When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Sleep Aids: Know the Types, Benefits, & Risks
- The best sleep aid depends on the cause of your sleep issues and any health conditions you may have.
- Over-the-counter sleep aids are typically antihistamines that have a sedative effect.
- Natural remedies, like diet and lifestyle changes, can promote better sleep and overall health.
- Talk to your doctor before taking a sleep aid and discuss any side effects concerning you.
Sleep problems are commonplace. In addition to disrupting sleep at night, these issues can have lasting effects on day-to-day life. To address sleep issues like insomnia, many people turn to sleep aids. These include prescription drugs, over-the-counter medications, and dietary supplements.
Every sleep aid has potential benefits and downsides, and it is important for individuals to be informed about their treatment options and talk with a doctor about the best option in their personal situation.
How Do Sleep Aids Work?
Most sleep aids work because they have a sedative effect, which means that they make you feel sleepy. That sleepiness may happen rapidly to help someone fall asleep, or it can have a prolonged effect to make it easier for them to sleep through the night.
The way that a sleep aid produces a sedative effect varies on its chemical composition. Depending on how they work and how they are regulated, sleeping pills can be organized into several distinct types.
Types of Sleep Aids
There are three types of sleep aids: prescription medications, over-the-counter drugs, and dietary supplements.
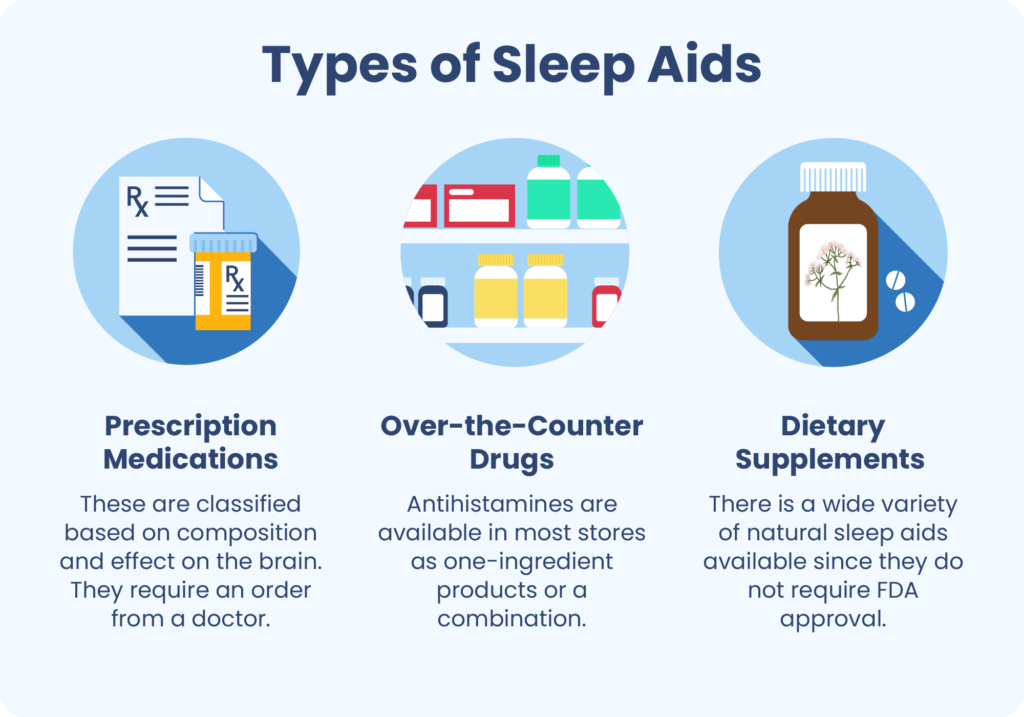
Prescription Drugs
Before a prescription drug can be sold, it must be approved by the Food and Drug Administration (FDA), which carefully reviews data from research studies about its effectiveness and safety. Once the drug is approved, doctors can prescribe them to patients.
Over-the-Counter Medications
Over-the-counter (OTC) medications can be purchased without a prescription. These medications do not go through the same level of FDA review as prescription medications, but they still must meet certain regulatory standards before they can be sold.
Over-the-counter sleep aids are typically composed of antihistamines. Antihistamines are frequently used to manage allergies, but because of their sedative effect, they are also marketed as sleeping pills.
Dietary Supplements
Although people may use them for health reasons, dietary supplements are not formal medications. They do not have to be approved by the FDA, and there is considerably less oversight of sleep aids sold as dietary supplements. Among the types of sleep aids, dietary supplements tend to have the least amount of evidence from studies documenting their benefits and downsides.
Potential Benefits of Sleep Aids
The primary benefit of most sleep aids is that they induce drowsiness to help you fall asleep or to increase the likelihood that you will stay asleep through the night.
By improving sleep in the short-term, many sleep aids may help alleviate daytime drowsiness and impaired thinking from sleep deprivation. They may help reset your sleep schedule, enabling you to get more consistent sleep.
That said, most sleep aids are not meant for long-term use. As a result, treatment for sleep disorders like insomnia often combines a sleep aid with practical steps, such as improving sleep hygiene, that can help you get quality sleep every night without relying on sleep medication.
Which Sleep Aids Work the Best?
Not everyone has the same reaction to a sleep aid, so there is no hard-and-fast rule about which one works the best. Instead, doctors suggest treatments based on the patient’s specific situation, including their symptoms and their overall health.
To make these suggestions, doctors may draw on guidance from expert organizations like the American Academy of Sleep Medicine (AASM). The AASM organizes panels of sleep experts who review the existing research and make general recommendations about sleep aids.
In the latest AASM guidelines for sleep aids for insomnia, certain prescription drugs are recommended depending on whether a person’s problem is with falling asleep or sleeping through the night. This is because certain sleep aids work quickly and wear off fast, and others start slowly and last a long time. The AASM recommends against the use of over-the-counter sleeping pills and dietary supplements like melatonin and valerian.
The safety and efficacy of supplements is not closely monitored by the U.S. Food and Drug Administration (FDA). Shoppers should take additional measures to make sure they are purchasing reputable products.
Potential Risks of Sleep Aids
Potential side effects can vary based on the specific sleep aid and whether the person taking it has any other health problems or medications that they take. In general, there are potential negative effects that can occur with almost all sleep medications, although the likelihood of these effects may be higher with some sleep aids.
- Lingering next-day effects:As many as 80% of people taking sleep aids say that the sedative effect may persist after they have woken up, creating excess drowsiness or slowed thinking when a person should be alert. This issue is most worrisome for people who drive in the morning and may be at a higher risk of auto accidents.
- Confusion or loss of coordination: A strong sedative effect can make a person feel confused, dizzy, or unable to concentrate. As a result, they may be at risk for falls or other accidents right before bed or during the night.
- Abnormal behavior: After taking sleep aids, some people engage in strange behavior while remaining partially asleep and unaware of their actions. This behavior can range from simple things like talking, to more complex actions like sleepwalking or trying to drive.
- Allergic reaction: These responses are rare, but some people have allergic reactions to sleep aids.
- Drug interaction: A sleep aid may interact with other medications and potentially change their potency or how they affect the body.
Are Sleep Aids Safe?
Sleep aids are usually considered safe for short-term use as long as they are used as directed. However, given the potential for side effects, it is always safest, regardless of the type of sleep aid, to take it under the guidance of a health care professional.
To reduce the risk of negative effects, it is important to take sleep aids safely. This generally means taking them at the right time and only with the recommended dosage. Extra doses should be avoided, even if sleeping problems continue. In addition, sleep aids should not be mixed with other sedatives, alcohol, or recreational drugs.

Medical Disclaimer: The content on this page should not be taken as medical advice or used as a recommendation for any specific treatment or medication. Always consult your doctor before taking a new medication or changing your current treatment.
References
5 Sources
-
A.D.A.M. Medical Encyclopedia. (2020, April 9). Medicines for sleep. MedlinePlus., Retrieved April 14, 2022, from
https://medlineplus.gov/ency/patientinstructions/000758.htm -
U.S. Food and Drug Administration (FDA). (2017, November 13). Prescription drugs and over-the-counter (OTC) drugs: Questions and answers., Retrieved April 14, 2022, from
https://www.fda.gov/drugs/questions-answers/prescription-drugs-and-over-counter-otc-drugs-questions-and-answers -
National Center for Complementary and Integrative Health. (2018, December). Using dietary supplements wisely., Retrieved April 14, 2022, from
https://www.nccih.nih.gov/health/using-dietary-supplements-wisely -
Sateia, M. J., Buysse, D. J., Krystal, A. D., Neubauer, D. N., & Heald, J. L. (2017). Clinical Practice Guideline for the Pharmacologic Treatment of Chronic Insomnia in Adults: An American Academy of Sleep Medicine Clinical Practice Guideline. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine, 13(2), 307–349.
https://pubmed.ncbi.nlm.nih.gov/27998379/ -
Fitzgerald, T., & Vietri, J. (2015). Residual Effects of Sleep Medications Are Commonly Reported and Associated with Impaired Patient-Reported Outcomes among Insomnia Patients in the United States. Sleep disorders, 2015, 607148.
https://pubmed.ncbi.nlm.nih.gov/26783470/