When you buy through our links, we may earn a commission. Products or services may be offered by an affiliated entity. Learn more.
Interrupted Sleep: Causes & Helpful Tips
- Interrupted sleep involves frequent awakenings during the night, disrupting the sleep cycle.
- Effects include daytime sleepiness, cognitive decline, mood disturbances, and health risks.
- Factors unique to the individual’s situation can interrupt sleep, like age, stress, and lifestyle.
- Optimizing your sleep routine and sleep environment can help prevent sleep interruptions.
When thinking about sleep and health, it’s common to focus on the issue of sleep quantity and whether we’re getting the recommended number of hours of sleep. While total sleep time is undoubtedly important, sleep continuity, or the ability to avoid interrupted sleep, is also critical.
Most people know that sleeping in stops and starts doesn’t feel as refreshing. Interrupted or fragmented sleep can contribute to insomnia, sleep deprivation, daytime sleepiness, and the numerous other potential consequences of insufficient sleep. Knowing more about the symptoms and causes of interrupted sleep can help you be informed about your situation and find the best treatments or preventative measures to minimize your sleep disturbances.
What Are the Symptoms of Interrupted Sleep?
For many people, the central symptom of interrupted sleep is easily noticeable: waking up from sleep one or more times during the course of the night (or during the day for people who work a night shift).
The timing and length of these wakeful episodes can vary. A person may have only a few breaks in sleep or several. They may be awake for just a few minutes or for an extended period before transitioning back to sleep. A person may experience restless sleep, tossing and turning or feeling only half-asleep without drifting off into deeper rest.
Not all cases of interrupted sleep, though, are readily apparent to the sleeper. For example, people with obstructive sleep apnea (OSA) have repeated lapses in breathing that cause brief arousals from deep sleep. These respiratory arousals are short enough that people with OSA don’t usually know that they are happening, but likely experience excessive daytime sleepiness as a result.
Why Does Interrupted Sleep Matter?
People who have interrupted sleep tend not to get enough overall sleep. Research has found a strong correlation between sleep continuity and total sleep time, indicating that people with disturbed sleep are at a higher risk of not sleeping enough hours. Not surprisingly, problems with sleep maintenance are a frequent complaint among people with insomnia. Insufficient sleep can cause daytime sleepiness that detracts from school or work performance and heightens the risk of accidents while driving or operating machinery.
Even when it doesn’t reduce sleep quantity, a mounting body of evidence points to the harm of interrupted sleep. During healthy sleep, a person progresses through a series of sleep cycles, each of which is made up of distinct sleep stages. Repeated interruptions and awakenings can disrupt that process, causing far-reaching effects of disrupted sleep on brain function, physical health, and emotional well-being.
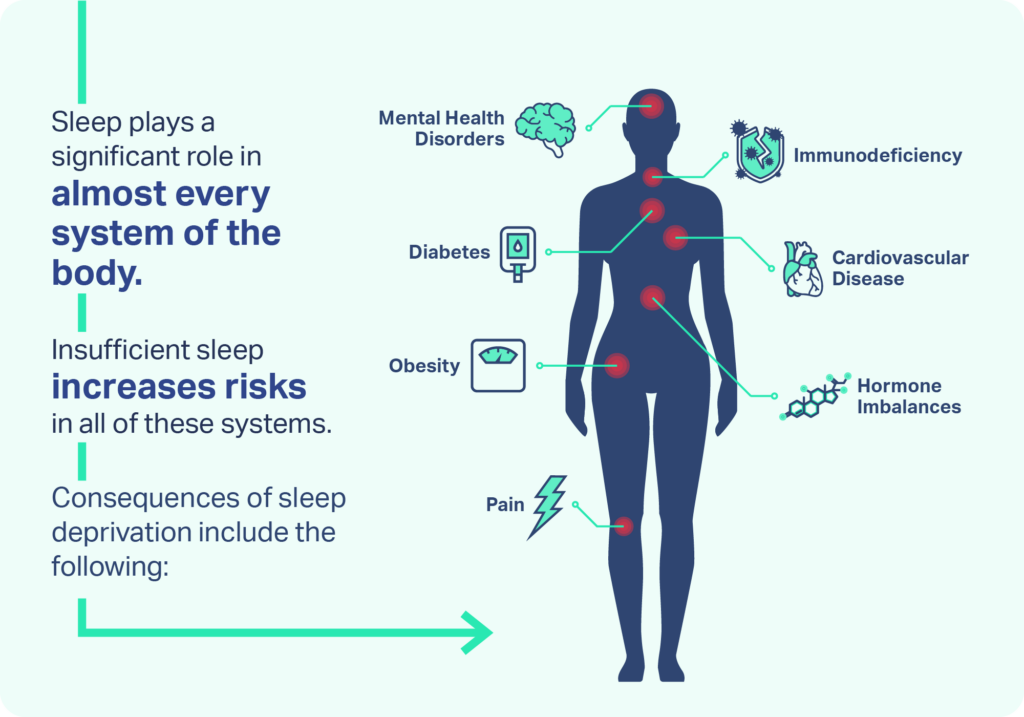
While the exact mechanisms underlying sleep’s role in brain health are not fully understood, research points to sleep continuity as important to thinking, memory, and decision-making. Sleep disruptions have also been associated with neurodegenerative disease including dementia and Parkinson’s disease. Fragmented sleep is considered to be an early symptom of these conditions, but research suggests that it may also be a contributing factor to their development.
In addition, repeated awakenings during sleep have been connected to mood disorders like depression. One study demonstrated a stronger correlation between interrupted sleep and a depressed mood compared to reduced total hours of continuous sleep. In addition, these issues were compounded with consecutive days of interrupted sleep, suggesting that the effect can accumulate over time.
Disrupted sleep can cause detrimental impacts on physical health as well. Otherwise healthy people have been found to have higher sensitivity to pain after just two nights of fragmented sleep. The long-term inability to proceed through each sleep stage combined with the activation of multiple systems of the body during repeated awakenings has been tied to higher rates of cardiovascular disease, weight gain, and metabolic problems including type 2 diabetes. All of these potential effects on the brain and body indicate that healthy sleep requires avoiding disruptions that inhibit sleep continuity.
What Causes Interrupted Sleep?
There are a wide-range of potential causes of interrupted sleep, and multiple factors may be involved in any specific person’s situation.
- Age: Sleep fragmentation is often a problem for older adults because they experience a natural change in their sleep patterns resulting in less time in deep sleep. With more time in light sleep stages, they are more easily awoken, leading to a greater number of disturbances and awakenings.
- Health: Disorders like restless legs syndrome (RLS) and bruxism are known to disrupt sleep. Other conditions, including nocturia, cardiovascular issues, as well as hormonal, lung, and neurological problems may threaten sleep continuity. Certain prescription drugs can have sleep-related side effects.
- Stress:Stress from a person’s personal or professional life may cause interrupted sleep, and anxiety, including worrying or ruminating about problems, may make it harder to get back to sleep after waking up. Parents with babies or young children can be awoken multiple times during the night, and caregivers for ill or disabled loved ones may confront similar challenges.
- Light: Changes to a person’s daylight exposure can throw off their circadian rhythm and make it hard to sleep continuously. This frequently occurs in people who have jet lag after intercontinental travel or who work the night shift and have to try to sleep during the day.
- Lifestyle: Scattered sleep schedules, excess consumption of alcohol or caffeine, and using electronic devices like cell phones in bed can disrupt a person’s sleep patterns. Too much light in the bedroom or excess noise, including from a partner’s snoring, may interfere with sleep.
When Should You Talk to a Doctor About Interrupted Sleep?
If you have interrupted sleep that has been going on for a long time, is persistent, or is worsening, you should talk with your doctor. You should also consult your doctor if you experience significant daytime sleepiness, mood changes during the day, or snoring, especially if it is loud and involves gasping for air.
It may be helpful to use a sleep diary to keep track of your symptoms including how often you experience interrupted sleep and how frequently you have excessive sleepiness during the day.
How Can You Prevent or Address Interrupted Sleep?
While not all causes of interrupted sleep are under your control, there are concrete steps that you can take to try to prevent interrupted sleep before it happens or address it if you’ve already found it to be a problem.
Sleep Hygiene Improvements
Sleep hygiene is a general term used to describe sleep-related habits and routines along with the sleep environment. Good sleep hygiene eliminates barriers to both falling asleep and staying asleep, making it easier to get solid nightly rest without distractions or disturbances.
Habits and Routines
A core element of sleep hygiene is making sure that your daily habits work to your benefit in promoting consistent sleep. Examples of healthy sleep tips to improve your habits include:
- Going to bed and waking up at the same time every day, including on weekends
- Following a steady routine before bed, including plenty of time to wind down and relax
- Avoiding alcohol, cigarettes, caffeine, and big meals in the evening, especially in the hours before bed
- Reducing your use of electronic devices before bed and avoiding them when in bed
- Getting outside or opening your blinds to get daily exposure to sunlight, especially in the morning
- Finding time to be physically active every day
Sleep Environment
To facilitate sleep continuity, you want to eliminate as many possible sources of sleep disturbances from your bedroom as you can:
- Use blackout curtains, a low-wattage bedside lamp, and if necessary, a sleep mask to avoid being bothered by excess light
- Wear ear plugs or use a white noise machine to block out noise
- Set your bedroom temperature to be comfortable, erring toward a cooler setting
- Make sure your mattress, pillows, blankets, and sheets are comfortable and inviting
- Talk to a bed partner or roommate if they snore, are restless, or otherwise cause potential sleep interruptions
Address Underlying Issues
Working with a health professional can help if your sleep is being interrupted by underlying sleep disorders or health problems. For example, treatment for obstructive sleep apnea can dramatically reduce sleep fragmentation in people with that condition. Addressing mental health disorders can frequently improve sleep issues like insomnia.

Still have questions? Ask our community!
Join our Sleep Care Community — a trusted hub of sleep health professionals, product specialists, and people just like you. Whether you need expert sleep advice for your insomnia or you’re searching for the perfect mattress, we’ve got you covered. Get personalized guidance from the experts who know sleep best.
References9 Sources
Kishi, A., Van Dongen, H. P., Natelson, B. H., Bender, A. M., Palombini, L. O., Bittencourt, L., Tufik, S., Ayappa, I., & Rapoport, D. M. (2017). Sleep continuity is positively correlated with sleep duration in laboratory nighttime sleep recordings. PloS one, 12(4), e0175504.
https://pubmed.ncbi.nlm.nih.gov/28394943/Van Someren, E. J., Cirelli, C., Dijk, D. J., Van Cauter, E., Schwartz, S., & Chee, M. W. (2015). Disrupted Sleep: From Molecules to Cognition. The Journal of neuroscience : the official journal of the Society for Neuroscience, 35(41), 13889–13895.
https://pubmed.ncbi.nlm.nih.gov/26468189/Wilckens, K. A., Woo, S. G., Kirk, A. R., Erickson, K. I., & Wheeler, M. E. (2014). Role of sleep continuity and total sleep time in executive function across the adult lifespan. Psychology and aging, 29(3), 658–665.
https://pubmed.ncbi.nlm.nih.gov/25244484/Abbott, S. M., & Videnovic, A. (2016). Chronic sleep disturbance and neural injury: links to neurodegenerative disease. Nature and science of sleep, 8, 55–61.
https://pubmed.ncbi.nlm.nih.gov/26869817/Lim, A. S., Kowgier, M., Yu, L., Buchman, A. S., & Bennett, D. A. (2013). Sleep Fragmentation and the Risk of Incident Alzheimer’s Disease and Cognitive Decline in Older Persons. Sleep, 36(7), 1027–1032.
https://pubmed.ncbi.nlm.nih.gov/23814339/Finan, P. H., Quartana, P. J., & Smith, M. T. (2015). The effects of sleep continuity disruption on positive mood and sleep architecture in healthy adults. Sleep, 38(11), 1735–1742.
https://pubmed.ncbi.nlm.nih.gov/26085289/Iacovides, S., George, K., Kamerman, P., & Baker, F. C. (2017). Sleep Fragmentation Hypersensitizes Healthy Young Women to Deep and Superficial Experimental Pain. The journal of pain : official journal of the American Pain Society, 18(7), 844–854.
https://linkinghub.elsevier.com/retrieve/pii/S1526590017304911Medic, G., Wille, M., & Hemels, M. E. (2017). Short- and long-term health consequences of sleep disruption. Nature and Science of Sleep, 9, 151–161.
https://pubmed.ncbi.nlm.nih.gov/28579842/Duffy, J. F., Scheuermaier, K., & Loughlin, K. R. (2016). Age-Related Sleep Disruption and Reduction in the Circadian Rhythm of Urine Output: Contribution to Nocturia?. Current aging science, 9(1), 34–43.
https://www.eurekaselect.com/137369/article