What Conditions Can Cause Excessive Daytime Sleepiness?
- Conditions such as neurological disorders, mental health issues, and sleep disorders like obstructive sleep apnea can all contribute significantly to excessive daytime sleepiness.
- Some medications, including sedatives, can also cause excessive sleepiness.
- Identifying the root cause—whether lifestyle, medical, or neurological—is key to effective treatment and improving alertness, mood, and overall health.
Feeling unusually tired during the day can be more than just a sign of a late night, it may point to an underlying health condition. Excessive daytime sleepiness is a common symptom that can affect focus, mood, and overall quality of life. While sleep disorders like sleep apnea or narcolepsy are well-known causes, a wide range of medical, neurological, and psychological conditions can also lead to persistent drowsiness.
Understanding what’s behind your fatigue is the first step toward finding effective treatment and restoring healthy, refreshing sleep.
What Is Excessive Daytime Sleepiness?
Excessive daytime sleepiness isn’t a condition in itself. Rather, it’s a symptom caused by an underlying problem or a combination of factors. Excessive daytime sleepiness is defined as a difficulty staying awake or alert throughout the day. Those who experience this drowsiness often feel the urge to sleep during the day when they need to be awake .
Many experts define EDS as distinct from fatigue , which involves strong feelings of physical exhaustion, but the two conditions may overlap.
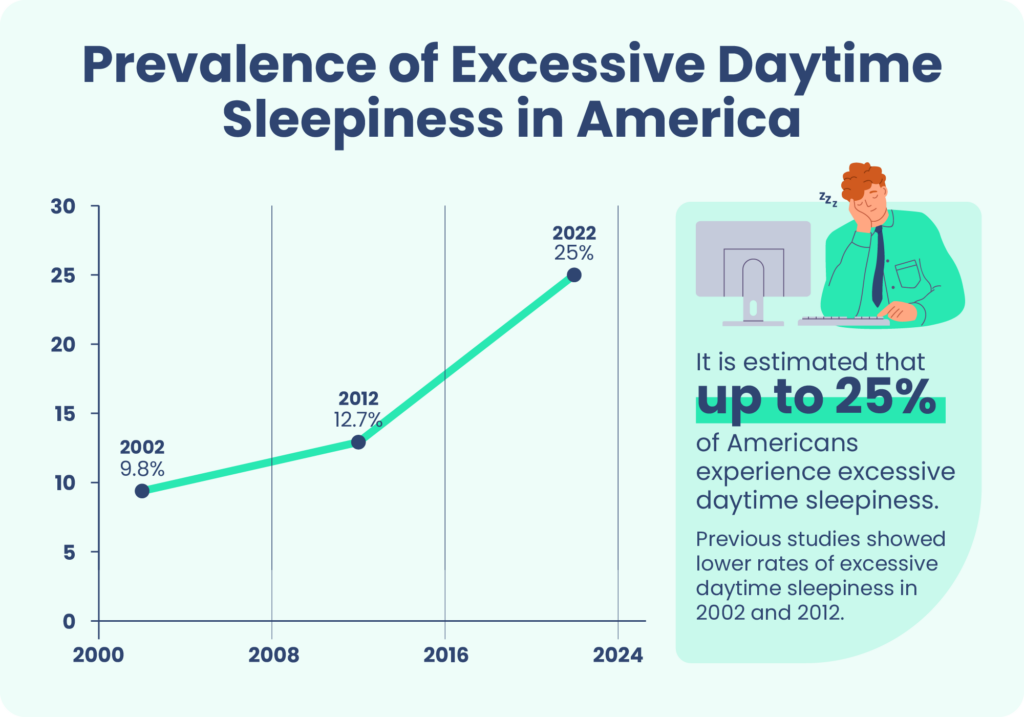
Recent research points to excessive sleepiness being a significant problem, affecting up to 25% of the population . Though varying definitions of excessive daytime sleepiness make it difficult to fully gauge its prevalence, it does appear to have increased in recent years .
Conditions That Can Cause Excessive Daytime Sleepiness
The most common causes of excessive sleepiness are sleep deprivation and disorders like sleep apnea and insomnia. Depression and other mental health conditions, certain medications, and medical conditions affecting the brain and body can cause daytime drowsiness as well.
Sleep Deprivation
Lack of sleep is widely considered to be the most common cause of excessive sleepiness . Sleep deprivation may be short-term or chronic and can have a variety of causes.
- Failure to prioritize sleep: Sacrificing sleep for other activities can cause drowsiness the next day, and the problem can accumulate over time. When these choices cause lack of sleep over an extended period of time, it’s known as insufficient sleep syndrome .
- Poor sleep quality: Sleep insufficiency isn’t just about a low quantity of sleep, it’s also about sleep quality. People who don’t smoothly progress through sleep cycles may fail to get enough deep sleep or REM sleep. As a result, they may not wake up refreshed even if they sleep for the recommended number of hours.
- Pain: Virtually any ailment that induces pain, including arthritis or fibromyalgia, can complicate sleep and make a person prone to drowsiness during the day.
- Frequent nighttime urination: This condition, known as nocturia, involves needing to get up from bed during the night to use the bathroom. People who experience nocturia may find it difficult to fall back asleep after each nighttime awakening.
Sleep Disorders
Sleep disorders can negatively affect the amount of quality sleep a person gets, resulting in daytime drowsiness.
- Insomnia: Insomnia makes it hard to fall asleep or stay asleep for as long as you want. Insomnia is often related to other sleep problems that give rise to excessive sleepiness.
- Sleep apnea: Obstructive sleep apnea (OSA) is a breathing disorder characterized by brief pauses in breathing during the night. It creates fragmented sleep that typically causes daytime drowsiness. Central sleep apnea (CSA) is less common but can also cause disturbed sleep.
- Restless legs syndrome (RLS): This condition causes a strong sensation of needing to move one’s extremities, particularly the legs. Restless legs syndrome is a known risk for disrupting total sleep time and sleep quality.
- Circadian rhythm sleep-wake disorders: When a person’s sleep schedule is misaligned with their local day-night cycle, it can cause short and fragmented sleep. Examples include jet lag and sleep problems among shift workers.
Other Medical Conditions
Certain medical conditions are associated with sleep issues and excessive daytime drowsiness.
- Mental health disorders: It’s believed that nearly 80% of people with major depression have excessive daytime sleepiness. Bipolar disorder, post-traumatic stress disorder (PTSD), and general anxiety disorder are associated with sleeping problems that may give rise to bouts of excessive sleepiness.
- Neurological conditions:Narcolepsy is a prominent example, as it’s a neurological condition in which the brain cannot properly regulate the sleep-wake cycle. Narcolepsy makes people prone to falling asleep rapidly, including at inopportune times.
- Neurodegenerative diseases: Neurodegenerative diseases including dementia and Parkinson’s disease are tied with sleeping difficulties and daytime drowsiness.
- Injury and infection: Traumatic brain injury (TBI) and concussions commonly cause sleeping problems , and brain tumors or lesions may provoke excessive sleepiness. Infections, including meningitis and those that cause swelling of the brain , can also lead to EDS.
- Neurodevelopmental disorders: Attention-deficit/hyperactivity disorder (ADHD) can cause a range of sleeping problems including daytime sleepiness. Children with autism spectrum disorder (ASD) have also been found to have difficulty sleeping , which could lead to daytime sleepiness. Sleeping issues may persist into adulthood for people with these neurodevelopmental disorders.
Other health problems can make a person sleepy during the day. Metabolic problems, including diabetes and hypothyroidism, can be risk factors for drowsiness. Medical conditions like anemia, abnormal blood sodium levels, and electrolyte imbalances can also provoke excessive sleepiness.
Medications
A lack of sleep isn’t the only potential cause of excessive sleepiness. Medications, especially sedatives, can make a person drowsy and disoriented during the day. Antidepressants, pain medications, and over-the-counter antihistamines are just a few of the other types of medications that can cause sleepiness. In addition, withdrawal from some drugs may provoke drowsiness.
It’s important to discuss your current medications and potential side effects with your doctor. They can offer guidance on timing and dosage of your medications and make adjustments as needed. Don’t make any changes to your medication without consulting your doctor.
Treatment for Excessive Daytime Sleepiness
Relief is possible for most people with excessive sleepiness. The optimal treatment for excessive sleepiness is tailored to each person based on the specific cause or contributing factors.
Because EDS can be caused by both poor sleep habits and medical and brain conditions, there are a diverse range of approaches to resolving it. A doctor is in the best position to identify and tailor optimal treatment pathways for individuals.
If drowsiness is derived from sleep deprivation, various steps can be taken to improve sleep quality and quantity. Examples include continuous positive airway pressure (CPAP) therapy for sleep apnea and cognitive behavioral therapy for insomnia (CBT-I). Many sleep-focused treatments will help facilitate improvements to sleep hygiene, which incorporates a person’s sleep habits and bedroom environment, and whether they’re using the best mattress and pillow for their needs.
If EDS is tied to another medical problem, treatment typically focuses on resolving that underlying issue. Sleep hygiene improvements may be encouraged along with other treatments to help people incorporate healthy sleep tips into their daily routines.
Frequently Asked Questions
Is excessive sleepiness a sign of dementia?
Excessive daytime sleepiness can sometimes occur in people with dementia, particularly Alzheimer’s disease. Changes in the brain may disrupt the body’s internal clock and interfere with normal sleep–wake patterns. People with dementia may nap frequently during the day or experience fragmented sleep at night.
However, excessive sleepiness can also have other causes, so it’s important to discuss symptoms with a healthcare provider for an accurate diagnosis.
Can ADHD cause excessive sleepiness?
Yes. While ADHD is often associated with hyperactivity, it can also cause fatigue and daytime sleepiness in some people. Sleep problems are common in individuals with ADHD, including delayed sleep timing, restless sleep, and difficulty waking up.
Certain ADHD medications can also affect sleep patterns. If excessive tiredness is interfering with daily life, a doctor can help evaluate whether sleep issues or medication side effects are contributing.
Is excessive sleepiness a sign of pregnancy?
Yes. Increased sleepiness is common during early pregnancy due to hormonal changes—particularly higher levels of progesterone—that promote drowsiness. Growing energy demands and disrupted nighttime sleep can also add to daytime fatigue.
While mild tiredness is normal, persistent or extreme sleepiness may indicate anemia, thyroid changes, or another medical concern, so it’s best to check with a prenatal care provider.
Can anemia cause excessive sleepiness?
Yes, anemia, especially iron-deficiency anemia, reduces the amount of oxygen delivered to tissues throughout the body. This can lead to fatigue, weakness, and difficulty staying alert during the day. Because anemia has many possible causes, including diet, chronic conditions, or blood loss, it’s important to have blood work done to confirm the diagnosis and guide treatment.
Can anxiety cause excessive sleepiness?
Yes, anxiety can disrupt sleep quality, making it hard to fall asleep or stay asleep through the night. Over time, poor sleep can cause persistent daytime fatigue and difficulty concentrating.
Additionally, the body’s stress response can be draining, leaving people feeling mentally and physically exhausted. Managing anxiety through therapy, relaxation techniques, or treatment can help improve sleepiness and overall energy.
Can a head injury cause excessive sleepiness?
Yes. After a head injury or concussion, it’s common to experience excessive sleepiness as the brain heals. Damage to brain regions that control sleep–wake cycles can lead to hypersomnia or irregular sleep patterns. In some cases, these symptoms may persist for weeks or even months.
Anyone who feels unusually sleepy after a head injury should seek medical evaluation to rule out more serious complications and receive appropriate care.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References12 Sources
American Academy of Sleep Medicine. (2014). The International Classification of Sleep Disorders – Third Edition (ICSD-3). Darien, IL.
https://aasm.org/Smith, S., Rossdale, J., Serry, Y., Sekaran, A., Drakatos, P., & Steier, J. (2018). Multiple dimensions of excessive daytime sleepiness. Journal of thoracic disease, 10(Suppl 1), S170–S176.
https://pubmed.ncbi.nlm.nih.gov/29445541/Chervin, R. D. (2021, September 29). Approach to the patient with excessive daytime sleepiness. In T. E. Scammell (Ed.). UpToDate.
https://www.uptodate.com/contents/approach-to-the-patient-with-excessive-daytime-sleepinessFord, E. S., Cunningham, T. J., Giles, W. H., & Croft, J. B. (2015). Trends in insomnia and excessive daytime sleepiness among U.S. adults from 2002 to 2012. Sleep Medicine, 16(3), 372–378.
https://pubmed.ncbi.nlm.nih.gov/25747141/Murray B. J. (2016). A practical approach to excessive daytime sleepiness: A focused review. Canadian Respiratory Journal, 2016, 4215938.
https://pubmed.ncbi.nlm.nih.gov/27445538/Chattu, V. K., Sakhamuri, S. M., Kumar, R., Spence, D. W., BaHammam, A. S., & Pandi-Perumal, S. R. (2018). Insufficient sleep syndrome: Is it time to classify it as a major noncommunicable disease?. Sleep Science, 11(2), 56–64.
https://pubmed.ncbi.nlm.nih.gov/30083291/Schwab, R. J. (2022, May). Insomnia and excessive daytime sleepiness (EDS). Merck Manual Consumer Version.
https://www.merckmanuals.com/home/brain,-spinal-cord,-and-nerve-disorders/sleep-disorders/insomnia-and-excessive-daytime-sleepiness-edsLim, M.M, & Baumann, C.R. (2023, February 15). Sleep-wake disorders in patients with traumatic brain injury. In A. F. Eichler (Ed.). UpToDate.
https://www.uptodate.com/contents/sleep-wake-disorders-in-patients-with-traumatic-brain-injuryA.D.A.M. Medical Encyclopedia. (2020, December 24). Meningitis. MedlinePlus.
https://medlineplus.gov/ency/article/000680.htmA.D.A.M. Medical Encyclopedia. (2020, August 29). Encephalitis. MedlinePlus.
https://medlineplus.gov/ency/article/001415.htmA.D.A.M. Medical Encyclopedia. (2022, June 7). Autism spectrum disorder. MedlinePlus.
https://medlineplus.gov/ency/article/001526.htmA.D.A.M. Medical Encyclopedia. (2022, July 14). Drowsiness. MedlinePlus.
https://medlineplus.gov/ency/article/003208.htm
































































