, T., Wittekind, D. A., Böttger, D., & Hegerl, U. (2015). Assessment of wakefulness and brain arousal regulation in psychiatric research. Neuropsychobiology, 72(3–4), 195–205.
https://pubmed.ncbi.nlm.nih.gov/26901462/Virtanen, I., Järvinen, J., & Anttalainen, U. (2019). Can real-life driving ability be predicted by the maintenance of wakefulness test? Traffic Injury Prevention, 20(6), 601–606.
https://pubmed.ncbi.nlm.nih.gov/31329466/Philip, P., Guichard, K., Strauss, M., Léger, D., Pepin, E., Arnulf, I., Sagaspe, P., Barateau, L., Lopez, R., Taillard, J., Micoulaud-Franchi, J. A., & Dauvilliers, Y. (2021). Maintenance of wakefulness test: How does it predict accident risk in patients with sleep disorders? Sleep Medicine, 77, 249–255.
https://pubmed.ncbi.nlm.nih.gov/32778442/Bioulac, S., Chaufton, C., Taillard, J., Claret, A., Sagaspe, P., Fabrigoule, C., Bouvard, M. P., & Philip, P. (2015). Excessive daytime sleepiness in adult patients with ADHD as measured by the maintenance of wakefulness test, an electrophysiologic measure. The Journal of Clinical Psychiatry, 76(7), 943–948.
https://pubmed.ncbi.nlm.nih.gov/25610980/Lok, R., & Zeitzer, J. M. (2021). Physiological correlates of the Epworth Sleepiness Scale reveal different dimensions of daytime sleepiness. Sleep Advances: A Journal of the Sleep Research Society, 2(1), zpab008.
https://pubmed.ncbi.nlm.nih.gov/34250482/Anniss, A. M., Young, A., & O’Driscoll, D. M. (2021). Microsleep assessment enhances interpretation of the maintenance of wakefulness test. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 17(8), 1571–1578.
https://pubmed.ncbi.nlm.nih.gov/33729911/Anniss, A. M., Young, A., & O’Driscoll, D. M. (2016). Importance of urinary drug screening in the multiple sleep latency test and maintenance of wakefulness test. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 12(12), 1633–1640.
https://pubmed.ncbi.nlm.nih.gov/27655451/Rayi, A., & Murr, N. (2021). Electroencephalogram. In StatPearls. StatPearls Publishing.
https://pubmed.ncbi.nlm.nih.gov/33085442/Silber, M. H., Ancoli-Israel, S., Bonnet, M. H., Chokroverty, S., Grigg-Damberger, M. M., Hirshkowitz, M., Kapen, S., Keenan, S. A., Kryger, M. H., Penzel, T., Pressman, M. R., & Iber, C. (2007). The visual scoring of sleep in adults. Journal of Clinical Sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 3(2), 121–131.
https://pubmed.ncbi.nlm.nih.gov/17557422/