When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Melatonin Dosage for Kids
- More research is needed to determine the safety of melatonin for kids.
- Melatonin dosage for kids should be determined by a medical professional, taking into consideration the child’s age, weight, and type of sleep issue.
- Doctors may recommend starting with the lowest possible dose, and only increasing the dose if needed.
- Parents and caregivers should speak with their child’s pediatrician before giving their child any type of sleep aid.
In recent years, the number of people using melatonin supplements has increased significantly. As this supplement grows in popularity, parents and caregivers may wonder whether it is safe for their kids to use melatonin and, if so, how to determine the appropriate dosage.
When it comes to melatonin, there are serious risks for parents and caregivers to consider. Before giving a child melatonin, it is important to consult a doctor for additional guidance regarding the use and dosage of melatonin. We take a closer look at the potential dosage and safety of melatonin for children and teenagers, as well as other measures that can help kids get better sleep.
Is Melatonin Safe for Kids?
At this time, there has not been enough research conducted to fully understand the overall safety of melatonin for children or adolescents.
Guidelines for melatonin usage in children focus on its use for diagnosed sleep disorders and in children with certain medical conditions, such as autism spectrum disorder and attention-deficit/hyperactivity disorder. Currently, there is limited data on melatonin use in children without these conditions .
Experts suggest working closely with a child’s pediatrician when deciding whether to give melatonin to a child or adolescent. In particular, medical professionals emphasize that melatonin should not be used as a way to pressure or force a child to sleep, but should only be given to children with a confirmed medical need under the guidance of a doctor.
How Much Melatonin Should I Give My Child?
Before giving your child melatonin, consult with their doctor to determine the dosage. Dosage recommendations for melatonin can vary depending on the type of sleep problem and the child’s age.
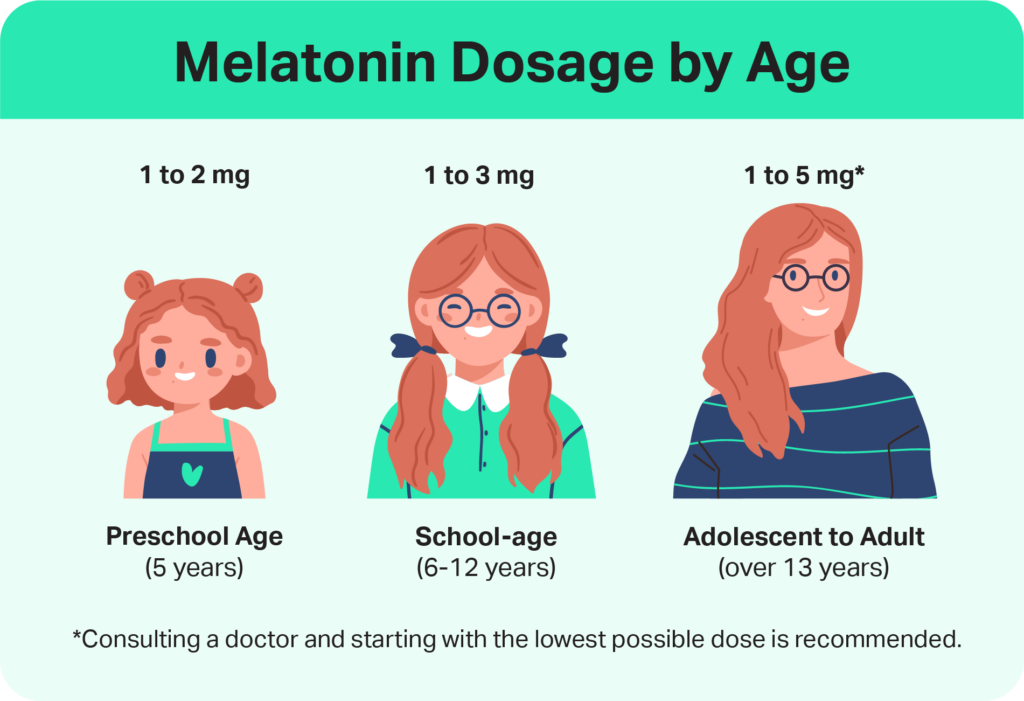
Doctors may prescribe melatonin for sleep-onset insomnia, which makes it difficult to fall asleep . For this diagnosis, doctors often use the following dosage levels:
- Preschoolers (5 years): 1 to 2 milligrams
- School-age (6 to 12 years): 1 to 3 milligrams
- Adolescents (13 to 18 years): 1 to 5 milligrams
In all cases, however, experts recommend always starting with the lowest dose of melatonin available, then increasing the amount only if necessary. Parents and caregivers should avoid cutting or splitting supplements to reduce the dosage, as this can result in inconsistent dosing.
Poison control centers have also noted increased reports of melatonin ingestion in children, with adverse effects . Parents and caregivers should take additional safety measures to keep melatonin out of reach of children in order to prevent accidental ingestion or overdose.
Side Effects of Melatonin in Children
When starting any new vitamin, supplement, or medication, it is important to discuss it with a doctor and weigh the risks beforehand. Although more studies need to evaluate risks of taking melatonin long-term, reported side effects in children and adolescents include:
- Agitation
- Dizziness
- Drowsiness
- Fatigue
- Headache
- Increased bedwetting
- Mood swings
Because melatonin is a hormone, some health professionals have suggested that taking it as a supplement could interfere with a child’s development.
Melatonin may also interact and interfere with other herbs, supplements, and certain medications. A child’s doctor should be aware of any supplements or medications the child is currently taking before they start melatonin.
What to Consider Before Giving Your Child Melatonin
Before giving a child any sleep aid, it is important to discuss this decision thoroughly with a pediatrician. Childhood sleep problems do not always require treatment with drugs or supplements. Many times, changing bedtime behavior alone is enough. The child’s doctor can discuss whether melatonin is appropriate for the situation as well as the supplement’s risks, benefits, and dosage.
As a dietary supplement, melatonin is not regulated or approved by the U.S. Food and Drug Administration. As a result, the actual concentration of melatonin contained in different products and formulations varies greatly . The true amount can even be different from the amount listed on the product’s label. Some experts suggest using pharmaceutical-grade products, which may be more reliable.
Furthermore, what may work for an adult as a sleep aid may not be helpful for a child . One reason for this is that children metabolize medicines and supplements differently than adults.
Many different melatonin products are available to purchase. If a child’s doctor approves the use of melatonin, it may be helpful to ask about specific products, as well as the dosage and duration of treatment.
The safety and efficacy of supplements is not closely monitored by the U.S. Food and Drug Administration (FDA). Shoppers should take additional measures to make sure they are purchasing reputable products.
Alternatives to Melatonin for Kids
Aside from melatonin, doctors may recommend other drugs or supplements to help a child with sleep-related issues. Some of these require a prescription. Others can be purchased over the counter, but should still only be used under the guidance of a doctor.
- Antihistamines: Over-the-counter antihistamines that relieve allergy symptoms can also cause drowsiness . Though antihistamines are available without a prescription, they have serious risks and should be used under the guidance of a pediatrician.
- Valerian: Valerian is a plant that is marketed as a sleep aid and dietary supplement. The evidence is mixed regarding valerian’s effectiveness at treating insomnia, but studies report few negative side effects. Children under 3 years old should not take valerian.
- Prescription drugs: In some cases, doctors may prescribe drugs that are usually used to treat sleep problems in adults.
Note that experts caution against taking melatonin in combination with other sleep aids. They can have an additive effect in the body, causing an excess of sleepiness or sedation, and may interact in other ways that could be dangerous.
Anyone considering giving a child or adolescent any product to help them sleep should start by talking with the child’s pediatrician for guidance. Every situation is unique, and what works for one child may not be helpful for another.
Sleep Tips for Kids
Problems at bedtime are relatively common in children and typically respond well to behavioral strategies. Before starting melatonin, it may be helpful to try new routines and other behavioral changes to combat sleep issues. There are a variety of sleep strategies to consider that may help a child get better sleep.
- Follow a bedtime routine: Routines help children improve their sleep. Components of a nightly routine might include taking a warm bath, changing into pajamas, brushing teeth, turning off bright lights, and reading a bedtime story.
- Set consistent bedtimes: Keep children’s bedtimes the same every day, even on weekends. This consistency reinforces the child’s sleep schedule.
- Keep screens out of the bedroom: Electronic devices that emit blue light can delay the release of natural melatonin in the body. Using smartphones, computers, TVs, and gaming devices just before sleep can signal the brain to remain alert and awake. It is recommended to avoid screens for at least two hours before bedtime.
- Provide opportunities for exercise: Daily physical activity improves the chances kids will be tired by bedtime. When kids and teens do not get their bodies moving during the day, they may not feel sleepy at bedtime.
- Be careful with food and drink: Eating a large meal before bedtime or drinking beverages with caffeine can make it harder to get a good night’s sleep.
- Create a space conducive to sleep: Be sure your child’s bedroom is free from light and noise, and keep the thermostat at a temperature that is comfortable.
Medical Disclaimer: The content on this page should not be taken as medical advice or used as a recommendation for any specific treatment or medication. Always consult your doctor before taking a new medication or changing your current treatment.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
13 Sources
-
Owens, J. A. (2023, January 3). Pharmacotherapy for insomnia in children and adolescents: A rational approach. In R. D. Chervin (Ed.). UpToDate., Retrieved March 29, 2023, from
https://www.uptodate.com/contents/pharmacotherapy-for-insomnia-in-children-and-adolescents-a-rational-approach -
Skrzelowski, M., Brookhaus, A., Shea, L. A., & Berlau, D. J. (2021). Melatonin use in pediatrics: Evaluating the discrepancy in evidence based on country and regulations regarding production. The Journal of Pediatric Pharmacology and Therapeutics, 26(1), 4–20.
https://pubmed.ncbi.nlm.nih.gov/33424495/ -
Schwab, R. J. (2022, May). Insomnia and excessive daytime sleepiness (EDS). Merck Manual Consumer Version., Retrieved March 29, 2023, from
https://www.merckmanuals.com/home/brain,-spinal-cord,-and-nerve-disorders/sleep-disorders/insomnia-and-excessive-daytime-sleepiness-eds -
Lelak, K., Vohra, V., Neuman, M. I., Toce, M. S., & Sethuraman, U. (2022). Pediatric melatonin ingestions – United States, 2012-2021. MMWR. Morbidity and Mortality Weekly Report, 71(22), 725–729.
https://pubmed.ncbi.nlm.nih.gov/35653284/ -
Zisapel, N. (2022). Assessing the potential for drug interactions and long term safety of melatonin for the treatment of insomnia in children with autism spectrum disorder. Expert Review of Clinical Pharmacology, 15(2), 175–185.
https://pubmed.ncbi.nlm.nih.gov/35285365/ -
Savage, R. A., Zafar, N., Yohannan, S., & Miller, J. M. (2022, August 8). Melatonin. In StatPearls. StatPearls Publishing., Retrieved March 29, 2023, from
https://www.ncbi.nlm.nih.gov/books/NBK534823/ -
Erland, L. A., & Saxena, P. K. (2017). Melatonin natural health products and supplements: Presence of serotonin and significant variability of melatonin content. Journal of Clinical Sleep Medicine, 13(2), 275–281.
https://pubmed.ncbi.nlm.nih.gov/27855744/ -
Jones, B. L. (2022, December). Overview of drug treatment in children. Merck Manual Professional Version., Retrieved March 29, 2023, from
https://www.merckmanuals.com/professional/pediatrics/principles-of-drug-treatment-in-children/overview-of-drug-treatment-in-children -
A.D.A.M. Medical Encyclopedia. (2022, April 10). Antihistamines for allergies. MedlinePlus., Retrieved March 29, 2023, from
https://medlineplus.gov/ency/patientinstructions/000549.htm -
National Institutes of Health Office of Dietary Supplements. (2013, March 15). Valerian., Retrieved March 29, 2023, from
https://ods.od.nih.gov/factsheets/Valerian-HealthProfessional/ -
Owens, J. A. (2020, August 18). Behavioral sleep problems in children. In R. D. Chervin (Ed.). UpToDate., Retrieved March 29, 2023, from
https://www.uptodate.com/contents/behavioral-sleep-problems-in-children -
Shechter, A., Kim, E. W., St-Onge, M. P., & Westwood, A. J. (2018). Blocking nocturnal blue light for insomnia: A randomized controlled trial. Journal of Psychiatric Research, 96, 196–202.
https://pubmed.ncbi.nlm.nih.gov/29101797/ -
Peterson, D. M. (2022, June 16). The benefits and risks of aerobic exercise. In M. D. Aronson & F. G. O’Connor (Eds.) UpToDate., Retrieved March 29, 2023, from
https://www.uptodate.com/contents/the-benefits-and-risks-of-aerobic-exercise