Why We Have Nightmares (And How to Prevent Them)
- Nightmares are bad dreams that wake you up, often with feelings worry or fear.
- Nightmares occur more frequently during rapid eye movement (REM) sleep.
- Frequent nightmares that interfere with daily functioning, mood, or sleep, may indicate a nightmare disorder.
- What causes nightmares is unknown, but it may have to do with emotional processing.
Dreaming is one of the most complicated and mysterious aspects of sleep. While dreams can include visions of grandeur and bliss, they can also be scary, threatening, or stressful. When a bad dream causes you to wake up, it’s known as a nightmare.
It’s normal to occasionally have a nightmare or bad dream, but for some people, they recur frequently, disrupting sleep and negatively impacting their waking life as well. Knowing the differences between bad dreams, nightmares, and nightmare disorder is a first step to addressing the causes of nightmares, starting appropriate treatment, and getting better sleep.
What Are Nightmares?
In sleep medicine, nightmares have a more strict definition than in everyday language. This definition helps distinguish nightmares from bad dreams: while both involve disturbing dream content, only a nightmare causes you to wake up from sleep.
Nightmares are vivid dreams that may be threatening, upsetting, bizarre, or otherwise bothersome. They occur more often during rapid eye movement (REM) sleep, the stage of sleep associated with intense dreaming. Nightmares arise more frequently in the second half of the night when more time is spent in REM sleep.
Upon waking up from a nightmare, it’s normal to be acutely aware of what happened in the dream, and many people find themselves feeling upset or anxious. Physical symptoms like heart rate changes or sweating may be detected after waking up as well.

Are Nightmares Normal?
It’s normal for both children and adults to have bad dreams and nightmares every now and again. About 2%-8% of adults have problems with nightmares.
Frequent nightmares are more common in children than in adults. Nightmares in children are most prevalent between the ages of 3 and 6 and tend to occur less often as children get older. In some cases, though, nightmares persist into adolescence and adulthood. For example, a study found that 47% of college students had at least one nightmare in the past two weeks.
Nightmares affect males and females, although women are generally more likely to report having nightmares, especially during adolescence through middle age.

What Causes Nightmares?
There is no consensus explanation for why we have nightmares. In fact, there is an ongoing debate in sleep medicine and neuroscience about why we dream at all. Many experts believe that dreaming is part of the mind’s methods for processing emotion and consolidating memory. Bad dreams, then, may be a component of the emotional response to fear and trauma, but more research is needed to definitively explain why nightmares occur.
Many different factors can contribute to a higher risk of nightmares:
- Stress and anxiety: Sad, traumatic, or worrisome situations that induce stress and fear may provoke nightmares. People with chronic stress and anxiety may be more likely to develop nightmare disorder.
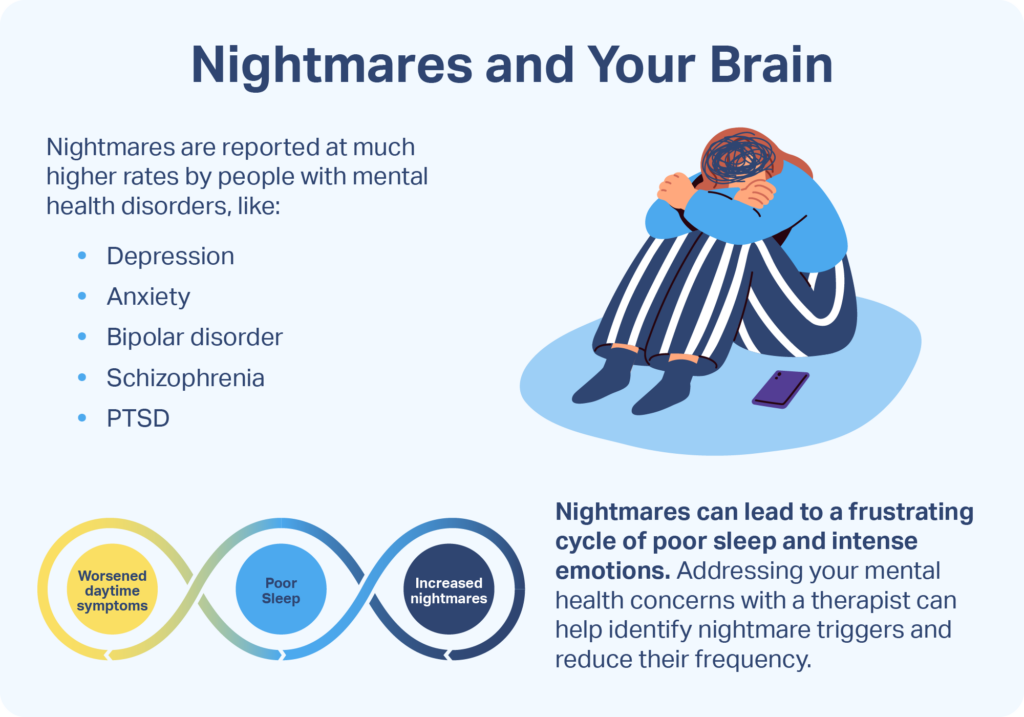
- Mental health conditions: Nightmares are often reported at much higher rates by people with mental health disorders like post-traumatic stress disorder (PTSD). People with PTSD often have frequent, intense nightmares in which they relive traumatic events, worsening symptoms of PTSD, and often contributing to insomnia.
- Certain drugs and medications: Using some types of illicit substances or prescription medications that affect the nervous system is associated with a higher risk of nightmares.
- Withdrawal from some medications: Some medications suppress REM sleep, so when a person stops taking those medications, there is a short-term rebound effect of more REM sleep accompanied by more nightmares.
- Sleep deprivation: After a period of insufficient sleep, a person often experiences a REM rebound that can trigger vivid dreams and nightmares.
- Family history: Though not fully understood, a genetic predisposition may exist that makes it more likely for frequent nightmares to run in a family. This association may be driven by genetic risk factors for mental health conditions that are tied to nightmares.
- Personal history of nightmares: In adults, a risk factor for nightmare disorder is a history of having had recurring nightmares during childhood and adolescence.
Some evidence indicates that people who have nightmares may have altered sleep architecture, meaning that they progress abnormally through sleep stages. Some studies have also found a correlation between nightmares and obstructive sleep apnea (OSA), a breathing disorder that causes fragmented sleep, although further research is needed to clarify this association.
What Is Nightmare Disorder?
Nightmare disorder is a parasomnia that occurs when a person has frequent nightmares that interfere with their sleep, mood, and/or daytime functioning. While most people have nightmares from time to time, nightmare disorder is far less common.
People who have occasional nightmares don’t have nightmare disorder. Instead, nightmare disorder involves recurring nightmares that bring about notable distress in their daily life.
Are Nightmares Different From Sleep Terrors?
Sleep terrors, sometimes called night terrors, are another type of parasomnia in which a sleeper appears agitated and frightened during sleep. Nightmares and sleep terrors have several distinguishing characteristics:
- Nightmares happen during REM sleep while sleep terrors happen during non-REM (NREM) sleep.
- Sleep terrors don’t involve a full awakening; instead, a person remains mostly asleep and difficult to awaken. If awakened, they likely will be disoriented. In contrast, when a person wakes up from a nightmare, they tend to be alert and aware of what was happening in their dream.
- The following day, a person with nightmares usually has a clear memory of the dream. People with sleep terrors very rarely have any awareness of the episode.
- Nightmares are more common in the second half of the night while sleep terrors happen more often in the first half.
How Can Nightmares Affect Sleep?
Nightmares, especially recurrent nightmares, can have a significant impact on a person’s sleep. People who have nighttime disruptions from nightmares may wake up feeling anxious, making it hard to relax their mind and get back to sleep. As a result, the fear of nightmares may cause sleep avoidance and less time allocated to sleep.
Unfortunately, this can make nightmares worse. Sleep avoidance can cause sleep deprivation, which can provoke a REM sleep rebound with even more intense dreams and nightmares. This often leads to further sleep avoidance, giving rise to a pattern of disturbed sleep that culminates in insomnia.
Insufficient sleep connected to nightmares and nightmare disorder can cause excessive daytime sleepiness, mood changes, and worsened cognitive function, all of which can have a substantial negative impact on a person’s daytime activities and quality of life. Nightmares may also exacerbate mental health conditions that can worsen sleep, and insufficient sleep can give rise to more pronounced symptoms of conditions like depression and anxiety.
When Should You See a Doctor About Nightmares?
Because it’s common to have an occasional nightmare, some people may find it hard to know when nightmares are a cause for concern. You should talk to your doctor about nightmares if:
- Nightmares happen more than once a week
- Nightmares affect your sleep, mood, and/or daily activity
- Nightmares begin at the same time that you start a new medication
To help your doctor understand how nightmares are affecting you, you can keep a sleep diary that tracks your total sleep and sleep disruptions, including nightmares.
How Is Nightmare Disorder Treated?
Infrequent nightmares don’t normally need any treatment, but both psychotherapy and medications can help people who have nightmare disorder. By reducing nightmares, treatments can promote better sleep and overall health.
Treatment for nightmares should always be overseen by a health professional who can identify the most appropriate therapy based on a patient’s overall health and the underlying cause of their nightmares.
Psychotherapy
Psychotherapy, also known as talk therapy, is a category of treatment that works to understand and reorient negative thinking. There are numerous types of talk therapy that may help reduce nightmares:
- Image Rehearsal Therapy: This approach involves rewriting a recurring nightmare into a script that is rewritten and then rehearsed when awake in order to change how it unfolds and impacts the sleeper.
- Lucid Dreaming Therapy: In a lucid dream, a person is actively aware that they are dreaming. Lucid dreaming therapy seizes on this idea to give a person the ability to positively modify the content of a nightmare through their awareness of it in the moment.
- Exposure and Desensitization Therapies: Because many nightmares are driven by fears, a number of approaches utilize controlled exposure to that fear to reduce the emotional reaction to it. Examples of these techniques to “face your fears” include self-exposure therapy and systematic desensitization.
- Hypnosis: This approach creates a relaxed, trance-like mental state in which a person can more easily take in positive thoughts to combat stress.
- Progressive deep muscle relaxation: While not a direct form of talk therapy, progressive deep muscle relaxation is a technique for calming the mind and body. It involves deep breathing and releasing tension throughout the body. There are many audio guides available online to help lead users through the technique.
- Cognitive-Behavioral Therapy for Insomnia (CBT-I):CBT-I focuses on restructuring the thoughts, feelings, and behaviors around sleep. However, mental health professionals can tailor therapy for nightmares and, when appropriate, account for a coexisting mental health disorder.
Many types of psychotherapy also involve modifying detrimental patterns of behavior. Recommendations associated with talk therapy frequently involve changes to sleep hygiene, including daily routines and habits that facilitate consistent sleep.
Medication
Several types of prescription medications may be used to treat nightmare disorder. Most often, these are medications that affect the nervous system such as anti-anxiety, antidepressant, or antipsychotic drugs. Different medications may be used for people who have nightmares associated with PTSD.
Medications benefit some patients, but they can also come with side effects. For that reason, it is important to talk with a doctor who can describe the potential benefits and downsides of prescription drugs for nightmare disorder.
How To Stop Nightmares and Get Better Sleep
Whether nightmares are common or occasional, you may get relief from improving sleep hygiene. There are many elements of sleep hygiene, but some of the most important ones, especially in the context of nightmares, include:
- Following a consistent sleep schedule: Having a set bedtime and sleep schedule helps keep your sleep stable, preventing sleep avoidance and nightmare-inducing REM rebound after sleep deprivation.
- Utilizing relaxation methods: Finding ways to wind down, even basic deep breathing, can help decrease the stress and worry that give rise to nightmares.
- Avoiding caffeine and alcohol: Caffeine can stimulate your mind, which makes it harder to relax and fall asleep. Drinking alcohol close to bedtime can induce a REM rebound in the second half of the night that may worsen nightmares. As much as possible, it’s best to avoid alcohol and caffeine in the evening.
- Reducing screen time before bed: Using a smartphone, tablet, or laptop before bed can amp up your brain activity and make it difficult to fall asleep. If the screen time involves negative or worrying imagery, it may make nightmares more likely. To avoid this, create a bedtime routine with no screen time for an hour or more before going to sleep.
- Creating a comforting sleep environment: Your bedroom should promote a sense of calm with as few distractions or disruptions as possible. Set a comfortable temperature, block out excess light and sound, and set up your bed and bedding to be supportive and inviting.
Building better sleep habits is a component of many therapies for nightmare disorder and can pave the way for high-quality sleep on a regular basis. If you have persistent nightmares that interfere with your daily life, the first step is to talk with your doctor. Identifying and addressing an underlying cause can help make nightmares less frequent and less bothersome.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References
11 Sources
-
Paul, F., Schredl, M., & Alpers, G. W. (2015). Nightmares affect the experience of sleep quality but not sleep architecture: an ambulatory polysomnographic study. Borderline personality disorder and emotion dysregulation, 2, 3.
https://pubmed.ncbi.nlm.nih.gov/26401306/ -
American Academy of Sleep Medicine. (2014). The International Classification of Sleep Disorders – Third Edition (ICSD-3). Darien, IL
https://aasm.org/ -
Pagel, J. F. (2000). Nightmares and disorders of dreaming. American Family Physician, 61(7), 2037–2042, 2044.
https://pubmed.ncbi.nlm.nih.gov/10779247/ -
Schredl, M., & Reinhard, I. (2011). Gender differences in nightmare frequency: a meta-analysis. Sleep medicine reviews, 15(2), 115–121.
https://linkinghub.elsevier.com/retrieve/pii/S1087079210000638 -
Levin, R., & Nielsen, T. A. (2007). Disturbed dreaming, posttraumatic stress disorder, and affect distress: a review and neurocognitive model. Psychological bulletin, 133(3), 482–528.
http://doi.apa.org/getdoi.cfm?doi=10.1037/0033-2909.133.3.482 -
National Institute of Neurological Disorders and Stroke (NINDS). (2019, March 27). Hypersomnia information page.
https://www.ninds.nih.gov/Disorders/All-Disorders/Hypersomnia-Information-Page -
De Stasio, S., Boldrini, F., Ragni, B., & Gentile, S. (2020). Predictive Factors of Toddlers’ Sleep and Parental Stress. International journal of environmental research and public health, 17(7), 2494.
https://pubmed.ncbi.nlm.nih.gov/32268482/ -
Simor, P., Bódizs, R., Horváth, K., & Ferri, R. (2013). Disturbed dreaming and the instability of sleep: altered nonrapid eye movement sleep microstructure in individuals with frequent nightmares as revealed by the cyclic alternating pattern. Sleep, 36(3), 413–419.
https://pubmed.ncbi.nlm.nih.gov/23449753/ -
Gieselmann A, Ait Aoudia M, Carr M, et al. Aetiology and treatment of nightmare disorder: State of the art and future perspectives. J Sleep Res. 2019;28(4):e12820. doi:10.1111/jsr.12820
https://pubmed.ncbi.nlm.nih.gov/30697860/ -
Markov, D., Jaffe, F., & Doghramji, K. (2006). Update on Parasomnias: A Review for Psychiatric Practice. Psychiatry (Edgmont), 3(7), 69-76.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2958868/ -
Aurora, R. N., Zak, R. S., Auerbach, S. H., Casey, K. R., Chowdhuri, S., Karippot, A., Maganti, R. K., Ramar, K., Kristo, D. A., Bista, S. R., Lamm, C. I., Morgenthaler, T. I., Standards of Practice Committee, & American Academy of Sleep Medicine (2010). Best practice guide for the treatment of nightmare disorder in adults. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine, 6(4), 389–401.
https://jcsm.aasm.org/doi/full/10.5664/jcsm.27883




